Continuing Education Activity
Eczema, also known as atopic dermatitis, is a common chronic skin condition that can lead to recurrent infections and poor quality of life if left untreated. This activity reviews the evaluation and management of eczema and highlights the role of interprofessional teams in improving outcomes for patients with this condition.
Objectives:
- Review the pathophysiology of eczema.
- Outline the adverse effects of poorly controlled eczema.
- Summarize the treatment options for eczema.
- Describe the importance of improving care coordination amongst the interprofessional team to improve outcomes for patients with eczema.
Introduction
Eczema, also known as atopic dermatitis, is the most common form of dermatitis. Genetic as well as environmental factors are thought to play a part in the pathogenesis. Eczema is most commonly seen in children but can be seen in adults. People with the disease tend to have dry, itchy skin that is prone to infection. Eczema is commonly known as the "itch that rashes" due to dry skin that leads to a rash as a result of scratching or rubbing. The most important treatment of eczema is skin hydration followed by topical steroids for flare-ups.
Etiology
People with eczema have a dysfunctional barrier which causes various problems. The cells that make up our skin are essential for optimal skin hydration. People with eczema tend to have dry skin due to the dysfunction in the skin barrier. Water can more easily escape from the skin leading to dehydrated skin. People with eczema are also more susceptible to infection. Harmful substances can more readily penetrate the skin due to the dysfunction. People with atopic dermatitis tend to have a skewed inflammatory immune response, and their skin is easily irritated by fragrances and allergens.
Epidemiology
The lifetime prevalence of atopic dermatitis is about 15-30% in children and 2-10% in adults. About 60% of cases will develop within the first year of life. The prevalence of atopic dermatitis is more common in rural rather than urban areas. This incidence which emphasizes the link to lifestyle and environment factors in the mechanisms of AD. Atopic dermatitis is apart of the triad known as the 'Atopic march.' This relates to the association between patients with atopic dermatitis, asthma, and allergic rhinitis. About 50% of patients with severe atopic dermatitis will develop asthma, and 75% will develop allergic rhinitis.[1]
Pathophysiology
Research shows there is a genetic component to atopic dermatitis. One common mutation has been observed in the gene Filaggrin, a vital gene for skin cell maturity. This gene is responsible for creating the tough, flat corneocytes that form the outermost protective layer of skin. In a patient with normal skin cells, the corneocytes are tightly packed in an organized manner. A patient with a filaggrin mutation will have a dysfunctional skin barrier due to the haphazard organization of the skin cells.[2] This dysfunction causes a 'leaky' skin barrier allowing water loss and decreased protection from harmful substances. People with eczema also have reduced numbers of beta-defensins in the skin. Beta-defensins are host defense peptides that are vital for fighting off certain bacteria, viruses, and fungi. A decrease in these peptides leads to increased colonization and infection, especially with staph aureus.[3]
Histopathology
The histopathology seen in atopic dermatitis is non-specific. In the acute phase lesions, characterized by intensely pruritic, erythematous papules, histopathology reveals mild epidermal hyperplasia, infiltrations of lymphocytes and macrophages along the venous plexus in the dermis and intercellular edema of the epidermis (spongiosis). Lesions biopsied in chronic atopic dermatitis, which are characterized by lichenification and fibrotic papules, may reveal increased hyperplasia and hyperkeratosis of the skin. There is also persistent dermal inflammatory cell infiltrate with lymphocytes and macrophages. The chronic phase lacks the edema or spongiosis that is present in acute phase lesions.
History and Physical
Acutely the rash will be intensely pruritic with erythematous papules and excoriations. As the person continues to itch and rub the skin, the skin starts to thicken and on physical exam, there may be lichenification (thickening of the skin with exaggeration of the typical skin markings due to scratching or rubbing).
The distribution of the rash seen in atopic dermatitis will vary depending on the age of the person. Infants tend to have widely distributed, dry, scaly and erythematous patches with small excoriations. They also tend to have involvement of their face, especially the cheeks. As the child ages, the rash becomes more localized. Areas affected will include the extensors surfaces such as the wrists, elbows, ankles, and knees. School-aged children tend to follow the pattern that is seen in adults. This pattern includes the involvement of the flexural surfaces usually affecting the anti-cubital and popliteal fosse.
Other physical exam findings besides the appearance of a rash may indicate a person has eczema. Examination of the face may reveal Dennie-Morgan lines. These are crease-like wrinkles just below the lower eyelid. This exam finding can be seen in up to 25% of patients with eczema. People with eczema may have co-existing pityriasis alba and have hypopigmented patches or fine scaling plaques more commonly seen on the face. On examination of the hands, there may be an increased number and depth of skin lines known as hyperlinear palms. People that have eczema and allergic rhinitis may have a transverse crease formed across their nose. This line is referred to as the "allergic salute" and is caused by habitually rubbing the nose in an upward manner.[4]
Evaluation
Diagnosis is typically clinical based on the appearance of the rash and history. Routine labwork is not usually indicated. If unsure of the diagnosis, allergy testing and patch testing may be performed.
Treatment / Management
The main management and treatment of atopic dermatitis include hydration and topical anti-inflammatory medications for flare-ups. The priority in treatment is focusing on a daily skin moisturizing regimen with a fragrance-free ointment that has limited preservatives.[5] An ointment is preferred over a cream due to the high proportion of oil to water in lotions. Patients/parents should also identify and address any triggers. They should be instructed to avoid any environmental allergens, harsh soaps, and detergents, fragrances as well as rough or non-breathable fabrics. Skin flare-ups can be treated with topical anti-inflammatory medications, such as topical steroids or steroid-free products like pimecrolimus, tacrolimus or Eucirsa. In children, itching tends to be worse at nighttime. Oral antihistamines can be used to intermittently at bedtime for disturbed sleep due to itch however antihistamines are no longer recommended for daytime use for itching in eczema. Patients with poorly controlled atopic dermatitis have a higher risk of cutaneous infections. Patients/parents may be instructed to do dilute bleach baths or intranasal mupirocin to decrease the number of cutaneous infections.[6]
Differential Diagnosis
The differential diagnosis for atopic dermatitis includes may eczematous dermatitides including:[7]
- Contact dermatitis
- Cutaneous fungal infections
- Seborrheic dermatitis
- Drug eruptions
- Scabies
- Psoriasis
- Ectodermal dysplasia
- Hyper IgE syndrome
- Netherton's syndrome
- Wiskott-Aldrich syndrome
Toxicity and Adverse Effect Management
It is crucial that the patient and parents understand that the use of topical steroids should only be used for active lesions. They can also be used prophylactically by applying the topical steroid a few times a week to prevent flare-ups. Topical steroids should not be routinely used daily. Long term use of topical steroids can cause atrophy (thinning of the skin), stretch marks (striae), acne, telangiectasia and rebound dermatitis/rosacea. The strength and formulation of the topical steroid need to be carefully determined based on the location of the body affected. Less potent steroids should be used on the face and intertriginous regions.
Prognosis
Most children will 'outgrow' eczema, and their symptoms will be resolved by adulthood. However, children with the already persistent disease, later onset, and/or more severe disease have increased persistence.[8]
Complications
Due to the dysfunctional skin barrier seen in atopic dermatitis, patients are at increased risk for infection from bacterial, viral, and fungal pathogens.[9] About 10% of healthy individuals are colonized with S. aureus compared to over 90% of AD patients.[10] The density of S. aureus colonization correlates with the severity of dermatitis.[11] Infection with staph aureus may cause furuncles, impetigo or cellulitis. Patients with repeated bacterial infections may require treatment with dilute bleach baths and intranasal mupirocin to reduce the number of bacteria on their skin.
Patients with atopic dermatitis are also more susceptible to viral infections. Eczema herpeticum is a life-threatening infection caused by herpes simplex virus-1. Patients present with widespread blisters, fever, and fatigue. The blisters appear in clusters and can cover a large area of the body. Eczema herpeticum is a medical emergency with complications including keratoconjunctivitis, meningitis, encephalitis or secondary bacterial sepsis.[12]
Another life-threatening viral infection seen in patients with atopic dermatitis is eczema cosackium.[9] Eczema cosackium is a variant of hand, foot, and mouth disease that is classically associated with the enterovirus coxsackievirus A16. Instead of the typical presentation of blisters and erosions located on the hands, feet, and hard palate, patients with AD have widespread blisters and abrasions that tend to appear in regions previously affected by atopic dermatitis. The rash can appear similar to eczema herpeticum. However, patients will lack fevers, decreased appetite or fatigue. Parents may report a brief history of diarrhea or fever a week before the rash appears. Rare complications include aseptic meningitis.
Deterrence and Patient Education
It is essential to determine the triggers for a patient with atopic dermatitis. Reduction or elimination of these triggers is an important step in the treatment of atopic dermatitis. Patients may see an improvement in their skin and reduced flare-ups if they avoid allergens (commonly dust mites, egg, peanuts, milk, fish, soy, rice, and wheat) and irritants (particularly chemicals, heat, soaps, humidity, acrylic, and wool).
Enhancing Healthcare Team Outcomes
A team-based approach is essential for the care of a patient with atopic dermatitis, especially in moderate to severe cases. Eczema is a common condition seen in pediatric and family medicine offices. Typically patients with mild to moderate eczema can be treated in the office by their primary care provider with standard therapy. Patients with moderate to severe cases may require referral to dermatology for systemic treatments. If a patient is not responding to typical treatment regimens, they may benefit from a consult with an allergist for a patch or skin scratch testing. an interprofessional team of a specialty trained dermatology nurse and specialty-trained dermatology clinician will provide the best patient care. [Level 5]

Figure
Eczema, Craquele DermNet New Zealand
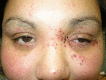
Figure
Eczema, Herpeticum DermNet New Zealand
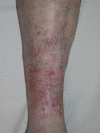
Figure
Venous Eczema DermNet New Zealand

Figure
Lick Eczema Contributed by Dr. Shyam Verma, MBBS, DVD, FRCP, FAAD, Vadodara, India
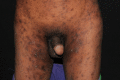
Figure
Eczematised Scabies Contributed by Dr. Shyam Verma, MBBS, DVD, FRCP, FAAD, Vadodara, India
References
- 1.
- Eichenfield LF, Tom WL, Chamlin SL, Feldman SR, Hanifin JM, Simpson EL, Berger TG, Bergman JN, Cohen DE, Cooper KD, Cordoro KM, Davis DM, Krol A, Margolis DJ, Paller AS, Schwarzenberger K, Silverman RA, Williams HC, Elmets CA, Block J, Harrod CG, Smith Begolka W, Sidbury R. Guidelines of care for the management of atopic dermatitis: section 1. Diagnosis and assessment of atopic dermatitis. J Am Acad Dermatol. 2014 Feb;70(2):338-51. [PMC free article: PMC4410183] [PubMed: 24290431]
- 2.
- Tsakok T, Woolf R, Smith CH, Weidinger S, Flohr C. Atopic dermatitis: the skin barrier and beyond. Br J Dermatol. 2019 Mar;180(3):464-474. [PubMed: 29969827]
- 3.
- Clausen ML, Edslev SM, Andersen PS, Clemmensen K, Krogfelt KA, Agner T. Staphylococcus aureus colonization in atopic eczema and its association with filaggrin gene mutations. Br J Dermatol. 2017 Nov;177(5):1394-1400. [PubMed: 28317091]
- 4.
- Mevorah B, Frenk E, Wietlisbach V, Carrel CF. Minor clinical features of atopic dermatitis. Evaluation of their diagnostic significance. Dermatologica. 1988;177(6):360-4. [PubMed: 3234581]
- 5.
- Kamińska E. [The role of emollients in atopic dermatitis in children]. Dev Period Med. 2018;22(4):396-403. [PMC free article: PMC8522819] [PubMed: 30636240]
- 6.
- Siegfried EC, Hebert AA. Diagnosis of Atopic Dermatitis: Mimics, Overlaps, and Complications. J Clin Med. 2015 May 06;4(5):884-917. [PMC free article: PMC4470205] [PubMed: 26239454]
- 7.
- Kim JP, Chao LX, Simpson EL, Silverberg JI. Persistence of atopic dermatitis (AD): A systematic review and meta-analysis. J Am Acad Dermatol. 2016 Oct;75(4):681-687.e11. [PMC free article: PMC5216177] [PubMed: 27544489]
- 8.
- Ong PY, Leung DY. Bacterial and Viral Infections in Atopic Dermatitis: a Comprehensive Review. Clin Rev Allergy Immunol. 2016 Dec;51(3):329-337. [PubMed: 27377298]
- 9.
- Ong PY, Leung DY. The infectious aspects of atopic dermatitis. Immunol Allergy Clin North Am. 2010 Aug;30(3):309-21. [PMC free article: PMC2913147] [PubMed: 20670815]
- 10.
- Gong JQ, Lin L, Lin T, Hao F, Zeng FQ, Bi ZG, Yi D, Zhao B. Skin colonization by Staphylococcus aureus in patients with eczema and atopic dermatitis and relevant combined topical therapy: a double-blind multicentre randomized controlled trial. Br J Dermatol. 2006 Oct;155(4):680-7. [PubMed: 16965415]
- 11.
- Wetzel S, Wollenberg A. [Eczema herpeticatum]. Hautarzt. 2004 Jul;55(7):646-52. [PubMed: 15150652]
- 12.
- Kantor R, Thyssen JP, Paller AS, Silverberg JI. Atopic dermatitis, atopic eczema, or eczema? A systematic review, meta-analysis, and recommendation for uniform use of 'atopic dermatitis'. Allergy. 2016 Oct;71(10):1480-5. [PMC free article: PMC5228598] [PubMed: 27392131]
Disclosure: Valerie Nemeth declares no relevant financial relationships with ineligible companies.
Disclosure: Justin Evans declares no relevant financial relationships with ineligible companies.
Publication Details
Author Information and Affiliations
Authors
Valerie Nemeth; Justin Evans1.Affiliations
Publication History
Last Update: August 8, 2022.
Copyright
This book is distributed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International (CC BY-NC-ND 4.0) ( http://creativecommons.org/licenses/by-nc-nd/4.0/ ), which permits others to distribute the work, provided that the article is not altered or used commercially. You are not required to obtain permission to distribute this article, provided that you credit the author and journal.
Publisher
StatPearls Publishing, Treasure Island (FL)
NLM Citation
Nemeth V, Evans J. Eczema. [Updated 2022 Aug 8]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024 Jan-.




