OVERVIEW
Introduction
Fluvoxamine is a selective serotonin reuptake inhibitor (SSRI) used in the therapy of obsessive-compulsive disorder. Fluvoxamine therapy can be associated with transient asymptomatic elevations in serum aminotransferase levels and has been linked to rare instances of clinically apparent acute liver injury.
Background
Fluvoxamine (floo vox' a meen) is a selective serotonin reuptake inhibitor (SSRI) that was developed largely for use in obsessive-compulsive disorder. Fluvoxamine acts by blocking the reuptake of serotonin in CNS synaptic clefts, thus increasing serotonin levels in the brain which is associated with its psychiatric effects. Fluvoxamine was approved for use in obsessive-compulsive disorder in 1994 in the United States and is used in both adults and children above the age of 8 years. It is also used for social anxiety disorder, but not specifically for depression or bipolar disorders. Fluvoxamine is available as tablets of 25, 50 and 100 mg in multiple generic forms and under the brand name of Luvox. Extended release forms are also available in doses of 100 and 150 mg. The recommended dosage in adults is 50 mg once daily, increasing to a maximum of 300 mg. The dosage in children is 25 mg daily, increasing to a maximum of 200 to 300 mg based upon age below or above 11 years. Common side effects are drowsiness, dyspepsia, nausea, headache, increased sweating, increased appetite, weight gain and sexual dysfunction.
Fluvoxamine is also a potent sigma-1 receptor (S1R) agonist, which results in an inhibition of proflammatory cytokine production. Because the proinflammatory cytokines such as IL-6 play a role in the hyperinflammatory response in severe COVID-19 pneumonia, fluvoxamine has been proposed as a therapy for COVID-19. Several small case series and clinical trials have suggested that fluvoxamine may prevent clinical deterioration in patients with SARS-CoV-2 infection, particularly if used before the onset of respiratory failure and the full scale hyperinflammatory state. Clinical trials of the efficacy or safety of fluvoxamine are currently underway.
Hepatotoxicity
Liver test abnormalities have been reported to occur in up to 1% patients on fluvoxamine, but elevations are usually modest and usually do not require dose modification or discontinuation. A few instances of acute, clinically apparent episodes of liver injury with marked liver enzyme elevations with no or minimal jaundice have been reported in patients on fluvoxamine. The onset of injury was within a few days of starting therapy and the pattern of serum enzyme elevations was hepatocellular or mixed. Autoimmune (autoantibodies) and immunoallergic features (rash, fever, eosinophilia) were not mentioned. Too few cases have been reported to characterize the clinical features of the liver injury in any detail. In large scale analyses of hepatic adverse events due to antidepressants and SSRIs, fluvoxamine is rarely mentioned.
Likelihood score: D (possible rare cause of clinically apparent liver injury).
Mechanism of Injury
The mechanism by which fluvoxamine causes liver injury is not known. Fluvoxamine is extensively metabolized by the liver, mainly via the cytochrome P450 system, and hepatotoxicity may be mediated by toxic intermediates of their metabolism. In addition, fluvoxamine inhibits several CYP enzymes and has significant drug-drug interactions.
Outcome and Management
The serum aminotransferase elevations that occur on fluvoxamine therapy are usually self-limited and do not require dose modification or discontinuation of therapy. No instances of acute liver failure or chronic liver injury have been attributed to fluvoxamine therapy. Restarting fluvoxamine has been reported to cause a rapid recurrence of injury and should be avoided. Persons with intolerance to fluvoxamine may have similar reactions to other SSRIs, and careful monitoring is warranted if other such agents are used.
Drug Class: Antidepressant Agents, COVID-19 Drugs
Other Drugs in the Subclass, SNRIs/SSRIs: Citalopram, Escitalopram, Duloxetine, Fluoxetine, Levomilnacipran, Paroxetine, Sertraline, Venlafaxine, Vilazodone, Vortioxetine
PRODUCT INFORMATION
REPRESENTATIVE TRADE NAMES
Fluvoxamine – Generic, Luvox®
DRUG CLASS
Antidepressant Agents
Product labeling at DailyMed, National Library of Medicine, NIH
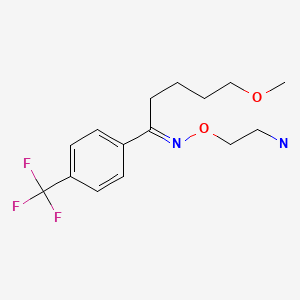
CHEMICAL FORMULA AND STRUCTURE
ANNOTATED BIBLIOGRAPHY
References updated: 11 May 2021
- Zimmerman HJ. Tricyclic antidepressants. In, Zimmerman HJ. Hepatotoxicity: the adverse effects of drugs and other chemicals on the liver. 2nd ed. Philadelphia: Lippincott, 1999, pp. 493-8.(Expert review of hepatotoxicity published in 1999 discusses several antidepressants including SSRIs but not fluvoxamine).
- Larrey D, Ripault MP. Hepatotoxicity of psychotropic drugs and drugs of abuse. In, Kaplowitz N, DeLeve LD, eds. Drug-induced liver disease. 3rd ed. Amsterdam: Elsevier, 2013, pp. 443-62.(Review of hepatotoxicity of antidepressants mentions that clinically apparent liver injury from fluvoxamine is rare and the clinical picture is usually hepatocellular).
- O'Donnell JM, Shelton RC. Drug therapy for depression and anxiety disorders. In, Brunton LL, Chabner BA, Knollman BC, eds. Goodman & Gilman’s the pharmacological basis of therapeutics. 12th ed. New York: McGraw-Hill, 2011, pp. 397-416.(Textbook of pharmacology and therapeutics).
- Lam KS, Blanchi A, Chavaillon JM. Gastroenterol Clin Biol. 1988;12:398–9. [Hepatitis probably secondary to the massive ingestion of fluvoxamine] [PubMed: 3133277](63 year old woman took an overdose of fluvoxamine [~1500 mg] and within 24 hours had elevations in ALT [1059 U/L], Alk P [668 U/L] and bilirubin [1.4 mg/dL], which remained high for more than a month).
- Mourilhe P, Stokes PE. Risks and benefits of selective serotonin reuptake inhibitors in the treatment of depression. Drug Saf. 1998;18:57–82. [PubMed: 9466088](Review of pharmacology, efficacy and safety of SSRIs; no mention of ALT elevations or hepatotoxicity).
- Grohmann R, Rüther E, Engel RR, Hippius H. Assessment of adverse drug reactions in psychiatric inpatients with the AMSP drug safety program: methods and first results for tricyclic antidepressants and SSRI. Pharmacopsychiatry. 1999;32:21–8. [PubMed: 10071179](Analysis of reporting of adverse events among inpatients in 29 German hospitals between 1993 to 1997; 896 severe adverse events were reported among 48,564 patients [1.8%], both total and hepatic events were more common with tricyclics than SSRIs).
- Carvajal García-Pando A, García del Pozo J, Sánchez AS, Velasco MA, Rueda de Castro AM, Lucena MI. Hepatotoxicity associated with the new antidepressants. J Clin Psychiatry. 2002;63:135–7. [PubMed: 11874214](Analysis of cases of hepatotoxicity from antidepressants in Spanish Pharmacovigilance System from 1989-1999, identified 99 cases; among SSRIs, 26 were due to fluoxetine, 14 paroxetine, 6 fluvoxamine, 5 sertraline, 3 venlafaxine and 2 citalopram; among tricyclics, 16 clomipramine 7 amitriptyline, 6 imipramine; among miscellaneous, 3 nefazodone and 1 trazodone; but all similar in rate of occurrence estimated to be 1-3 per 100,000 patient-years of exposure, except for nefazodone=29/100,000).
- Lucena MI, Carvajal A, Andrade R, Velasco A. Antidepressant-induced hepatotoxicity. Expert Opin Drug Saf. 2003;2:249–62. [PubMed: 12904104](Review of hepatotoxicity of antidepressants; antidepressant use has increased markedly between 1992 and 2002, accounting for 5% of cases of hepatotoxicity; SSRIs are less likely to cause injury than tricyclics and MAO inhibitors; range of presentations, typically self-limited and rapid recovery; no hallmarks of hypersensitivity).
- Spigset O, Hägg S, Bate A. Hepatic injury and pancreatitis during treatment with serotonin reuptake inhibitors: data from the World Health Organization (WHO) database of adverse drug reactions. Int Clin Psychopharmacol. 2003;18:157–61. [PubMed: 12702895](Among 27,542 reports of hepatic injury in WHO database, 786 were related to SSRIs [3%], including citalopram 42, fluoxetine 222, fluvoxamine 54, paroxetine 191, sertraline 112, nefazodone 91 and venlafaxine 74; only nefazodone had an excess of hepatic reports in relationship to total reports).
- Degner D, Grohmann R, Kropp S, Rüther E, Bender S, Engel RR, Schmidt LG. Severe adverse drug reactions of antidepressants: results of the German multicenter drug surveillance program AMSP. Pharmacopsychiatry. 2004;37 Suppl 1:S39–45. [PubMed: 15052513](Analysis of adverse drug reactions reported from 1993-2000 in 35 psychiatric hospitals; 0.7% of SSRI recipients had a severe adverse event; hepatic in 0.05%).
- Solomons K, Gooch S, Wong A. Toxicity with selective serotonin reuptake inhibitors. Am J Psychiatry. 2005;162:1225. [PubMed: 15930079](38 year old woman developed abdominal pain and ALT elevations [378 U/L] without jaundice 9 days after starting fluvoxamine; had a positive rechallenge and recurrence with citalopram [ALT 379 within 4 days], and positive rechallenge with citalopram again 1 year later).
- Pinzani V, Peyrière H, Hillaire-Buys D, Pageaux GP, Blayac BP, Larrey D. Specific serotonin recapture inhibitor (SSRI) antidepressants: hepatoxicity assessment in a large cohort in France. J Hepatol. 2006;44 Suppl 2:S256.(Abstract; analysis of French Pharmacovigilance data on SSRIs found 63 cases of hepatotoxicity from paroxetine, 45 fluoxetine, 30 citalopram, 18 sertraline, and 2 fluvoxamine).
- Sabaté M, Ibáñez L, Pérez E, Vidal X, Buti M, Xiol X, Mas A, et al. Risk of acute liver injury associated with the use of drugs: a multicentre population survey. Aliment Pharmacol Ther. 2007;25:1401–9. [PubMed: 17539979](Among 126 cases of drug induced liver injury seen in Spain between 1993-2000, 3 were attributed to paroxetine and 3 to fluoxetine with a relative risk of injury to rate of use in the population of 3.0 and 1.8, respectively).
- DeSanty KP, Amabile CM. Antidepressant-induced liver injury. Ann Pharmacother. 2007;41:1201–11. [PubMed: 17609231](Review of drug induced liver injury and reports of injury from MAO inhibitors, SSRIs, tricyclics and atypical agents).
- Chalasani N, Fontana RJ, Bonkovsky HL, Watkins PB, Davern T, Serrano J, Yang H, Rochon J., Drug Induced Liver Injury Network (DILIN). Causes, clinical features, and outcomes from a prospective study of drug-induced liver injury in the United States. Gastroenterology. 2008;135:1924–34. [PMC free article: PMC3654244] [PubMed: 18955056](Among 300 cases of drug induced liver disease in the US collected from 2004 to 2008, 6 were attributed to duloxetine, 3 to atomoxetine, 2 to fluoxetine, 2 to bupropion, and 1 to sertraline as single agents; no case attributed to fluvoxamine).
- Reuben A, Koch DG, Lee WM., Acute Liver Failure Study Group. Drug-induced acute liver failure: results of a U.S. multicenter, prospective study. Hepatology. 2010;52:2065–76. [PMC free article: PMC3992250] [PubMed: 20949552](Among 1198 patients with acute liver failure enrolled in a US prospective study between 1998 and 2007, 133 were attributed to drug induced liver injury, including 1 due to fluoxetine and 1 to venalaxine but none to fluvoxamine).
- Molleston JP, Fontana RJ, Lopez MJ, Kleiner DE, Gu J, Chalasani N. Drug-induced Liver Injury Network. Characteristics of idiosyncratic drug-induced liver injury in children: results from the DILIN prospective study. J Pediatr Gastroenterol Nutr. 2011;53:182–9. [PMC free article: PMC3634369] [PubMed: 21788760](Among 30 children with suspected drug induced liver injury, half [n=15] were due to antimicrobials [minocycline 4, INH 3, azithromycin 3] and the rest largely due to CNS agents and anticonvulsants; one case was attributed to amitriptyline, but no other antidepressant was listed).
- Park SH, Ishino R. Liver injury associated with antidepressants. Curr Drug Saf. 2013;8:207–23. [PubMed: 23914755](Review of antidepressant induced liver injury).
- Björnsson ES, Bergmann OM, Björnsson HK, Kvaran RB, Olafsson S. Incidence, presentation and outcomes in patients with drug-induced liver injury in the general population of Iceland. Gastroenterology. 2013;144:1419–25. [PubMed: 23419359](In a population based study of drug induced liver injury from Iceland, 96 cases were identified over a 2 year period, none of which were attributed to fluvoxamine or other SSRIs, despite the fact that 5 SSRIs ranked among the top 30 most frequently prescribed drugs in Iceland).
- Voican CS, Corruble E, Naveau S, Perlemuter G. Antidepressant-induced liver injury: a review for clinicians. Am J Psychiatry. 2014;171:404–15. [PubMed: 24362450](Review of antidepressant induced liver injury mentions a single, anicteric case of liver injury attributed to fluvoxamine [Solomons 2005]).
- Hernández N, Bessone F, Sánchez A, di Pace M, Brahm J, Zapata R, A, Chirino R, et al. Profile of idiosyncratic drug induced liver injury in Latin America. An analysis of published reports. Ann Hepatol. 2014;13:231–9. [PubMed: 24552865](Systematic review of literature of drug induced liver injury in Latin American countries published from 1996 to 2012 identified 176 cases, but none were attributed to fluvoxamine).
- Chalasani N, Bonkovsky HL, Fontana R, Lee W, Stolz A, Talwalkar J, Reddy KR, et al. United States Drug Induced Liver Injury Network. Features and outcomes of 899 patients with drug-induced liver injury: The DILIN Prospective Study. Gastroenterology. 2015;148:1340–52.e7. [PMC free article: PMC4446235] [PubMed: 25754159](Among 899 cases of drug induced liver injury enrolled in a US prospective study between 2004 and 2013, 20 cases [2%] were attributed to antidepressants, but none to fluvoxamine).
- Bunchorntavakul C, Reddy KR. Drug hepatotoxicity: newer agents. Clin Liver Dis. 2017;21:115–34. [PubMed: 27842767](Review of newly approved agents that have been linked to liver injury, mentions that fluvoxamine has a lower risk of hepatotoxicity than tricyclic or SNRIs and that it has not been linked to cases of acute liver failure).
- Friedrich ME, Akimova E, Huf W, Konstantinidis A, Papageorgiou K, Winkler D, Toto S, et al. Drug-induced liver injury during antidepressant treatment: results of AMSP, a drug surveillance program. Int J Neuropsychopharmacol. 2016;19:pyv126. pii. [PMC free article: PMC4851269] [PubMed: 26721950](Monitoring of 184,234 inpatients in 80 psychiatric hospitals for liver injury during antidepressant treatment identified 149 cases including 2 among 3991 fluvoxamine treated subjects [0.05%], a rate similar to other SSRIs and SNRIs; no cases resulted in acute liver failure or death from liver disease).
- Ferrajolo C, Scavone C, Donati M, Bortolami O, Stoppa G, Motola D, Vannacci A, et al. DILI-IT Study Group. Antidepressant-induced acute liver injury: a case-control study in an Italian inpatient population. Drug Saf. 2018;41:95–102. [PubMed: 28770534](Among 179 cases of hospitalizations for unexplained acute liver injury enrolled in a prospective study between 2010 and 2014, 17 had been exposed to antidepressants, but none specifically to fluvoxamine).
- Billioti de Gage S, Collin C, Le-Tri T, Pariente A, Bégaud B, Verdoux H, Dray-Spira R, et al. Antidepressants and hepatotoxicity: a cohort study among 5 million individuals registered in the French National Health Insurance Database. CNS Drugs. 2018;32:673–84. [PMC free article: PMC6061298] [PubMed: 29959758](Among 5 million persons identified in a national French health insurance database who started an antidepressant between 2010 and 2015, 382 developed serious liver injury resulting in hospitalization, rates per 100,0000 persons-years being 19 for SSRIs, 22 venlafaxine, 13 duloxetine, and 33 mirtazapine).
- Chan HL, Chiu WC, Chen VC, Huang KY, Wang TN, Lee Y, McIntyre RS, et al. SSRIs associated with decreased risk of hepatocellular carcinoma: A population-based case-control study. Psychooncology. 2018;27:187–92. [PubMed: 28666060](Analysis of the Taiwan National Health Service Insurance Research Database identified 59,859 patients with initial diagnosis of hepatocellular carcinoma and 285,124 matched controls; SSRI [including fluvoxamine] use was more frequent in the controls than in the HCC cases, but only in analyses adjusted for possibly confounding factors).
- Drugs for depression. Med Lett Drugs Ther. 2020;62(1592):25–32. [PubMed: 32320387](Concise review of the mechanism of action, clinical efficacy, safety and costs of drugs for depression; hepatotoxicity is mentioned only for nefazodone [now rarely used because of severe hepatotoxicity] and duloxetine [in heavy drinkers]; most SSRIs but not fluvoxamine are discussed).
- Ueberberg B, Frommberger U, Messer T, Zwanzger P, Kuhn J, Anghelescu I, Ackermann K, Assion HJ. Drug-induced liver injury (DILI) in patients with depression treated with antidepressants: a retrospective multicenter study. Pharmacopsychiatry. 2020;53:60–4. [PubMed: 31958850](Among 329 psychiatric inpatients with depression seen at 6 psychiatric centers in Germany, 17 [5%] had serum aminotransferase elevations but none had clinically apparent liver injury, most commonly implicated drugs included mirtazapine, agomelatine, citalopram and venlafaxine; fluvoxamine is not mentioned).
- Lenze EJ, Mattar C, Zorumski CF, Stevens A, Schweiger J, Nicol GE, Miller JP, et al. Fluvoxamine vs placebo and clinical deterioration in outpatients with symptomatic COVID-19: a randomized clinical trial. JAMA. 2020;324:2292–300. [PMC free article: PMC7662481] [PubMed: 33180097](Among 152 non-hospitalized patients with early SARS-CoV-2 infection, clinical deterioration arose in 8.3% [6 of 72] treated with placebo vs none [0 of 80] treated with fluvoxamine [100 mg three times daily for 14 days], an SSRI that also is a potent sigma-1 receptor agonist; adverse events were more frequent among placebo recipients, 4 of who required hospitalization and one mechanical ventilation vs none receiving fluvoxamine).
- Anderson GM. Fluvoxamine, melatonin and COVID-19. Psychopharmacology (Berl). 2021;238:611. [PMC free article: PMC7779245] [PubMed: 33392622](Review of fluvoxamine and melatonin as potential therapies for COVID-19 mentions that fluvoxamine, besides inhibiting the sigma-1 receptor also inhibits CYP 1A2 and 2C19, effects that decrease the metabolism of melatonin can result in increased serum levels).
- Seftel D, Boulware DR. Prospective cohort of fluvoxamine for early treatment of coronavirus disease 19. Open Forum Infect Dis 2021; 8: ofab050. [PMC free article: PMC7888564] [PubMed: 33623808](Among patients testing positive for SARS-CoV-2 who were offered therapy with fluvoxamine [loading dose followed by 50 mg twice daily for 14 days], 65 agreed among whom none developed symptoms as of day 14 and none were hospitalized compared to 48 who refused treatment among whom 29 developed symptoms, 6 were hospitalized and 1 died).
- Sukhatme VP, Reiersen AM, Vayttaden SJ, Sukhatme VV. Fluvoxamine: a review of Its mechanism of action and its role in COVID-19. Front Pharmacol. 2021;12:652688. [PMC free article: PMC8094534] [PubMed: 33959018](Review of the intracellular actions of fluvoxamine that might play a role in therapy for COVID-19 including its effects on increasing sigma-1 receptor signaling, lysosomal effects blocking viral release, antiinflammatory effects of reduction in platelet aggregation and mast cell degranulation, and drug-interaction effects in delaying metabolism of melatonin).
- Fluvoxamine for COVID-19? Med Lett Drugs Ther. 2021;63(1623):69–70. [PubMed: 33976099](Concise review of the mechanism of action, evidence for clinical efficacy, safety and costs of fluvoxamine which is an unapproved therapy for COVID-19 that is now undergoing rigorous evaluation in randomized, placebo controlled trials).
Publication Details
Publication History
Last Update: May 11, 2021.
Copyright
Publisher
National Institute of Diabetes and Digestive and Kidney Diseases, Bethesda (MD)
NLM Citation
LiverTox: Clinical and Research Information on Drug-Induced Liver Injury [Internet]. Bethesda (MD): National Institute of Diabetes and Digestive and Kidney Diseases; 2012-. Fluvoxamine. [Updated 2021 May 11].