Attribution Statement: LactMed is a registered trademark of the U.S. Department of Health and Human Services.
NCBI Bookshelf. A service of the National Library of Medicine, National Institutes of Health.
Drugs and Lactation Database (LactMed®) [Internet]. Bethesda (MD): National Institute of Child Health and Human Development; 2006-.
CASRN: 104206-65-7
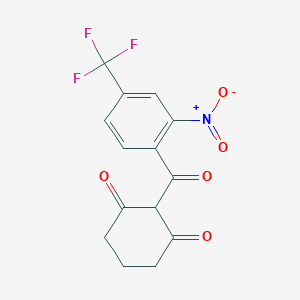
Drug Levels and Effects
Summary of Use during Lactation
Blood levels in two exclusively breastfed infants of one mother were far below the therapeutic range and dropped from the initial postpartum measurement to levels taken during the second week of breastfeeding. The infants had no adverse reactions and grew normally. If nitisinone is required by the mother, it is not a reason to discontinue breastfeeding. Until more data are available, monitoring the breastfed infant’s blood nitisinone, tyrosine and succinylacetone concentrations might be advisable.[1]
Drug Levels
Maternal Levels. Relevant published information was not found as of the revision date.
Infant Levels. A mother was taking nitisinone 40 mg daily for type-1 tyrosinemia during pregnancy and breastfeeding. The infant’s mother breastfed exclusively for 2 weeks. Two days postpartum, the infant’s blood nitisinone concentration was 10.9 micromoles/L. Because of the drug’s long half-life of 54 hours, this concentration was probably from transplacental passage. The blood level dropped to 1.7 micromoles/L at about 10 days postpartum and at 6 weeks, nitisinone was undetectable (<0.1 micromoles/L ) in the infant’s blood. A second infant of the same mother was born when the mother was taking nitisinone 80 mg daily. The infant was exclusively breastfed exclusively for 2 weeks. The infant’s blood nitisinone concentration was 5 micromoles/L on day 5 of life, 1.7 micromoles/L at about day 12 of life and undetectable on day 24 of life. All of the measured infant blood levels were far below the therapeutic reference range for infants of 30 to 60 micromoles/L.[1]
Effects in Breastfed Infants
A patient with type-1 tyrosinemia was taking nitisinone 40 mg daily or 0.44 mg/kg daily in addition to a low tyrosine and phenylalanine diet. She continued on this regimen during her first pregnancy and postpartum. In her second pregnancy, the nitisinone dosage was increased to 60 mg daily in the week 11 of pregnancy, to 80 mg daily in the week 28 and continued at that dosage postpartum. Both infants were exclusively breastfed for 2 weeks postpartum. They showed no adverse reactions and grew normally.[1]
Effects on Lactation and Breastmilk
Relevant published information was not found as of the revision date.
References
- 1.
- Zöggeler T, Ramoser G, Höller A, et al. Nitisinone treatment during two pregnancies and breastfeeding in a woman with tyrosinemia type 1 - a case report. J Pediatr Endocrinol Metab. 2022;35:259–65. [PubMed: 34506697]
Substance Identification
Substance Name
Nitisinone
CAS Registry Number
104206-65-7
Disclaimer: Information presented in this database is not meant as a substitute for professional judgment. You should consult your healthcare provider for breastfeeding advice related to your particular situation. The U.S. government does not warrant or assume any liability or responsibility for the accuracy or completeness of the information on this Site.
- User and Medical Advice Disclaimer
- Drugs and Lactation Database (LactMed) - Record Format
- LactMed - Database Creation and Peer Review Process
- Fact Sheet. Drugs and Lactation Database (LactMed)
- Drugs and Lactation Database (LactMed) - Glossary
- LactMed Selected References
- Drugs and Lactation Database (LactMed) - About Dietary Supplements
- Breastfeeding Links
- PubChem SubstanceRelated PubChem Substances
- PubMedLinks to PubMed
- Nitisinone treatment during two pregnancies and breastfeeding in a woman with tyrosinemia type 1 - a case report.[J Pediatr Endocrinol Metab. 2022]Nitisinone treatment during two pregnancies and breastfeeding in a woman with tyrosinemia type 1 - a case report.Zöggeler T, Ramoser G, Höller A, Jörg-Streller M, Janzen N, Ramoni A, Scholl-Bürgi S, Karall D. J Pediatr Endocrinol Metab. 2022 Feb 23; 35(2):259-265. Epub 2021 Sep 10.
- Validation of a therapeutic range for nitisinone in patients treated for tyrosinemia type 1 based on reduction of succinylacetone excretion.[JIMD Rep. 2019]Validation of a therapeutic range for nitisinone in patients treated for tyrosinemia type 1 based on reduction of succinylacetone excretion.Jack RM, Scott CR. JIMD Rep. 2019 Mar; 46(1):75-78. Epub 2019 Mar 14.
- Review Diazoxide.[Drugs and Lactation Database (...]Review Diazoxide.. Drugs and Lactation Database (LactMed®). 2006
- Clinical utilization of dried blood spot nitisinone (NTBC) and succinylacetone (SA) concentrations in hereditary tyrosinaemia type 1 - A UK centre experience.[Ann Clin Biochem. 2020]Clinical utilization of dried blood spot nitisinone (NTBC) and succinylacetone (SA) concentrations in hereditary tyrosinaemia type 1 - A UK centre experience.Yeo M, Turner C, Dalton NR, Rahman Y, Vara R. Ann Clin Biochem. 2020 Nov; 57(6):412-419. Epub 2020 Sep 30.
- Review Levetiracetam.[Drugs and Lactation Database (...]Review Levetiracetam.. Drugs and Lactation Database (LactMed®). 2006
- Nitisinone - Drugs and Lactation Database (LactMed®)Nitisinone - Drugs and Lactation Database (LactMed®)
Your browsing activity is empty.
Activity recording is turned off.
See more...
