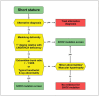
Molecular Pathogenesis
The short stature homeobox-containing gene (SHOX) is located within the pseudoautosomal region of the X (Xp22.3) and Y (Yp11.3) chromosomes. Although SHOX on the Y chromosome has been referred to as SHOXY, the official gene name, SHOX, does not refer to the chromosome on which it is located. Of note, SHOX escapes X-chromosome inactivation. The frequency with which pathogenic variants in SHOX occur on the X or Y chromosome is not known but is irrelevant, as this gene, located at the tip of the pseudoautosomal region, has an exchange rate of 50% in male meiosis [Kant et al 2011].
Gene structure.
SHOX encodes two major transcripts, SHOXa (NM_000451.3) and SHOXb (NM_006883.2), each containing five coding exons and differing only in their 3'UTR and a small region of the coding sequence [Rao et al 1997]. Meanwhile, further transcript variants have been described, suggesting that alternative splicing contributes to the regulation of SHOX expression [Durand et al 2011]. For a summary of gene and protein information, see Table A, Gene.
Pathogenic variants. More than 1,200 unique DNA variants and more than 180 pathogenic variants in SHOX have been described. An up-to-date list of these can be found on the Human Short Stature Gene Allelic Variant Database website (grenada.lumc.nl/LSDB_list/lsdbs/SHOX). (For more information, see Table A.)
The majority of SHOX pathogenic variants are large deletions encompassing the entire gene as well as adjacent genes.
Partial and complete duplications of SHOX have also been described [Benito-Sanz et al 2012, Sandoval et al 2014, van Duyvenvoorde et al 2014, Wit & Oostdijk 2015, Bunyan et al 2016, Benito-Sanz et al 2017, Hirschfeldova & Solc 2017, Upners et al 2017].
Normal gene product
Because there is no SHOX mouse ortholog, use of a mouse knockout model has not been possible [Clement-Jones et al 2000]. However, expression of human SHOXa cDNA under the control of a murine Col2a1 promoter and enhancer has been analyzed in transgenic mice [Beiser et al 2014]. Chicken SHOX models have also been a valuable model for limb development [Tiecke et al 2006, Sabherwal et al 2007, Durand et al 2010].
In human embryos SHOX is most strongly expressed in the mid-portion of limbs (especially the elbow and knee) and also in the distal ulna/radius and wrist [Clement-Jones et al 2000]. This expression pattern provides an explanation for the short stature, bowing, and shortening of the forearms and lower legs, the Madelung deformity, and the shortening of the fourth metacarpals seen in LWD and Turner syndrome [Clement-Jones et al 2000]. SHOX protein was also identified in human growth plate hypertrophic chondrocytes, further supporting a role for SHOX in bone development [Marchini et al 2004, Munns et al 2004].
SHOX is expressed in the first and second pharyngeal arches, suggesting that it may play a role in the development of the palatine maxillary sleeves, mandible, auricular ossicles, and the external auditory meatus [Clement-Jones et al 2000]. As such, haploinsufficiency of SHOX may cause the high-arched palate, micrognathia, and sensorineural deafness of Turner syndrome [Clement-Jones et al 2000].
SHOX acts as a nuclear transcription factor that inhibits cellular growth and apoptosis, possibly through the upregulation of p53 [Rao et al 2001, Blaschke et al 2003, Marchini et al 2004, Sabherwal et al 2004a, Sabherwal et al 2004b]. In the absence of normal SHOX, chondrocytes may undergo atypical proliferation and differentiation [Marchini et al 2004, Marchini et al 2007, Marchini et al 2016].
Direct and indirect targets of the SHOX transcription factor have been described. The targets BNP, FGFR3, and Ctgf are directly regulated by SHOX, whereas the regulation of Agc1 is indirect [Marchini et al 2007, Aza-Carmona et al 2011, Decker et al 2011, Beiser et al 2014].
An influence of SHOX as a regulator on FGFR3 signaling, CNP/Npr2 signaling and Bmp4 signaling and RUNX activity have been described (for a review see Marchini et al [2016]).
Abnormal gene product. The homeodomain of SHOX mediates several key functions including nuclear localization, DNA binding, and protein-protein interaction [Schneider et al 2005a]. Pathogenic variants within the homeodomain interfere with these processes and result in the skeletal defects. Pathogenic variants outside the homeodomain and deletions may lead to a reduced level of SHOX protein, thereby affecting growth and skeletal development.
Schneider et al [2005a] have shown that single missense pathogenic variants in SHOX, which were present in individuals with LWD or children with short stature of unknown cause (often called idiopathic short stature), alter the biologic function of SHOX with loss of DNA binding, dimerization, and/or nuclear localization [Schneider et al 2005a].
Recently, the first genetic modifier of SHOX deficiency, CYP26C1 (which is associated with a more severe phenotype), was described [Montalbano et al 2016]. Subsequently, pathogenic variants in CYP26C1 in the absence of pathogenic variants in SHOX have been associated with short stature [Montalbano et al 2018].