OVERVIEW
Introduction
Ribociclib is a unique cyclin-dependent kinase inhibitor that is used in combination with aromatase inhibitors in the treatment of postmenopausal women with metastatic breast cancer. Ribociclib is associated with a moderate rate of serum aminotransferase elevations during therapy, and to clinically apparent liver injury in a proportion of these.
Background
Ribociclib (rye" boe sye' klib) is an orally available, small molecule inhibitor of cyclin-dependent kinases 4 and 6 that is used in combination with aromatase inhibitors in the therapy of postmenopausal women with metastatic breast cancer that is positive for the estrogen hormone receptor (ER+), but negative for human epidermal growth factor receptor 2 (HER2-). The cyclin kinases 4 and 6 regulate the cellular transition from the G1 to the S phase of the cell cycle acting through the retinoblastoma protein (Rb) pathway. Inhibition of this transition blocks the progression of the cell cycle and results in growth arrest in rapidly dividing cells. Components of this pathway are often mutated or overexpressed in cancer cells. In several clinical trials, the addition of ribociclib to letrozole (aromatase inhibitor) therapy of advanced or metastatic breast cancer (ER+, HER2-) in postmenopausal women was associated with a prolongation of disease-free but not overall survival. Ribociclib received accelerated approval for use in the United States in 2017. Ribociclib is under investigation as therapy of several solid tumors and lymphomas, but the initial indications were limited to advanced or metastatic ER+, HER2- breast cancer in postmenopausal women given in combination with an aromatase inhibitor. Ribociclib is available in tablets of 200 mg under the brand name Kisqali, and the initial recommended dose is 600 mg once daily in 21 day cycles every 28 days indefinitely or until there is disease progression. Common side effects include neutropenia, fatigue, nausea, diarrhea, anorexia, thrombocytopenia, headache and back pain. Less common, but potentially severe adverse reactions include prolongation of the QTc interval, severe neutropenia, fever and infections, and embryo-fetal toxicity.
Hepatotoxicity
In the large clinical trials, adverse events were common and led to dose reductions in 45% of patients and discontinuation in 7%. In preregistration clinical trials, ALT elevations occurred in 46% of ribociclib vs 36% of control subjects and elevations above 5 times the ULN in 10% vs 1%. In one study, 1% of recipients developed clinically apparent liver injury with jaundice, but all recovered. The liver injury arose after 3 to 5 cycles and presented with asymptomatic elevations in serum ALT followed by symptoms and jaundice. Immunoallergic and autoimmune features were not present, although liver histology sometimes showed autoimmune hepatitis-like features. Recovery was slow (3 to 5 months), but ultimately complete. Restarting ribociclib resulted in more rapid and severe recurrence. Thus, experience with ribociclib is limited, but it appears to be capable of causing significant liver injury.
Likelihood score: C (probable cause of clinically apparent liver injury).
Mechanism of Injury
The causes of serum enzyme elevations and liver injury from ribociclib therapy are not known. Ribociclib is extensively metabolized in the liver largely through the CYP 3A4 pathway and liver injury might be caused by production of a toxic or immunogenic intermediate. On the other hand, inhibition of cyclin-dependent kinases 4 and 6 may also affect hepatocytes and have direct toxicity. Because it is a substrate for CYP 3A4, ribociclib is susceptible to drug-drug interactions with agents that inhibit or induce this specific hepatic microsomal activity.
Outcome and Management
The product label for ribociclib recommends prospective monitoring of liver tests during therapy, with values obtained before starting, at 2 week intervals during the first two cycles and at the beginning of the ensuing 4 cycles, and “as clinically indicated” thereafter. The product label also provides careful recommendations for dose interruption, reduction or discontinuation based upon toxicities (neutropenia, liver injury, QTc prolongation), with dose interruption until recovery for aminotransferase elevations above 3 times ULN, interruption until normal and subsequent dose reduction if above 5 times ULN, and permanent discontinuation if above 20 times ULN or in the presence of ALT elevations and jaundice. There is no information regarding cross reactivity in risk for adverse events, hypersensitivity or hepatic injury between ribociclib and palbociclib or other cyclin-dependent kinase inhibitors.
Drug Class: Antineoplastic Agents, Protein Kinase Inhibitors
Other Cyclin-Dependent Kinase Inhibitor Drugs: Palbociclib
PRODUCT INFORMATION
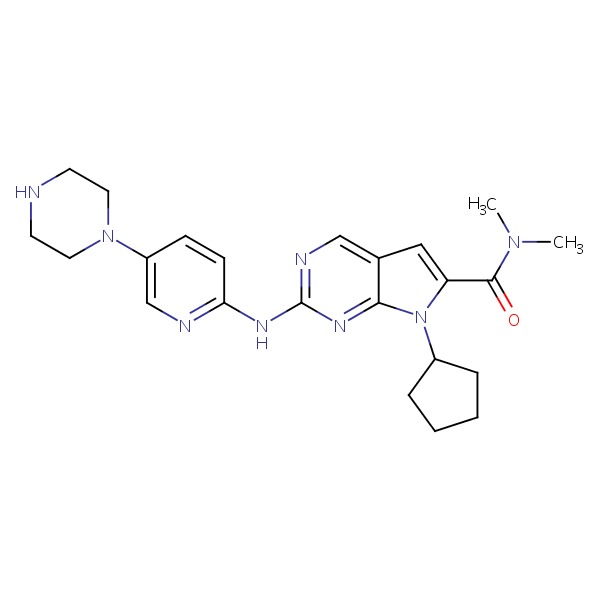
CHEMICAL FORMULA AND STRUCTURE
ANNOTATED BIBLIOGRAPHY
References updated: 08 May 2018
- Zimmerman HJ. Hepatotoxicity: the adverse effects of drugs and other chemicals on the liver. 2nd ed. Philadelphia: Lippincott, 1999.(Review of hepatotoxicity published in 1999 before the availability of kinase inhibitors including palbociclib and ribociclib).
- DeLeve LD. Erlotinib. Cancer chemotherapy. In, Kaplowitz N, DeLeve LD, eds. Drug-induced liver disease. 3rd ed. Amsterdam: Elsevier, 2013, pp. 556.(Review of hepatotoxicity of cancer chemotherapeutic agents discusses several tyrosine kinase inhibitors including imatinib, gefitinib, erlotinib and crizotinib, but not palbociclib or ribociclib).
- Chabner BA, Barnes J, Neal J, Olson E, Mujagic H, Sequist L, Wilson W, et al. Targeted therapies: tyrosine kinase inhibitors, monoclonal antibodies, and cytokines. In, Brunton LL, Chabner BA, Knollman BC, eds. Goodman & Gilman's the pharmacological basis of therapeutics. 12th ed. New York: McGraw-Hill, 2011, pp. 1731-54.(Textbook of pharmacology and therapeutics).
- Turner NC, Ro J, André F, Loi S, Verma S, Iwata H, Harbeck N, et al.; PALOMA3 Study Group. Palbociclib in hormone-receptor-positive advanced breast cancer. N Engl J Med 2015; 373: 209-19. [PubMed: 26030518](Among 521 women with advanced breast cancer [ER+, HER2-] treated with letrozole and either palbociclib or placebo for up to 1 year, progression-free survival was prolonged by adding palbociclib [9.2 vs 3.8 months], and side effects were more common including neutropenia [62% vs 1%] and fatigue [38% vs 26%]; no mention of ALT elevations or hepatotoxicity).
- Mangini NS, Wesolowski R, Ramaswamy B, Lustberg MB, Berger MJ. Palbociclib: A novel cyclin-dependent kinase inhibitor for hormone receptor-positive advanced breast cancer. Ann Pharmacother 2015; 49: 1252-60. [PMC free article: PMC7331461] [PubMed: 26324355](Review of the structure, mechanism of action, pharmacology, clinical efficacy and safety of palbociclib as therapy of metastatic breast cancer, discusses neutropenia and infections, but does not mention ALT elevations or hepatotoxicity).
- Hortobagyi GN, Stemmer SM, Burris HA, Yap YS, Sonke GS, Paluch-Shimon S, Campone M, et al. Ribociclib as first-line therapy for HR-positive, advanced breast cancer. N Engl J Med 2016; 375: 1738-48. [PubMed: 27717303](Among 668 postmenopausal women with advanced breast cancer treated with letrozole with or without ribociclib, progression-free survival was improved with ribociclib and adverse events were more frequent including neutropenia [59% vs 1%], infections [4.2% vs 2.4%] and ALT elevations [15.6% vs 3.9%], which were above 5 times ULN in 9.3% vs 1.2% and accompanied by bilirubin elevations in 1.2%).
- Infante JR, Cassier PA, Gerecitano JF, Witteveen PO, Chugh R, Ribrag V, Chakraborty A, et al. A phase I study of the cyclin-dependent kinase 4/6 inhibitor ribociclib (LEE011) in patients with advanced solid tumors and lymphomas. Clin Cancer Res 2016; 23: 5696-705. [PMC free article: PMC5621377] [PubMed: 27542767](Among 132 patients with advanced solid tumors or lymphoma [Rb+] who were treated with different doses of ribociclib, dose limiting toxicities included neutropenia, thrombocytopenia, nausea, fatigue and prolongation of QTc interval; no mention of ALT elevations or hepatotoxicity).
- Spring LM, Zangardi ML, Moy B, Bardia A. Clinical Management of potential toxicities and drug interactions related to cyclin-dependent kinase 4/6 inhibitors in breast cancer: practical considerations and recommendations. Oncologist 2017; 22 (9): 1039-48. [PMC free article: PMC5599204] [PubMed: 28706010](Review of the adverse side effects of palbociclib and ribociclib and their management, including recommendations for monitoring liver tests and product label recommendations on dose adjustments for liver test abnormalities).
- Costa R, Costa RB, Talamantes SM, Helenowski I, Peterson J, Kaplan J, Carneiro BA, et al. Meta-analysis of selected toxicity endpoints of CDK4/6 inhibitors: palbociclib and ribociclib. Breast 2017; 35: 1-7. [PubMed: 28618307](Systematic review of adverse events from 7 publications on phase 2 and 3 trials of palbociclib and ribociclib discusses serious adverse events of symptoms [such as fatigue, nausea and rash], myelosuppression, neutropenic fever and thromboembolic events, but not ALT elevations or hepatotoxicity).
- Syed YY. Ribociclib: First global approval. Drugs 2017; 77: 799-807. [PubMed: 28417244](Review of the mechanism of action, pharmacokinetics, clinical efficacy, current and planned clinical trials and toxicities of ribociclib shortly after its approval in the US [March 2017]).
- O'Shaughnessy J, Petrakova K, Sonke GS, Conte P, Arteaga CL, Cameron DA, Hart LL, et al. Ribociclib plus letrozole versus letrozole alone in patients with de novo HR+, HER2- advanced breast cancer in the randomized MONALEESA-2 trial. Breast Cancer Res Treat 2018; 168: 127-34. [PMC free article: PMC5847028] [PubMed: 29164421](Secondary analysis of controlled trial ribociclib and letrozole vs letrozole alone in 668 postmenopausal women with advanced or metastatic breast cancer [Hortobagyi 2016], focusing on 227 with de novo cancer found improved progression-free survival with addition of ribociclib, but higher rates of adverse events, including any AST elevation in 17% vs 4% and values above 5 times ULN in 6% vs none).
- Hortobagyi GN, Stemmer SM, Burris HA, Yap YS, Sonke GS, Paluch-Shimon S, Campone M, Pet al. Updated results from MONALEESA-2, a phase III trial of first-line ribociclib plus letrozole versus placebo plus letrozole in hormone receptor-positive, HER2-negative advanced breast cancer. Ann Oncol 2018 Apr 27. [Epub ahead of print] [PubMed: 29718092](Further follow up of results of trial of letrozole with or without ribociclib in 668 postmenopausal women with advanced or metastatic breast cancer [Hortobagyi 2016] reported no differences in overall survival with addition of ribociclib, but higher rates of adverse events including neutropenia [77% vs 6%] and abnormal liver tests [20% vs 6%]).
- https://www
.accessdata .fda.gov/drugsatfda_docs /nda/2017/209092Orig1s000MultidisciplineR.pdf. (FDA review of the safety of ribociclib including descriptions of 4 cases of clinically apparent liver injury with jaundice; pages 145-7).
Publication Details
Publication History
Last Update: May 8, 2018.
Copyright
Publisher
National Institute of Diabetes and Digestive and Kidney Diseases, Bethesda (MD)
NLM Citation
LiverTox: Clinical and Research Information on Drug-Induced Liver Injury [Internet]. Bethesda (MD): National Institute of Diabetes and Digestive and Kidney Diseases; 2012-. Ribociclib. [Updated 2018 May 8].