NCBI Bookshelf. A service of the National Library of Medicine, National Institutes of Health.
National Guideline Centre (UK). Emergency and acute medical care in over 16s: service delivery and organisation. London: National Institute for Health and Care Excellence (NICE); 2018 Mar. (NICE Guideline, No. 94.)

Emergency and acute medical care in over 16s: service delivery and organisation.
Show detailsChapter 35Discharge planning
35. Discharge planning
35.1. Introduction
Planning for a patient’s discharge from hospital is a key aspect of effective care. Many patients who are discharged from hospital will have ongoing care needs that must be met in the community. This ongoing care comes in many forms, including the use of specialised equipment at home such as a hospital-type bed, daily support from carers to complete the activities of daily living, or regular visits from district nurses to administer medication.
There is a wide variety of care available in the community, but it needs to be planned in advance of the patient’s return home, to ensure that there is no gap in the provision of care between the discharge from hospital and the initiation of community services. Furthermore, information about the patient must be handed over from the hospital team to the community team so an informed plan of care can be put into place.
Discharge planning is the process by which the hospital team considers what support might be required by the patient in the community, refers the patient to these services, and then liaises with these services to manage the patient’s discharge. Poor discharge planning can lead to poor patient outcomes and delayed discharge planning can cause patients to remain in hospital longer than necessary, taking up valuable inpatient beds when they could be more easily and comfortably cared for in the community.
While the guideline committee affirmed the value of discharge planning based on experience, they wanted to review any evidence available about the efficacy and cost implications of discharge planning for patients following an acute medical emergency.
35.2. Review question: Does discharge planning facilitate early hospital discharge?
For full details see review protocol in Appendix A.
Table 1
PICO characteristics of review question.
35.3. Clinical evidence
Ten studies (11 papers) were included in the review;8,16,23,32,33,36,42,52,53,59,64 these are summarised in Table 2 below. Evidence from these studies is summarised in the clinical evidence summary below (Table 3). See also the study selection flow chart in Appendix B, forest plots in Appendix C, study evidence tables in Appendix D, GRADE tables in Appendix F and excluded studies list in Appendix G.
Table 2
Summary of studies included in the review.
Table 3
Clinical evidence summary: Discharge planning versus standard processes.
35.4. Economic evidence
Published literature
No relevant health economic studies were identified.
The economic article selection protocol and flow chart for the whole guideline can found in the guideline’s Appendix 41A and Appendix 41B.
35.5. Evidence statements
Clinical
Ten studies comprising 3,271 people evaluated the role of discharge planning for improving outcomes in secondary care in adults and young people at risk of an AME, or with a suspected or confirmed AME. The evidence suggested that discharge planning may provide a benefit in reduced avoidable adverse events expressed as falls (1 study, very low quality), length of stay (5 studies, moderate quality), quality of life SF-12 mental ratings (1 study, very low quality) patient and/or carer satisfaction defined as preparedness to leave hospital (1 study, low quality). The evidence suggested there was no effect on quality of life (St Georges Respiratory questionnaire and SF-12 physical ratings) (1 study, low to very low quality), staff satisfaction (1 study, low quality) avoidable adverse events defined as adverse medicine reaction (1 study, very low quality) and patient and/or carer satisfaction (1 study, very low quality).
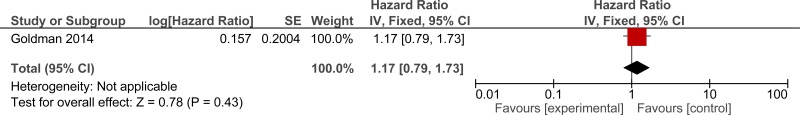
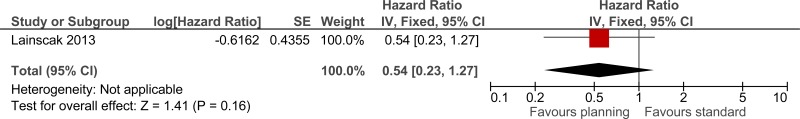
The evidence suggested a benefit for discharge planning in reducing readmissions in 3 studies (low quality) but in 1 study that reported a hazard ratio there was no difference in readmission (very low quality). The evidence suggested a benefit for discharge planning in reducing mortality at 6 months (1 study, very low quality) and during admission (1 study, very low quality). However, evidence from 4 studies suggested an increase in mortality from 5 days-12months (moderate quality).
Economic
No relevant economic evaluations were identified.
35.6. Recommendations and link to evidence
| Recommendations |
|
| Research recommendation | - |
| Relative values of different outcomes | Mortality, avoidable adverse events, quality of life, patient and/or carer satisfaction and length of stay were considered by the committee to be critical outcomes to decision making. Readmission, delayed transfers of care and staff satisfaction were considered important outcomes. |
| Trade-off between benefits and harms |
A total of 10 studies were identified that assessed the role of discharge planning for improving outcomes in secondary care in adults and young people at risk of an AME, or with a suspected or confirmed AME. The evidence suggested that discharge planning may provide a benefit in reduced avoidable adverse events (falls), length of stay, quality of life (as measured by SF-12 mental rating in 1 study) and patient and/or carer satisfaction measured by the preparedness to leave hospital. The evidence suggested there was no effect on quality of life (as measured by either the St Georges Respiratory questionnaire or SF-12 physical ratings), staff satisfaction and patient and/or carer satisfaction assessed by patient rating of the discharge process. Discharge planning was beneficial in terms of reducing readmissions in 3 studies but in 1 study that reported a hazard ratio that there was no difference in readmission. The evidence from 1 study reporting results only as hazard rations suggested a benefit for reduced mortality at 6 months and another study suggested reduced in hospital mortality for discharge planning. However, evidence from 3 studies suggested an increase in mortality from 1 day -12 months. It should also be noted that 2 of the studies23,59 in the meta-analysis suggesting an increase in mortality post discharge; discharge planning were small studies and there is evidence to suggest that the frailty of the patients in the discharge planning groups was more pronounced than in the control group which may explain the excess mortality in the study groups. No evidence was identified for delayed transfers of care. The discharge planning interventions evaluated by the studies varied in terms of their composition and focus. Whereas some were grounded in facilitating the organisation of community, social care and living arrangements, others were more focused on improving post-discharge management of clinical conditions through patient education and management of follow-up appointments and prescriptions. Some interventions also included post-discharge components such as follow-up telephone calls and visits. However, despite these differences, pooled analyses showed no significant heterogeneity. The committee felt that if no plan for discharge is made, it can result in bed blocking if a patient is medically fit for discharge, but is unable to be discharged because the appropriate community and social care measures, if required, are not in place. This plan should be made on admission to enable adequate time to make arrangements for the point where the patient is medically ready for discharge. Therefore, the committee decided to make a recommendation based on the evidence and their wide experience within primary, secondary and community care. |
| Trade-off between net effects and costs |
No economic studies were included. One of the studies included above found substantial cost savings but this has not been included since (as outlined in the review protocol) the US setting is unlikely to make the economic findings generalisable to the UK. Unit costs of ED attendances and hospital admissions were provided to aid the consideration of cost-effectiveness. The review above indicated a reduction in readmissions and length of stay associated with discharge planning, which could result in substantial costs savings. The committee noted that implementing a form of early discharge planning is likely to be low cost and therefore it is likely to be cost saving overall. Safeguards need to be in place to ensure that earlier discharge is safe and the patients have appropriate support in the community. |
| Quality of evidence |
The evidence was graded very low to moderate quality due to risk of bias, imprecision and indirectness. There was no economic evidence included in the review. |
| Other considerations |
The committee considered current practice with regard to discharge planning. Discharge planning of some form occurs throughout all hospitals in the UK but is not standardised across hospitals. Although it is stated that it should begin at the point of admission (and before admission in the case of elective admission), this often does not happen. The Department of Health has guidelines and a tool for discharge planning.57 Discharges are divided into ‘simple’ and ‘complex’. Simple discharges account for 80% of discharges and should be easily achieved with the appropriate training, planning and resources. The processes to achieve a simple discharge are predictable and reproducible. In these cases, when the discharge process does not occur as planned, it is most likely to be a consequence of a failure in communication. Complex discharges account for the remaining 20%. These are patients with more complex needs such as multimorbidity or frailty, who may need additional input from other professionals such as social workers and therapists. The involvement of additional services, staff and specialties makes prior co-ordination and planning even more critical. This is of particular importance in the frail elderly and those patients with mental health issues. These patient groups are vulnerable to poor communication and co-ordination which have a disproportionate impact on the discharge process. Doctors are not usually specifically trained in discharge planning. It is assumed that they gain knowledge and skills through clinical practice. Training in discharge planning would benefit doctors early in their career and junior nursing staff so that it is embedded in the management plan. The committee decided to make a positive recommendation as they considered it good practice to start planning discharge at the point of admission. This would ensure that discharge gets equal prominence with the ongoing management of the acute illness which should mitigate the risk of delayed discharge once the patient is fit to return to the community. |
References
- 1.
- Altfeld SJ, Shier GE, Rooney M, Johnson TJ, Golden RL, Karavolos K et al. Effects of an enhanced discharge planning intervention for hospitalized older adults: a randomized trial. Gerontologist. 2013; 53(3):430–440 [PubMed: 22961467]
- 2.
- Anderson C, Ni Mhurchu C, Brown PM, Carter K. Stroke rehabilitation services to accelerate hospital discharge and provide home-based care: an overview and cost analysis. Pharmacoeconomics. 2002; 20(8):537–552 [PubMed: 12109919]
- 3.
- Atienza F, Anguita M, Martinez-Alzamora N, Osca J, Ojeda S, Almenar L et al. Multicenter randomized trial of a comprehensive hospital discharge and outpatient heart failure management program. European Journal of Heart Failure. 2004; 6(5):643–652 [PubMed: 15302014]
- 4.
- Azzalini L, Sole E, Sans J, Vila M, Duran A, Gil-Alonso D et al. Feasibility and safety of an early discharge strategy after low-risk acute myocardial infarction treated with primary percutaneous coronary intervention: the EDAMI pilot trial. Cardiology. 2015; 130(2):120–129 [PubMed: 25612789]
- 5.
- Balaban RB, Weissman JS, Samuel PA, Woolhandler S. Redefining and redesigning hospital discharge to enhance patient care: a randomized controlled study. Journal of General Internal Medicine. 2008; 23(8):1228–1233 [PMC free article: PMC2517968] [PubMed: 18452048]
- 6.
- Beech R, Rudd AG, Tilling K, Wolfe CD. Economic consequences of early inpatient discharge to community-based rehabilitation for stroke in an inner-London teaching hospital. Stroke. 1999; 30(4):729–735 [PubMed: 10187870]
- 7.
- Braet A, Weltens C, Vleugels A. Effectiveness of discharge interventions from hospital to home to reduce readmissions: a systematic review. JBI Database of Systematic Reviews and Implementation Reports. 2012; 10:S105–S117 [PubMed: 27820399]
- 8.
- Chan B, Goldman LE, Sarkar U, Schneidermann M, Kessell E, Guzman D et al. The effect of a care transition intervention on the patient experience of older multi-lingual adults in the safety net: results of a randomized controlled trial. Journal of General Internal Medicine. 2015; 30(12):1788–1794 [PMC free article: PMC4636586] [PubMed: 25986136]
- 9.
- Clemson L, Lannin NA, Wales K, Salkeld G, Rubenstein L, Gitlin L et al. Occupational therapy predischarge home visits in acute hospital care: a randomized trial. Journal of the American Geriatrics Society. 2016; 64(10):2019–2026 [PubMed: 27603152]
- 10.
- Cotton MM, Bucknall CE, Dagg KD, Johnson MK, MacGregor G, Stewart C et al. Early discharge for patients with exacerbations of chronic obstructive pulmonary disease: a randomized controlled trial. Thorax. 2000; 55(11):902–906 [PMC free article: PMC1745631] [PubMed: 11050257]
- 11.
- Cunliffe AL, Gladman JRF, Husbands SL, Miller P, Dewey ME, Harwood RH. Sooner and healthier: a randomised controlled trial and interview study of an early discharge rehabilitation service for older people. Age and Ageing. 2004; 33(3):246–252 [PubMed: 15082429]
- 12.
- Davies CWH, Wimperis J, Green ES, Pendry K, Killen J, Mehdi I et al. Early discharge of patients with pulmonary embolism: a two-phase observational study. European Respiratory Journal. 2007; 30(4):708–714 [PubMed: 17567672]
- 13.
- Domingo GRR, Reyes FC, Thompson FV, Johnson PM, Shortridge-Baggett LM. Effectiveness of structured discharge process in reducing hospital readmission of adult patients with community acquired pneumonia: a systematic review. JBI Library of Systematic Reviews. 2012; 10(18):1086–1121 [PubMed: 27820311]
- 14.
- Durvasula R, Kayihan A, Del Bene S, Granich M, Parker G, Anawalt BD et al. A multidisciplinary care pathway significantly increases the number of early morning discharges in a large academic medical center. Quality Management in Health Care. 2015; 24(1):45–51 [PubMed: 25539490]
- 15.
- Early Supported Discharge Trialists. Services for reducing duration of hospital care for acute stroke patients. Cochrane Database of Systematic Reviews. 2001; Issue 2:CD000443. DOI:10.1002/14651858.CD000443 [PubMed: 10796365] [CrossRef]
- 16.
- Evans RL, Hendricks RD. Evaluating hospital discharge planning: a randomized clinical trial. Medical Care. 1993; 31(4):358–370 [PubMed: 8464252]
- 17.
- Farren EA. Effects of early discharge planning on length of hospital stay. Nursing Economics. 1991; 9(1):25–63 [PubMed: 1899919]
- 18.
- Finn KM, Heffner R, Chang Y, Bazari H, Hunt D, Pickell K et al. Improving the discharge process by embedding a discharge facilitator in a resident team. Journal of Hospital Medicine. 2011; 6(9):494–500 [PubMed: 22042739]
- 19.
- Fjaertoft H, Indredavik B, Johnsen R, Lydersen S. Acute stroke unit care combined with early supported discharge. Long-term effects on quality of life. A randomized controlled trial. Clinical Rehabilitation. 2004; 18(5):580–586 [PubMed: 15293492]
- 20.
- Fox M. Nurse-led early discharge planning for chronic disease reduces hospital readmission rates and all-cause mortality. Evidence-Based Nursing. 2016; 19(2):62 [PubMed: 26701748]
- 21.
- Fox MT, Persaud M, Maimets I, Brooks D, O’Brien K, Tregunno D. Effectiveness of early discharge planning in acutely ill or injured hospitalized older adults: a systematic review and meta-analysis. BMC Geriatrics. 2013; 13:70 [PMC free article: PMC3707815] [PubMed: 23829698]
- 22.
- George S, Atwal A. Discharge planning reduces length of stay and re-admission rates for older people admitted with a medical condition. Australian Occupational Therapy Journal. 2013; 60(5):375–376 [PubMed: 24089992]
- 23.
- Goldman LE, Sarkar U, Kessell E, Guzman D, Schneidermann M, Pierluissi E et al. Support from hospital to home for elders: a randomized trial. Annals of Internal Medicine. 2014; 161(7):472–481 [PubMed: 25285540]
- 24.
- Goncalves-Bradley DC, Lannin NA, Clemson LM, Cameron ID, Shepperd S. Discharge planning from hospital. Cochrane Database of Systematic Reviews. 2016; Issue 1:CD000313. DOI:10.1002/14651858.CD000313.pub5 [PMC free article: PMC7073416] [PubMed: 26816297] [CrossRef]
- 25.
- Haggmark C, Nilsson B. Effects of an intervention programme for improved discharge-planning. Nordic Journal of Nursing Research. 1997; 17(2):4–8
- 26.
- Harrison LL. Patient education in early postpartum discharge programs. MCM American Journal of Maternal Child Nursing. 1990; 15(1):39 [PubMed: 2153889]
- 27.
- Harrison MB, Browne GB, Roberts J, Tugwell P, Gafni A, Graham ID. Quality of life of individuals with heart failure: a randomized trial of the effectiveness of two models of hospital-to-home transition. Medical Care. 2002; 40(4):271–282 [PubMed: 12021683]
- 28.
- Hesselink G, Schoonhoven L, Barach P, Spijker A, Gademan P, Kalkman C et al. Improving patient handovers from hospital to primary care: a systematic review. Annals of Internal Medicine. 2012; 157(6):417–428 [PubMed: 22986379]
- 29.
- Hofstad H, Gjelsvik BEB, Naess H, Eide GE, Skouen JS. Early supported discharge after stroke in Bergen (ESD Stroke Bergen): three and six months results of a randomised controlled trial comparing two early supported discharge schemes with treatment as usual. BMC Neurology. 2014; 14(1):239 [PMC free article: PMC4301654] [PubMed: 25528166]
- 30.
- Hyde CJ, Robert IE, Sinclair AJ. The effects of supporting discharge from hospital to home in older people. Age and Ageing. 2000; 29(3):271–279 [PubMed: 10855913]
- 31.
- Indredavik B, Fjaertoft H, Ekeberg G, Loge AD, Morch B. Benefit of an extended stroke unit service with early supported discharge: a randomized, controlled trial. Stroke. 2000; 31(12):2989–2994 [PubMed: 11108761]
- 32.
- Jack BW, Chetty VK, Anthony D, Greenwald JL, Sanchez GM, Johnson AE et al. A reengineered hospital discharge program to decrease rehospitalization: a randomized trial. Annals of Internal Medicine. 2009; 150(3):178–187 [PMC free article: PMC2738592] [PubMed: 19189907]
- 33.
- Jennings JH, Thavarajah K, Mendez MP, Eichenhorn M, Kvale P, Yessayan L. Predischarge bundle for patients with acute exacerbations of COPD to reduce readmissions and ED visits: a randomized controlled trial. Chest. 2015; 147(5):1227–1234 [PubMed: 25940250]
- 34.
- Kleinpell RM. Randomized trial of an intensive care unit-based early discharge planning intervention for critically ill elderly patients. American Journal of Critical Care. 2004; 13(4):335–345 [PubMed: 15293587]
- 35.
- Kotowycz MA, Cosman TL, Tartaglia C, Afzal R, Syal RP, Natarajan MK. Safety and feasibility of early hospital discharge in ST-segment elevation myocardial infarction - a prospective and randomized trial in low-risk primary percutaneous coronary intervention patients (the Safe-Depart Trial). American Heart Journal. 2010; 159(1):117 [PubMed: 20102876]
- 36.
- Lainscak M, Kadivec S, Kosnik M, Benedik B, Bratkovic M, Jakhel T et al. Discharge coordinator intervention prevents hospitalizations in patients with COPD: a randomized controlled trial. Journal of the American Medical Directors Association. 2013; 14(6):450–456 [PubMed: 23623520]
- 37.
- Langhorne P, Taylor G, Murray G, Dennis M, Anderson C, Bautz-Holter E et al. Early supported discharge services for stroke patients: a meta-analysis of individual patients’ data. The Lancet. 2005; 365(9458):501–506 [PubMed: 15705460]
- 38.
- Langhorne P, Holmqvist LW, Early Supported Discharge Trialists. Early supported discharge after stroke. Journal of Rehabilitation Medicine. 2007; 39(2):103–108 [PubMed: 17351690]
- 39.
- Laramee AS, Levinsky SK, Sargent J, Ross R, Callas P. Case management in a heterogeneous congestive heart failure population: a randomized controlled trial. Archives of Internal Medicine. 2003; 163(7):809–817 [PubMed: 12695272]
- 40.
- Legrain S, Tubach F, Bonnet-Zamponi D, Lemaire A, Aquino JP, Paillaud E et al. A new multimodal geriatric discharge-planning intervention to prevent emergency visits and rehospitalizations of older adults: the optimization of medication in AGEd multicenter randomized controlled trial. Journal of the American Geriatrics Society. 2011; 59(11):2017–2028 [PubMed: 22091692]
- 41.
- Linden A, Butterworth S. A comprehensive hospital-based intervention to reduce readmissions for chronically ill patients: a randomized controlled trial. American Journal of Managed Care. 2014; 20(10):783–792 [PubMed: 25365681]
- 42.
- Lindpaintner LS, Gasser JT, Schramm MS, Cina-Tschumi B, Muller B, Beer JH. Discharge intervention pilot improves satisfaction for patients and professionals. European Journal of Internal Medicine. 2013; 24(8):756–762 [PubMed: 24075842]
- 43.
- Lockwood KJ, Taylor NF, Harding KE. Pre-discharge home assessment visits in assisting patients’ return to community living: a systematic review and meta-analysis. Journal of Rehabilitation Medicine. 2015; 47(4):289–299 [PubMed: 25782842]
- 44.
- Mahler SA, Riley RF, Hiestand BC, Russell GB, Hoekstra JW, Lefebvre CW et al. The HEART Pathway randomized trial: identifying emergency department patients with acute chest pain for early discharge. Circulation: Cardiovascular Quality and Outcomes. 2015; 8(2):195–203 [PMC free article: PMC4413911] [PubMed: 25737484]
- 45.
- Mazloum SR, Heidari-Gorji MA, Bidgoli-Gholkhatmi M, Agayei N. Effectiveness of discharge-planning on physical quality of life of patients with ischemic heart disease. International Journal of Applied and Basic Medical Research. 2016; 6(2):129–133 [PMC free article: PMC4830153] [PubMed: 27127744]
- 46.
- McClellan CM, Cramp F, Powell J, Benger JR. A randomised trial comparing the cost effectiveness of different emergency department healthcare professionals in soft tissue injury management. BMJ Open. 2013; 3(1):e001116 [PMC free article: PMC3549250] [PubMed: 23293239]
- 47.
- McInnes E, Mira M, Atkin N, Kennedy P, Cullen J. Can GP input into discharge planning result in better outcomes for the frail aged: results from a randomized controlled trial. Family Practice. 1999; 16(3):289–293 [PubMed: 10439984]
- 48.
- McNamee P, Christensen J, Soutter J, Rodgers H, Craig N, Pearson P et al. Cost analysis of early supported hospital discharge for stroke. Age and Ageing. 1998; 27(3):345–351
- 49.
- Melberg T, Jorgensen M, Orn S, Solli T, Edland U, Dickstein K. Safety and health status following early discharge in patients with acute myocardial infarction treated with primary PCI: a randomized trial. European Journal of Preventive Cardiology. 2015; 22(11):1427–1434 [PubMed: 25398704]
- 50.
- Mistiaen P, Francke AL, Poot E. Interventions aimed at reducing problems in adult patients discharged from hospital to home: a systematic meta-review. BMC Health Services Research. 2007; 7:47 [PMC free article: PMC1853085] [PubMed: 17408472]
- 51.
- Moher D, Weinberg A, Hanlon R, Runnalls K. Effects of a medical team coordinator on length of hospital stay. CMAJ Canadian Medical Association Journal. 1992; 146(4):511–515 [PMC free article: PMC1488427] [PubMed: 1737315]
- 52.
- Naughton BJ, Moran MB, Feinglass J, Falconer J, Williams ME. Reducing hospital costs for the geriatric patient admitted from the emergency department: a randomized trial. Journal of the American Geriatrics Society. 1994; 42(10):1045–1049 [PubMed: 7930327]
- 53.
- Naylor M, Brooten D, Jones R, Lavizzo-Mourey R, Mezey M, Pauly M. Comprehensive discharge planning for the hospitalized elderly. A randomized clinical trial. Annals of Internal Medicine. 1994; 120(12):999–1006 [PubMed: 8185149]
- 54.
- Naylor MD, Brooten D, Campbell R, Jacobsen BS, Mezey MD, Pauly MV et al. Comprehensive discharge planning and home follow-up of hospitalized elders: a randomized clinical trial. JAMA - Journal of the American Medical Association. 1999; 281(7):613–620 [PubMed: 10029122]
- 55.
- Naylor MD, McCauley KM. The effects of a discharge planning and home follow-up intervention on elders hospitalized with common medical and surgical cardiac conditions. Journal of Cardiovascular Nursing. 1999; 14(1):44–54 [PubMed: 10533691]
- 56.
- Nazareth I, Burton A, Shulman S, Smith P, Haines A, Timberal H. A pharmacy discharge plan for hospitalized elderly patients-a randomized controlled trial. Age and Ageing. 2001; 30(1):33–40 [PubMed: 11322670]
- 57.
- NHS Institute for Innovation and Improvement. Quality and service improvement tools: discharge planning, 2008. Available from: http://webarchive
.nationalarchives http://www.gov.uk/20121108093302/ .institute .nhs.uk/quality_and_service _improvement_tools /quality_and_service _improvement_tools /discharge_planning.html - 58.
- Palmer HC, Armistead NS, Elnicki DM, Halperin AK, Ogershok PR, Manivannan S et al. The effect of a hospitalist service with nurse discharge planner on patient care in an academic teaching hospital. American Journal of Medicine. 2001; 111(8):627–632 [PubMed: 11755506]
- 59.
- Pardessus V, Puisieux F, Di Pompeo C, Gaudefroy C, Thevenon A, Dewailly P. Benefits of home visits for falls and autonomy in the elderly: a randomized trial study. American Journal of Physical Medicine and Rehabilitation. 2002; 81(4):247–252 [PubMed: 11953541]
- 60.
- Parfrey PS, Gardner E, Vavasour H, Harnett JD, McManamon C, McDonald J et al. The feasibility and efficacy of early discharge planning initiated by the admitting department in two acute care hospitals. Clinical and Investigative Medicine Medecine Clinique Et Experimentale. 1994; 17(2):88–96 [PubMed: 8004854]
- 61.
- Parkes J, Shepperd S. Discharge planning from hospital to home. Cochrane Database of Systematic Reviews. 2000; Issue 4:CD000313. DOI:10.1002/14651858.CD000313 [PubMed: 11034682] [CrossRef]
- 62.
- Phillips CO, Wright SM, Kern DE, Singa RM, Shepperd S, Rubin HR. Comprehensive discharge planning with postdischarge support for older patients with congestive heart failure: a meta-analysis. JAMA - Journal of the American Medical Association. 2004; 291(11):1358–1367 [PubMed: 15026403]
- 63.
- Pray D, Hoff J. Implementing a multidisciplinary approach to discharge planning. Nursing Management. 1992; 23(10):52–56 [PubMed: 1407840]
- 64.
- Preen DB, Bailey BE, Wright A, Kendall P, Phillips M, Hung J et al. Effects of a multidisciplinary, post-discharge continuance of care intervention on quality of life, discharge satisfaction, and hospital length of stay: a randomized controlled trial. International Journal for Quality in Health Care. 2005; 17(1):43–51 [PubMed: 15668310]
- 65.
- Puhr MI, Thompson HJ. The use of transitional care models in patients with stroke. Journal of Neuroscience Nursing. 2015; 47(4):223–234 [PubMed: 25906245]
- 66.
- Rich MW, Beckham V, Wittenberg C, Leven CL, Freedland KE, Carney RM. A multidisciplinary intervention to prevent the readmission of elderly patients with congestive heart failure. New England Journal of Medicine. 1995; 333(18):1190–1195 [PubMed: 7565975]
- 67.
- Rich MW, Vinson JM, Sperry JC, Shah AS, Spinner LR, Chung MK et al. Prevention of readmission in elderly patients with congestive heart failure: results of a prospective, randomized pilot study. Journal of General Internal Medicine. 1993; 8(11):585–590 [PubMed: 8289096]
- 68.
- Rousseaux M, Daveluy W, Kozlowski R. Value and efficacy of early supported discharge from stroke units. Annals of Physical and Rehabilitation Medicine. 2009; 52(3):224–233 [PubMed: 19522037]
- 69.
- Rudd AG. Correction: randomised controlled trial to evaluate early discharge scheme for patients with stroke (British Medical Journal (1997) 25 October (1039-1044)). BMJ. 1998; 316(7129):435 [PMC free article: PMC2127677] [PubMed: 9366727]
- 70.
- Saleh SS, Freire C, Morris-Dickinson G, Shannon T. An effectiveness and cost-benefit analysis of a hospital-based discharge transition program for elderly Medicare recipients. Journal of the American Geriatrics Society. 2012; 60(6):1051–1056 [PubMed: 22690981]
- 71.
- Sharif F, Moshkelgosha F, Molazem Z, Najafi Kalyani M, Vossughi M. The effects of discharge plan on stress, anxiety and depression in patients undergoing percutaneous transluminal coronary angioplasty: a randomized controlled trial. International Journal of Community Based Nursing and Midwifery. 2014; 2(2):60–68 [PMC free article: PMC4201194] [PubMed: 25349846]
- 72.
- Shepperd S, Parkes J, McClaren J, Phillips C. Discharge planning from hospital to home. Cochrane Database of Systematic Reviews. 2004; Issue 1:CD000313. DOI:10.1002/14651858.CD000313.pub2 [PubMed: 14973952] [CrossRef]
- 73.
- Shepperd S, Doll H, Broad J, Gladman J, Iliffe S, Langhorne P et al. Early discharge hospital at home. Cochrane Database of Systematic Reviews. 2009; Issue 1:CD000356. DOI:10.1002/14651858.CD000356.pub3 [PMC free article: PMC4175532] [PubMed: 19160179] [CrossRef]
- 74.
- Shepperd S, Lannin NA, Clemson LM, McCluskey A, Cameron ID, Barras SL. Discharge planning from hospital to home. Cochrane Database of Systematic Reviews. 2013; Issue 1:CD000313. DOI:10.1002/14651858.CD000313.pub4 [PubMed: 23440778] [CrossRef]
- 75.
- Shepperd S, McClaran J, Phillips CO, Lannin NA, Clemson LM, McCluskey A et al. Discharge planning from hospital to home. Cochrane Database of Systematic Reviews. 2010; Issue 1:CD000313. DOI:10.1002/14651858.CD000313.pub3 [PubMed: 20091507] [CrossRef]
- 76.
- Sulch D, Perez I, Melbourn A, Kalra L. Randomized controlled trial of integrated (managed) care pathway for stroke rehabilitation. Stroke. 2000; 31(8):1929–1934 [PubMed: 10926959]
- 77.
- Torp CR, Vinkler S, Pedersen KD, Hansen FR, Jorgensen T, Willaing I et al. Model of hospital-supported discharge after stroke. Stroke. 2006; 37(6):1514–1520 [PubMed: 16645132]
- 78.
- Ulin K, Olsson L-E, Wolf A, Ekman I. Person-centred care - an approach that improves the discharge process. European Journal of Cardiovascular Nursing. 2014; 15(3):e19–e26 [PubMed: 25648848]
- 79.
- Utens CMA, Goossens LMA, Smeenk FWJM, Rutten-van Molken MPMH, van Vliet M, Braken MW et al. Early assisted discharge with generic community nursing for chronic obstructive pulmonary disease exacerbations: results of a randomised controlled trial. BMJ Open. 2012; 2(5):e001684 [PMC free article: PMC3488726] [PubMed: 23075570]
- 80.
- Weinberger M, Oddone EZ, Henderson WG. Does increased access to primary care reduce hospital readmissions? Veterans Affairs Cooperative Study Group on Primary Care and Hospital Readmission. New England Journal of Medicine. 1996; 334(22):1441–1447 [PubMed: 8618584]
- 81.
- Zhu QM, Liu J, Hu HY, Wang S. Effectiveness of nurse-led early discharge planning programmes for hospital inpatients with chronic disease or rehabilitation needs: a systematic review and meta-analysis. Journal of Clinical Nursing. 2015; 24(19-20):2993–3005 [PubMed: 26095175]
Appendices
Appendix A. Review protocol
Table 4Review protocol: Discharge planning
| Review question | Discharge planning |
|---|---|
| Guideline condition | Acute medical emergencies. |
| Review population | Adults and young people (16 years and over) with a suspected or confirmed AME (discharged from the acute hospital). |
| Adults | |
| Line of therapy not an inclusion criterion. | |
|
Interventions and comparators: generic/class; specific/drug (All interventions will be compared with each other, unless otherwise stated) |
Discharge planning; discharge planning as defined by study. Usual care; as defined by study. Standard processes; usual practice. |
| Outcomes |
|
| Study design | Systematic reviews (SRs) of RCTs, RCTs, observational studies only to be included if no relevant SRs or RCTs are identified. |
| Unit of randomisation |
Patient. Hospital. Ward. |
| Crossover study | Not permitted. |
| Minimum duration of study | Not defined. |
| Subgroup analyses if there is heterogeneity |
|
| Search criteria |
Databases: Medline, Embase, the Cochrane Library, CINAHL. Date limits for search: none. Language: English only. |
Appendix B. Clinical article selection
Appendix C. Forest plots
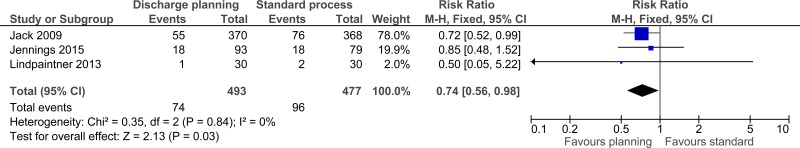
C.1. Discharge planning versus standard processes
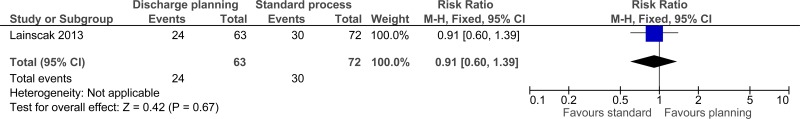
Figure 9Quality of life (minimal clinically important difference on St. George’s Respiratory Questionnaire)
Appendix D. Clinical evidence tables
Download PDF (569K)
Appendix E. Economic evidence tables
No relevant health economic studies were identified.
Appendix F. GRADE tables
Table 5Clinical evidence profile: Discharge planning versus standard processes
| Quality assessment | No of patients | Effect | Quality | Importance | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| No of studies | Design | Risk of bias | Inconsistency | Indirectness | Imprecision | Other considerations | Discharge | standard processes | Relative (95% CI) | Absolute | ||
| Readmission (follow-up 30 days; assessed with: number readmitted) | ||||||||||||
| 1 | randomised trials | serious1 | no serious inconsistency | serious2 | serious3 | none | - | 0% | HR 1.17 (0.79 to 1.73) | - |
⨁◯◯◯ VERY LOW | IMPORTANT |
| Readmission (follow-up 5-30 days; assessed with: number readmitted) | ||||||||||||
| 3 | randomised trials | serious1 | no serious inconsistency | no serious indirectness | serious3 | none |
74/493 (15%) | 20.7% | RR 0.74 (0.56 to 0.98) | 54 fewer per 1000 (from 4 fewer to 91 fewer) |
⨁⨁◯◯ LOW | IMPORTANT |
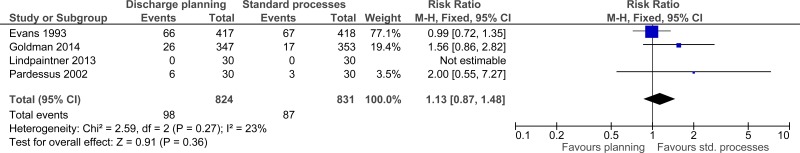
| Mortality (follow-up 5 days -12 months; assessed with: number of deaths) | ||||||||||||
| 4 | randomised trials | no serious risk of bias | no serious inconsistency | no serious indirectness | serious3 | none |
98/824 (11.9%) | 10% | RR 1.13 (0.87 to 1.48) | 13 more per 1000 (from 13 fewer to 48 more) |
⨁⨁⨁◯ MODERATE | CRITICAL |
| Mortality (follow-up 6 months; assessed with: number of deaths) | ||||||||||||
| 1 | randomised trials | no serious risk of bias | no serious inconsistency | serious2 | very serious3 | none | - | 0% | HR 0.54 (0.23 to 1.27) | - |
⨁◯◯◯ VERY LOW | CRITICAL |
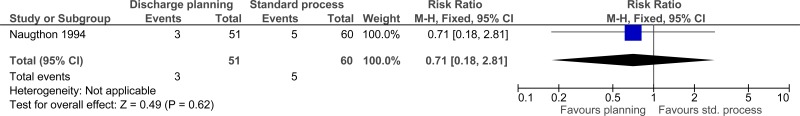
| Mortality (in-hospital) (follow-up during admission; assessed with: number of deaths during admission) | ||||||||||||
| 1 | randomised trials | no serious risk of bias | no serious inconsistency | serious2 | very serious3 | none |
3/51 (5.9%) | 8.3% | RR 0.71 (0.18 to 2.81) | 24 fewer per 1000 (from 68 fewer to 150 more) |
⨁◯◯◯ VERY LOW | CRITICAL |
| Avoidable adverse events (follow-up 1-5 days; assessed with: adverse medicine reaction) | ||||||||||||
| 1 | randomised trials | very serious1 | no serious inconsistency | serious2 | very serious3 | none |
3/30 (10%) | 6.7% | RR 1.5 (0.27 to 8.34) | 34 more per 1000 (from 49 fewer to 492 more) |
⨁◯◯◯ VERY LOW | CRITICAL |
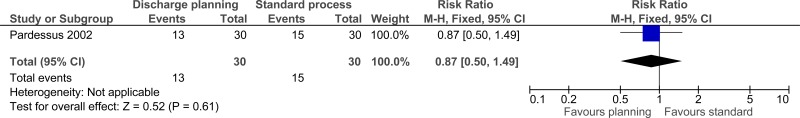
| Avoidable adverse events (follow-up 12 months; assessed with: falls) | ||||||||||||
| 1 | randomised trials | very serious1 | no serious inconsistency | no serious indirectness | very serious3 | none |
13/30 (43.3%) | 50% | RR 0.87 (0.5 to 1.49) | 65 fewer per 1000 (from 250 fewer to 245 more) |
⨁◯◯◯ VERY LOW | CRITICAL |
| Quality of life (follow-up 180 days; assessed with: minimal clinically important difference on St. George’s Respiratory Questionnaire) | ||||||||||||
| 1 | randomised trials | serious1 | no serious inconsistency | serious2 | very serious3 | none |
24/63 (38.1%) | 41.7% | RR 0.91 (0.6 to 1.39) | 38 fewer per 1000 (from 167 fewer to 163 more) |
⨁◯◯◯ VERY LOW | CRITICAL |
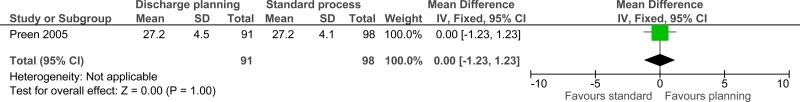
| Quality of life (follow-up 7 days; measured with: medical outcomes study short form 12 - physical ratings; Better indicated by higher values) | ||||||||||||
| 1 | randomised trials | very serious1 | no serious inconsistency | no serious indirectness | no serious imprecision | none | 91 | 98 | - | MD 0 higher (1.23 lower to 1.23 higher) |
⨁⨁◯◯ LOW | CRITICAL |
| Quality of life (follow-up 7 days; measured with: medical outcomes study short form 12 - mental ratings; Better indicated by higher values) | ||||||||||||
| 1 | randomised trials | very serious1 | no serious inconsistency | no serious indirectness | serious3 | none | 91 | 98 | - | MD 1.5 higher (0.11 lower to 3.11 higher) |
⨁◯◯◯ VERY LOW | CRITICAL |
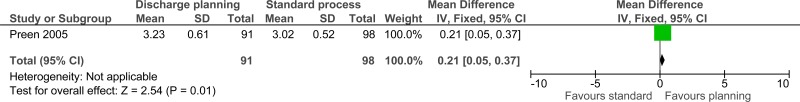
| Patient satisfaction (follow-up 7 days; measured with: rating of discharge process; Better indicated by higher values) | ||||||||||||
| 1 | randomised trials | very serious1 | no serious inconsistency | no serious indirectness | serious3 | none | 91 | 98 | - | MD 0.21 higher (0.05 to 0.37 higher) |
⨁◯◯◯ VERY LOW | CRITICAL |
| Patient satisfaction (follow-up 30 days; assessed with: preparedness to leave hospital (prepared or very prepared)) | ||||||||||||
| 1 | randomised trials | serious1 | no serious inconsistency | no serious indirectness | serious3 | none |
197/307 (64.2%) | 52.9% | RR 1.21 (1.06 to 1.39) | 111 more per 1000 (from 32 more to 206 more) |
⨁⨁◯◯ LOW | CRITICAL |
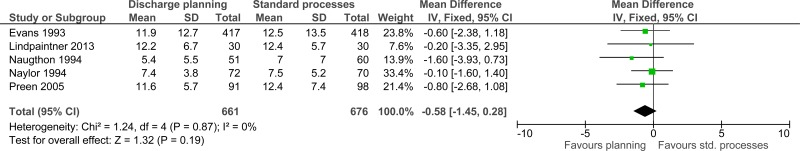
| Length of stay (measured with: days in hospital; Better indicated by lower values) | ||||||||||||
| 5 | randomised trials | serious1 | no serious inconsistency | no serious indirectness | no serious imprecision | none | 661 | 676 | - | MD 0.58 lower (1.45 lower to 0.28 higher) |
⨁⨁⨁◯ MODERATE | CRITICAL |
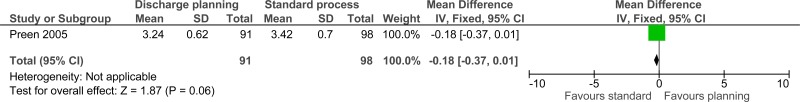
| Staff satisfaction (follow-up 7 days; measured with: GP satisfaction; Better indicated by higher values) | ||||||||||||
| 1 | randomised trials | very serious1 | no serious inconsistency | no serious indirectness | no serious imprecision | none | 91 | 98 | - | MD 0.18 lower (0.37 lower to 0.01 higher) |
⨁⨁◯◯ LOW | IMPORTANT |
- 1
Downgraded by 1 increment if the majority of the evidence was at high risk of bias, and downgraded by 2 increments if the majority of the evidence was at very high risk of bias.
- 2
Downgraded by 1 or 2 increments because the majority of the evidence was based on indirect interventions (interventions included post discharge components).
- 3
Downgraded by 1 increment if the confidence interval crossed 1 MID or by 2 increments if the confidence interval crossed both MIDs.
Appendix G. Excluded clinical studies
Table 6Studies excluded from the clinical review
| Study | Exclusion reason |
|---|---|
| Altfeld 20131 | Incorrect interventions (post discharge intervention) |
| Anderson 20022 | Systematic review (not relevant or unclear PICO) |
| Anon 200015 | Systematic review (not relevant or unclear PICO) |
| Anon 2004 | Study summary |
| Atienza 20043 | Incorrect intervention (multicomponent intervention – patient and family education prior to discharge, post discharge visit with primary care physician and regular follow up visits at a heart failure clinic) |
| Azzalini 20154 | Incorrect interventions. early supported discharge |
| Balaban 20085 | Said to be an RCT but patients were not randomised |
| Beech 19996 | Incorrect interventions. early supported discharge |
| Braet 20127 | Systematic review protocol |
| Clemson 20169 | Incorrect comparison (discharge planning with home follow up vs. in-hospital discharge planning) |
| Cotton 200010 | Data not useable (no SDs provided) |
| Cunliffe 200411 | Not guideline condition (fracture) |
| Davies 200712 | Incorrect study design |
| Domingo 201213 | Systematic review protocol |
| Durvasula 201514 | Incorrect study design |
| Farren 199117 | Incorrect study design |
| Finn 201118 | Incorrect interventions (nurse discharge facilitator assigned to patients who were ready for discharge to assist with discharge processes) |
| Fox 201321 | Systematic review (not relevant or unclear PICO) |
| Fox 201620 | Commentary |
| Fjaertoft 200419 | Incorrect interventions. early supported discharge |
| George 201322 | Letter |
| Goncalves-bradley 201624 | Systematic review is not relevant to review question or unclear PICO |
| Haggmark 199725 | Incorrect population (cancer patients) |
| Harrison 199026 | Article |
| Harrison 200227 | Inappropriate comparison - both arms received the same discharge planning |
| Hesselink 201228 | Systematic review (not relevant or unclear PICO) |
| Hofstad 201429 | Incorrect interventions (early supported discharge) |
| Hyde 200030 | Incorrect interventions (post discharge intervention; supported discharge) |
| Indredavik 200031 | Incorrect interventions (early supported discharge) |
| Kleinpell 200434 | Not guideline condition. outcomes not useable (no SDs given) |
| Kotowycz 201035 | Incorrect interventions (early supported discharge) |
| Langhorne 200537 | Systematic review (not relevant or unclear PICO) |
| Langhorne 200738 | Systematic review (not relevant or unclear PICO) |
| Laramee 200339 | Incorrect interventions - congestive heart failure case manager, multicomponent intervention (early discharge planning and coordination of care, patient education, enhanced telephone follow up and promotion of CHF medications) |
| Legrain 201140 | Inappropriate comparison (discharge planning in both arms) |
| Linden 201441 | Incorrect intervention (multicomponent intervention including several post discharge components) |
| Lockwood 201543 | Systematic review is not relevant to review question or unclear PICO |
| Mahler 201544 | Systematic review (not relevant or unclear PICO) |
| Mazloum 201645 | Non-OECD country |
| Mcclellan 201346 | Incorrect population (soft tissue injury) |
| Mcinnes 199947 | Incorrect interventions. GP input in to discharge planning |
| Mcnamee 199848 | No useable outcomes |
| Melberg 201549 | Incorrect interventions. early discharge for low risk patients |
| Mistiaen 200750 | Systematic review (not relevant or unclear PICO) |
| Moher 199251 | Incorrect interventions - medical team coordinator (27% of the time spent on activities related to discharge planning, rest of the time participating in ward rounds, generating bed census, retrieving missing medical information etc.) |
| Naylor 199954 | Incorrect intervention (discharge planning and home follow up protocol implemented by advanced practice nurses 4 weeks post discharge) |
| Naylor 1999B55 | Incorrect intervention (discharge planning and home follow up protocol implemented by advanced practice nurses 4 weeks post discharge) |
| Nazareth 200156 | Incorrect interventions - pharmacy discharge plan at discharge |
| Palmer 200158 | Incorrect study design |
| Parfrey 199460 | Incorrect population |
| Parkes 200061 | Systematic review (not relevant or unclear PICO) |
| Phillips 200462 | Systematic review (not relevant or unclear PICO) |
| Pray 199263 | Narrative article |
| Puhr 201565 | Systematic review is not relevant to review question or unclear PICO |
| Rich 199367 | Incorrect interventions - multicomponent intervention (intensive patient education, analysis of medications, early discharge planning and enhanced follow up through home care and telephone contact |
| Rich 199566 | Incorrect interventions - multicomponent intervention (intensive patient education, dietary assessment, consultation with social services personnel, analysis of medications, intensive post discharge follow up by hospital’s home care services |
| Rousseaux 200968 | Systematic review (not relevant or unclear PICO) |
| Rudd 199869 | Correction |
| Saleh 201270 | Incorrect interventions (intervention is post discharge) |
| Sharif 201471 | Non-OECD country |
| Shepperd 200472 | Systematic review (not relevant or unclear PICO) |
| Shepperd 200973 | Systematic review (not relevant or unclear PICO) |
| Shepperd 201075 | Systematic review (not relevant or unclear PICO) |
| Shepperd 201374 | Systematic review (not relevant or unclear PICO) |
| Sulch 200076 | Incorrect interventions - inpatient rehabilitation |
| Torp 200677 | Inappropriate comparison. discharge planning in both arms |
| Utens 201279 | Incorrect intervention (early supported discharge) |
| Ulin 201478 | Incorrect study design |
| Weinberger 199680 | Incorrect interventions - increased access to primary care before and after discharge |
| Zhu 201581 | Systematic review (incorrect PICO); references screened |
Appendix H. Excluded health economic studies
No health economic studies were excluded from this review.
- Discharge planning - Emergency and acute medical care in over 16s: service deliv...Discharge planning - Emergency and acute medical care in over 16s: service delivery and organisation
- Standardised systems of care for intra- and inter-hospital transfers - Emergency...Standardised systems of care for intra- and inter-hospital transfers - Emergency and acute medical care in over 16s: service delivery and organisation
- Cost-effectiveness analyses - Emergency and acute medical care in over 16s: serv...Cost-effectiveness analyses - Emergency and acute medical care in over 16s: service delivery and organisation
- GP access to laboratory investigations - Emergency and acute medical care in ove...GP access to laboratory investigations - Emergency and acute medical care in over 16s: service delivery and organisation
- Multidisciplinary team meetings - Emergency and acute medical care in over 16s: ...Multidisciplinary team meetings - Emergency and acute medical care in over 16s: service delivery and organisation
Your browsing activity is empty.
Activity recording is turned off.
See more...