Continuing Education Activity
Malar rash, also named a butterfly rash, is a common facial presentation of multiple disorders. It is characterized by an erythematous flat or raised rash across the bridge of the nose and cheeks, which usually spares nasolabial folds. It may be transient or progress to involve other areas of facial skin. Malar rash may occur in several systemic and local diseases. Differential diagnoses for malar rash are as follows: systemic lupus erythematosus, cellulitis, rosacea, erysipelas, dermatomyositis, and pellagra. Treatment starts with sun protection and management of the underlying disease. This activity reviews the role of the interprofessional team in the evaluation and treatment of this condition.
Objectives:
- Identify the most common cause of the malar rash.
- Explain the importance of precise history and physical examination in the diagnosis of the underlying cause of the malar rash.
- Summarize the epidemiology of the most common cause of the malar rash.
- Review the importance of an interprofessional team approach to the evaluation and treatment of malar rash will provide the best outcome.
Introduction
Malar rash, also named a butterfly rash, is a common facial presentation of multiple disorders.[1] characterized by an erythematous flat or raised rash across the bridge of the nose and cheeks, which usually spares nasolabial folds. It may be transient or progress to involve other areas of facial skin.[2]
This is mainly seen in patients with systemic lupus erythematosus. As per the American College of Rheumatology, Malar rash is one of the criteria for systemic lupus erythematosus (SLE); it may also be present with other types of lupus including discoid lupus and subacute cutaneous lupus.[2]
Differential diagnoses for malar rash are as follows: systemic lupus erythematosus, cellulitis, rosacea, erysipelas, dermatomyositis, and pellagra.
Treatment starts with sun protection, including appropriate clothing, sunscreens, and behavior change and management of the underlying disease.
Etiology
Malar rash may occur in several systemic and local diseases.[3]
Common causes of malar rash are as follows:
- Erysipelas
- Cellulitis
- Systemic lupus erythematosus
- Rosacea
- Pellagra
- Dermatomyositis
Erysipelas
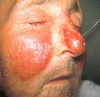
Erysipelas is a type of skin infection that involves superficial lymphatics and upper dermis. The classic manifestation includes a painful, rapidly progressive, well-circumscribed, erythematous, shiny plaque accompanied by perifollicular edema and swelling (peau d’orange). Clinical presentations include acute onset of systemic symptoms, including fever, chills, and malaise.[4][5]
Cellulitis
Cellulitis is a skin infection that involves subcutaneous fat and deeper dermis. It is different from erysipelas in that it is less well-demarcated with little or no edema, and does not usually have systemic symptoms. In the presence of systemic symptoms, the course of the disease is more indolent.[3]
Lupus or SLE
The systemic lupus erythematosus (SLE) is an autoimmune disease that involves multiple organs in which the immune system produces numerous auto-antibodies that attack different tissues such as kidneys, joints, skin, brain, and heart. It can vary from mild rashes and arthritis to debilitating fever, joint pain fatigue, or severe organ damage and life-threatening disease.[6]
Rosacea
Rosacea is a chronic inflammatory acneiform disease that involves facial area, especially in the middle age. Rosacea is considered as the most common cause of the malar rash. It usually occurs in fair-skin patients and involves the cheeks, chin, nose, forehead, eyelids, and nose. Classic findings include erythema, telangiectasia, and pustules or papules with no comedones. The rash of rosacea may be accompanied by episodes of flushing triggered by hot drinks, stress, or alcohol. Genetic factors and extrinsic factors are involved in the pathogenesis of the disease. Rosacea never causes systemic illness.[7]
Pellagra
Pellagra is a systemic disease that results from a cellular niacin deficiency. It is defined by 4 “D’s”: dermatitis, dementia, diarrhea, and death. Dermatitis related to pellagra is a bilateral symmetric eruption on sun-exposed areas of the skin. During the acute phase, it may be painful to touch and eventually can become so striking clinically. In the absence of characteristic cutaneous manifestations, making the diagnosis of pellagra would be difficult.[8][9][10]
Dermatomyositis
Dermatomyositis (DM) is an idiopathic inflammatory myopathy that affecting individuals of all ages. DM has multiple classic skin manifestations, of which poikiloderma is the most important. Poikiloderma is characterized by a tetrad of hyperpigmentation, hypopigmentation, epidermal atrophy, and telangiectasias. Poikiloderma may be seen in various dermatologic disorders and is not specific to DM, but it has a typical distribution on the sun-exposed areas of the skin, including face and eyelids, elbows, knees, knuckles, chest, and back. The poikiloderma in DM is more violaceous in color in contrast to the poikiloderma in SLE.[11][12]
Epidemiology
Cellulitis and Erysipelas
Since cellulitis and Erysipelas is not a reportable disorder, the exact prevalence is not clear; however, it is a common infection, involving all different racial and ethnic groups.
Rosacea
Rosacea is a chronic inflammatory facial disorder with a worldwide prevalence of 5.46%.[13] Fair-skinned Caucasians with sun-sensitive skin (skin phototypes I and II) seem to have the highest risk for rosacea.[14][15] The prevalence of rosacea in the fair-skinned population is estimated from 2 to 22 percent.[13]
Lupus or SLE
The Lupus Foundation of America has the estimation of the prevalence of at least 1.5 million cases. In a study of worldwide prevalence and incidence of SLE, the highest prevalence and incidence of SLE were in North America (241/100 000 and 23.2/100 000 person-years, respectively). Lower incidence of SLE was detected in Ukraine and Africa (0.3/100 000 person-years), and the lowest prevalence was reported in Northern Australia (0 cases in 847 people). Women were more commonly affected than men in every age and ethnic group. People of African ethnicity had the greatest prevalence and incidence of SLE, whereas those of the White race had the lowest prevalence and incidence. The annual incidence of SLE from the 1970s to 2000s has been estimated from approximately 1 to 10 per 100,000 population, while the SLE prevalence has been ranged from 5.8 to 130 per 100,000 population.[16]
Pellagra
In the United States, the incidence of pellagra is not clear. Pellagra epidemics no longer occur. Sporadic cases of pellagra may be seen in patients with malabsorption disorders, patients with alcoholism, individuals dependent on illegal drugs and food faddists. [17] [18] [19]
Dermatomyositis
The incidence of dermatomyositis is estimated as 9.63 cases per million of the population. Dermatomyositis has a bimodal age distribution; one peak at 5 to 15 years and the other one at 45 to 60 years.[11]
Histopathology
Cellulitis
Histopathologic findings include vascular and lymphatic dilatation with marked edema in the dermal and subepidermal areas. Dense and diffuse neutrophil infiltration is usually seen beneath edema.[20]
Erysipelas
Histopathologic evaluation reveals significant dermal edema, vascular dilatation, and bacterial invasion to the lymphatics and connective tissue. Blood vessel invasion is rarely seen.
Dermatomyositis and SLE
The main histopathologic findings of dermatomyositis and SLE are epidermal thinning, basal layer with hydropic degeneration, and disrupted dermo-epidermal junction; upper dermis edema; sparse lymphocyte infiltration in the dermis; and connective tissue with fibrinoid degeneration. On direct immunofluorescence microscopy, deposition of immunoglobulin G (IgG), immunoglobulin M (IgM), and C3 are detected at the basement membrane in both involved and uninvolved skin of SLE patients which is not true for patients with dermatomyositis.[21]
Rosacea
Histopathologic findings of rosacea include dilated vessels, lymphohistiocytic infiltration in perifollicular and perivascular area, neutrophils in intrafollicular area, and edema. Sebaceous gland hyperplasia, expansion of connective tissue, and elastosis are also seen.[22]
Pellagra
Microscopic findings of pellagra are nonspecific and almost similar to other nutritional deficiencies, which include acanthosis, hyperkeratosis, and parakeratosis. Psoriasiform hyperplasia may also be detected. Other histopathologic findings are ballooning keratinocytes and increased melanin in the upper epidermis, perivascular inflammatory infiltrate, and telangiectasia.[23]
History and Physical
Malar rash can occur in several systemic and local disorders. Diagnosing the underlying condition in which malar rash has been resulted from may be difficult due to the wide range of probable causes. A full and detailed clinical history and investigation of all symptoms, as well as a thorough physical examination, should be done by the clinicians to make the appropriate diagnosis.
Evaluation
Evaluation of a malar rash is based on the causative condition.
Cellulitis and Erysipelas
In general, no laboratory workup is required for uncomplicated cases of erysipelas and cellulitis. In toxic patients, laboratory blood test like complete blood count (CBC) with differential, erythrocyte sedimentation rate ( ESR) and C-reactive protein (CRP) is recommended.
SLE
Malar rash of systemic lupus erythematosus may precede other symptoms of SLE by months and years or may appear along with other symptoms of acute SLE. laboratory findings in isolated malar rash are similar to SLE such as positive ANA, CRP, ESR. Histopathologic examination of the skin will support the laboratory tests.
Dermatomyositis
Diagnosis of a malar rash of dermatomyositis in a patient with no clinical signs of muscle disease is a skin biopsy. Patients with the only clinical presentation of skin disease should be evaluated for concomitant muscle disease. Patients should be evaluated every 2 to 3 months for serum CK level and aldolase along with muscle examination.
Rosacea
The diagnosis is made clinically.
Pellagra
The diagnosis of pellagra is based on clinical presentation and response to niacin (Vitamin B3) treatment. the laboratory tests that support the diagnosis of pellagra are as follows: Blood count (anemia), hypoproteinemia, low phosphorus, high level of calcium, low serum niacin level, NADP and NAD levels. low urinary levels of N-methyl nicotinamide.
Treatment / Management
Management of a malar or butterfly rash is based on the causative condition.
Cellulitis and Erysipelas
The mainstay of the management includes oral or intravenous antibiotic therapy.
SLE and Dermatomyositis
Treatment starts with sun protection, including appropriate clothing, sunscreens, and behavior change. Next lines of treatment include topical or intralesional corticosteroids, antimalarial medications, and immunosuppressive agents.
Rosacea
Treatment may include gels or creams to repair the skin and decrease redness, as well as antibiotic therapy to control the inflammation.
Pellagra
Oral niacin or nicotinamide is usually effective in resolving the clinical symptoms of pellagra.
Differential Diagnosis
Common differential diagnoses of the malar rash are as follow:
- Cellulitis
- Dermatomyositis
- Erysipelas
- Pellagra
- Rosacea
- Systemic lupus erythematosus
Prognosis
Causative conditions of malar rash have a wide variety of morbidity and mortality. Malar rash due to erysipelas and cellulitis improves with proper antibiotic therapy. Rosacea has a chronic progressive or relapsing course in some patients. Prognosis of SLE and dermatomyositis mainly depends on the disease activity. Pellagra has an excellent prognosis with appropriate treatment.
Consultations
Consultation may be appropriate with dermatology, rheumatology, or infectious disease.
Deterrence and Patient Education
Treatment and management of malar rash are different based on the condition which causes it. In general, patients with cellulitis, erysipelas, and pellagra will improve with proper treatment. Patients with rosacea might have a course of remission and relapse, and multiple dermatology follows up might be needed. Patients with SLE and dermatomyositis diseases need rheumatology to follow up.
Enhancing Healthcare Team Outcomes
Many diseases can cause a malar rash. However, it is essential to perform a proper history and physical exam because the diagnosis may not be straight forward. These patients will present to the nurse practitioner, primary care provider, dermatologist, and rheumatologist. An interprofessional team approach to the evaluation and treatment of malar rash will provide the best outcome.

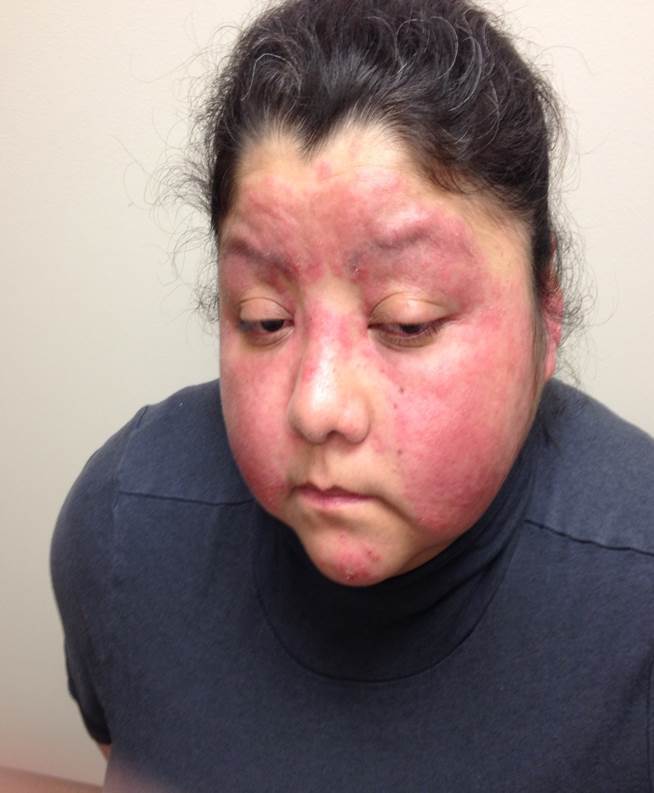
Figure
Rash, Face. Rash on the face presents on bilateral cheeks with sparing of the nasolabial folds. Contributed by Scott Jones, MD
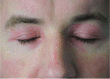
Figure
Dermatomyositis rash Photograph courtesy of Dr Mark Tarnopolsky, McMaster University, Hamilton, Canada.
References
- 1.
- Dreizen S. The butterfly rash and the malar flush. What diseases do these signs reflect? Postgrad Med. 1991 Jan;89(1):225-8, 233-4. [PubMed: 1824645]
- 2.
- Uva L, Miguel D, Pinheiro C, Freitas JP, Marques Gomes M, Filipe P. Cutaneous manifestations of systemic lupus erythematosus. Autoimmune Dis. 2012;2012:834291. [PMC free article: PMC3410306] [PubMed: 22888407]
- 3.
- O'Connor K, Paauw D. Erysipelas: rare but important cause of malar rash. Am J Med. 2010 May;123(5):414-6. [PubMed: 20399315]
- 4.
- Celestin R, Brown J, Kihiczak G, Schwartz RA. Erysipelas: a common potentially dangerous infection. Acta Dermatovenerol Alp Pannonica Adriat. 2007 Sep;16(3):123-7. [PubMed: 17994173]
- 5.
- Stulberg DL, Penrod MA, Blatny RA. Common bacterial skin infections. Am Fam Physician. 2002 Jul 01;66(1):119-24. [PubMed: 12126026]
- 6.
- Askanase A, Shum K, Mitnick H. Systemic lupus erythematosus: an overview. Soc Work Health Care. 2012;51(7):576-86. [PubMed: 22905974]
- 7.
- Blount BW, Pelletier AL. Rosacea: a common, yet commonly overlooked, condition. Am Fam Physician. 2002 Aug 01;66(3):435-40. [PubMed: 12182520]
- 8.
- Tyler I, Wiseman MC, Crawford RI, Birmingham CL. Cutaneous manifestations of eating disorders. J Cutan Med Surg. 2002 Jul-Aug;6(4):345-53. [PubMed: 11951131]
- 9.
- Karthikeyan K, Thappa DM. Pellagra and skin. Int J Dermatol. 2002 Aug;41(8):476-81. [PubMed: 12207761]
- 10.
- Isaac S. The "gauntlet" of pellagra. Int J Dermatol. 1998 Aug;37(8):599. [PubMed: 9732006]
- 11.
- Bendewald MJ, Wetter DA, Li X, Davis MD. Incidence of dermatomyositis and clinically amyopathic dermatomyositis: a population-based study in Olmsted County, Minnesota. Arch Dermatol. 2010 Jan;146(1):26-30. [PMC free article: PMC2886726] [PubMed: 20083689]
- 12.
- Strowd LC, Jorizzo JL. Review of dermatomyositis: establishing the diagnosis and treatment algorithm. J Dermatolog Treat. 2013 Dec;24(6):418-21. [PubMed: 22686682]
- 13.
- Spoendlin J, Voegel JJ, Jick SS, Meier CR. A study on the epidemiology of rosacea in the U.K. Br J Dermatol. 2012 Sep;167(3):598-605. [PubMed: 22564022]
- 14.
- Rainer BM, Fischer AH, Luz Felipe da Silva D, Kang S, Chien AL. Rosacea is associated with chronic systemic diseases in a skin severity-dependent manner: results of a case-control study. J Am Acad Dermatol. 2015 Oct;73(4):604-8. [PubMed: 26256428]
- 15.
- Tan J, Berg M. Rosacea: current state of epidemiology. J Am Acad Dermatol. 2013 Dec;69(6 Suppl 1):S27-35. [PubMed: 24229634]
- 16.
- Rees F, Doherty M, Grainge MJ, Lanyon P, Zhang W. The worldwide incidence and prevalence of systemic lupus erythematosus: a systematic review of epidemiological studies. Rheumatology (Oxford). 2017 Nov 01;56(11):1945-1961. [PubMed: 28968809]
- 17.
- Lorentzen HF, Fugleholm AM, Weismann K. [Zinc deficiency and pellagra in alcohol abuse]. Ugeskr Laeger. 2000 Dec 11;162(50):6854-6. [PubMed: 11187143]
- 18.
- Lu JY, Yu CL, Wu MZ. Pellagra in an immunocompetent patient with cytomegalovirus colitis. Am J Gastroenterol. 2001 Mar;96(3):932-4. [PubMed: 11280594]
- 19.
- Kertesz SG. Pellagra in 2 homeless men. Mayo Clin Proc. 2001 Mar;76(3):315-8. [PubMed: 11243279]
- 20.
- Drucker AM, Piguet V. Hot Stuff: Thermal Imaging Aids in Cellulitis Diagnosis. J Invest Dermatol. 2018 Mar;138(3):482-484. [PubMed: 29477190]
- 21.
- Kazandjieva J, Tsankov N, Pramatarov K. The red face revisited: connective tissue disorders. Clin Dermatol. 2014 Jan-Feb;32(1):153-8. [PubMed: 24314389]
- 22.
- Lee WJ, Jung JM, Lee YJ, Won CH, Chang SE, Choi JH, Moon KC, Lee MW. Histopathological Analysis of 226 Patients With Rosacea According to Rosacea Subtype and Severity. Am J Dermatopathol. 2016 May;38(5):347-52. [PubMed: 26460622]
- 23.
- Sato M, Matsumura Y, Kojima A, Nakashima C, Katoh M, Kore-Eda S, Miyachi Y. Pellagra-like erythema on sun-exposed skin of patients with anorexia nervosa. J Dermatol. 2011 Oct;38(10):1037-40. [PubMed: 21592198]
Disclosure: Sara Naji Rad declares no relevant financial relationships with ineligible companies.
Disclosure: Priyanka Vashisht declares no relevant financial relationships with ineligible companies.
Publication Details
Author Information and Affiliations
Authors
Sara Naji Rad1; Priyanka Vashisht.Affiliations
Publication History
Last Update: September 4, 2023.
Copyright
This book is distributed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International (CC BY-NC-ND 4.0) ( http://creativecommons.org/licenses/by-nc-nd/4.0/ ), which permits others to distribute the work, provided that the article is not altered or used commercially. You are not required to obtain permission to distribute this article, provided that you credit the author and journal.
Publisher
StatPearls Publishing, Treasure Island (FL)
NLM Citation
Naji Rad S, Vashisht P. Malar Rash. [Updated 2023 Sep 4]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024 Jan-.