OVERVIEW
Introduction
Fluphenazine is a phenothiazine and antipsychotic agent which is no longer in common use. Fluphenazine can cause mild and transient serum enzyme elevations and has been linked to rare instances of clinically apparent cholestatic liver injury.
Background
Fluphenazine (floo fen' a zeen) is a tricyclic aliphatic phenothiazine which acts by postsynaptic inhibition of dopamine receptors. Fluphenazine has other peripheral and central nervous system effects, producing both alpha adrenergic stimulation and blocking histamine- and serotonin-mediated effects. Fluphenazine was approved in the United States in 1972 for use in the therapy of acute and chronic psychosis. It was formerly a commonly prescribed antipsychotic medication, but in recent years has been replaced in large part by the atypical antipsychotics, which have fewer extrapyramidal side effects. Fluphenazine is currently used as parentral therapy of psychosis and is available generically in solution for depot injection. Fluphenazine was previously available under the brand name Prolixin. The typical maintenance dose in adults in 12.5 to 25 mg im or sc every 3 to 6 weeks. Common side effects include drowsiness, dizziness, headache, blurred vision, dry mouth, constipation, tremor, restlessness, muscle spasms and weight gain. Rare but potentially severe adverse effects include suicidal thoughts or behaviors, neuroleptic malignant syndrome and tardive dyskinesia.
Hepatotoxicity
Liver test abnormalities have been reported to occur in up to 40% of patients on long term therapy with phenothiazines, but elevations are uncommonly above 3 times the upper limit of normal. The aminotransferase abnormalities are usually mild, asymptomatic and transient, reversing even with continuation of medication. Several instances of clinically apparent acute liver injury have been reported due to fluphenazine, which have resembled the liver injury caused by chlorpromazine and other phenothiazines. The onset of phenothiazide-related jaundice is usually within 1 to 4 weeks, and the pattern of serum enzyme elevations is typically cholestatic or mixed. Immunoallergic features (fever, rash and eosinophilia) are present in some cases, but they are usually mild and self-limited; autoantibodies are rare. Most importantly, phenothiazide induced jaundice can be prolonged and associated with vanishing bile duct syndrome. All phenothiazine antipsychotic agents are probably capable of causing cholestatic liver injury, but the frequency of hepatotoxicity appears to be far greater with chlorpromazine than with others such as fluphenazine.
Likelihood score: C (probable cause of clinically apparent liver injury).
Mechanism of Injury
The mechanism by which fluphenazine and other phenothiazines cause serum aminotransferase elevations is not known. Many aspects of the clinical presentation of phenothiazine hepatotoxicity (short latency period, fever, eosinophilia) suggest a hypersensitivity reaction, and rechallenge typically causes a rapid recurrence of injury. Fluphenazine is extensively metabolized by the liver via sulfoxidation and oxidation, and some instances of serum aminotransferase elevations as well as more clinically apparent liver injury may be caused by production of a toxic intermediate of its metabolism.
Outcome and Management
The serum aminotransferase elevations that occur on fluphenazine therapy are usually self-limited and do not require dose modification or discontinuation of therapy. The acute cholestatic hepatitis caused by fluphenazine is typically self-limited and benign. While cases of prolonged jaundice and cholestasis have not been described with fluphenazine, many instances of vanishing bile duct syndrome have been attributed to other phenothiazides. Many patients with chronic cholestasis eventually improve but they often have persistent enzyme elevations and biliary cirrhosis. Fatalities from fluphenazine jaundice have not been reported. Rechallenge should be avoided. Patients with fluphenazine induced liver injury may have cross sensitivity to other phenothiazines, but generally tolerate the atypical antipsychotics.
Drug Class: Antipsychotic Agents
Other Drugs in the Subclass, Phenothiazines: Chlorpromazine, Perphenazine, Prochlorperazine, Thioridazine, Trifluoperazine
PRODUCT INFORMATION
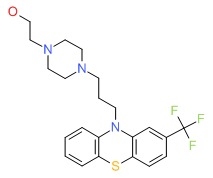
CHEMICAL FORMULA AND STRUCTURE
ANNOTATED BIBLIOGRAPHY
References updated: 02 February 2018
- Zimmerman HJ. Neuroleptic drugs. In, Zimmerman HJ. Hepatotoxicity: the adverse effects of drugs and other chemicals on the liver. 2nd ed. Philadelphia: Lippincott, 1999, pp. 483-91.(Expert review of hepatotoxicity of neuroleptic drugs including chlorpromazine published in 1999; several hundred cases of jaundice related to chlorpromazine have been reported, usually cholestatic, arising after 1-5 weeks, often with fever and eosinophilia, sometimes causing vanishing bile duct syndrome; other phenothiazines have only rarely been linked to liver injury, except for prochlorperazine).
- Larry D, Ripault MP. Hepatotoxicity of psychotropic drugs and drugs of abuse. In, Kaplowitz N, DeLeve LD, eds. Drug-induced liver disease. 3rd ed. Amsterdam: Elsevier, 2013, pp. 443-62.(Review of phenothiazine induced liver injury; liver enzyme elevations arise in up to 42% of patients treated with phenothiazines, and hundreds of cases of chlorpromazine jaundice have been published, frequency ~0.5-1%; onset in 2-5 weeks, usually with an acute cholestatic hepatitis with jaundice and pruritus; a prodrome of fever and abdominal pain is common; prolonged course in 7% but often benign; other phenothiazines including fluphenazine have been linked to liver injury similar to that of chlorpromazine, but with a lower frequency).
- Meyer JM. Pharmacotherapy of psychosis and mania. In, Brunton LL, Chabner BA, Knollman BC, eds. Goodman & Gilman’s the pharmacological basis of therapeutics. 12th ed. New York: McGraw-Hill, 2011, pp. 417-56.(Textbook of pharmacology and therapeutics).
- Walters GM, Terrence C, Steckel R. Jaundice following administration of fluphenazine dihydrochloride. Am J Psychiatry 1963; 120: 81-2. [PubMed: 13998698](29 year old woman developed rash 2 days after starting fluphenazine, followed by facial edema and then jaundice with a tender liver [bilirubin 4.7 mg/dL, Alk P ~3 times ULN], resolving within 2 weeks of stopping).
- McQueen EG. Toxic effects of phenothiazine tranquillizers. N Z Med J 1963; 62: 460-2. [PubMed: 14073060](Review of the phenothiazines and their side effects; “Jaundice has occurred in about 1% of patients taking chlorpromazine, and also, although less frequently, in patients taking one of the more recently developed analogues”).
- Walker CO, Combes B. Biliary cirrhosis induced by chlorpromazine. Gastroenterology 1966; 51: 631-40. ( [PubMed: 5926937]Two patients, a 32 year old woman and a 31 year old man developed persistent jaundice [>4 years], cholestasis and liver fibrosis 3 and 4 weeks after starting chlorpromazine; acute cholestatic hepatitis evolving into chronic form with biopsies showing cirrhosis and complications of portal hypertension).
- Ishak KG, Irey NS. Hepatic injury associated with the phenothiazines. Clinicopathologic and follow-up study of 36 patients. Arch Pathol 1972; 93: 283-304. [PubMed: 5017281](Review of 36 liver biopsies of phenothiazine induced hepatotoxicity from the files of the Armed Forces Institute of Pathology; 33 were due to chlorpromazine, 3 prochlorperazine; mean onset 15 days, eosinophilia in 73%, mean bilirubin 12.4 mg/dL, Alk P ~8 fold elevated, ALT 146 U/L; 6 [17%] had prolonged course for 10-16 months).
- Nolen WA, Börger J. Disturbances of liver function of long acting neuroleptic drugs. Pharmakopsychiatr Neuropsychopharmakol 1978; 11: 199-204. [PubMed: 674355](Analysis of 39 patients receiving fluphenazine; abnormalities of thymol turbidity were common, small number had ALT elevations, but no details given).
- Snyder S. Fluphenazine jaundice. Report of a case. Am J Gastroenterol 1980; 73: 336-40. [PubMed: 7416129](19 year old woman developed jaundice within days of starting fluphenazine [bilirubin 3.9 mg/dL, AST 2660 U/L, Alk P 181 U/L], improving over the next 2 weeks, but with rise in AST with restarting [59 to 94 U/L], and ultimately falling to normal after stopping; patient had recent history of injection drug use and report predated availability of tests for hepatitis C).
- Døssing M, Andreasen PB. Drug-induced liver disease in Denmark. An analysis of 572 cases of hepatotoxicity reported to the Danish Board of Adverse Reactions to Drugs. Scand J Gastroenterol 1982; 17: 205-11. [PubMed: 6982502](Among 572 cases of drug induced liver disease seen between 1968-78 in Denmark, 51 were attributed to chlorpromazine [9%, ranking 2nd behind halothane], latency averaging 14 days [range 11-46]; 5 deaths; no mention of fluphenazine or other phenothiazines).
- Kennedy P. Liver cross-sensitivity to antipsychotic drugs. Br J Psychiatry 1983; 143: 312. 6138114. [PubMed: 6138114](26 year old man with schizophrenia developed jaundice while on chlorpromazine [bilirubin 14.7 mg/dL, ALT 240 U/L, Alk P 294 U/L], had enzyme elevations within 2 weeks of starting haloperidol but then tolerated depixol [a thioxanthene antipsychotic not available in the US] long term).
- Jones JK, Van de Carr SW, Zimmerman H, Leroy A. Hepatotoxicity associated with phenothiazines. Psychopharmacol Bull 1983; 19: 24-7. [PubMed: 6131467](Analysis of several health databases for rates of hepatotoxicity and prescription drug use suggested that all categories of phenothiazides are associated with liver injury, being more common in persons under the age of 50 and not limited to chlorpromazine).
- Holt RJ. Fluphenazine decanoate-induced cholestatic jaundice and thrombocytopenia. Pharmacotherapy 1984; 4: 227-9. [PubMed: 6483640](30 year old man developed abdominal pain and fever ~9 months after starting intermittent fluphenazine [bilirubin 2.5 mg/dL, AST 173 U/L, Alk P 100 U/L, low platelet count], resolving rapidly with stopping fluphenazine; patient later tolerated haloperidol without liver injury).
- Kaplowitz N, Aw TY, Simon FR, Stolz A. Drug-induced hepatotoxicity. Ann Intern Med 1986; 104: 826-39. [PubMed: 3518564](Review of drug induced hepatotoxicity including phenothiazine induced jaundice).
- Munyon WH, Salo R, Briones DF. Cytotoxic effects of neuroleptic drugs. Psychopharmacology (Berl) 1987; 91: 182-8. [PubMed: 2883697](In vitro assay for cytotoxicity of 8 neuroleptic drugs found that chlorpromazine was more toxic than haloperidol and loxapine, but similar to other phenothiazines including fluphenazine).
- Regal RE, Bili JE, Glazer HM. Phenothiazine-induced cholestatic jaundice. Clinical Pharmacy 1987; 6: 787-94. [PubMed: 2905941](Review of phenothiazine induced liver injury; cross sensitivity is rare “but does exist”).
- Lok AS, Ng IO. Prochlorperazine-induced chronic cholestasis. J Hepatol 1988; 6: 369-73. [PubMed: 3392386](68 year old man developed jaundice 4 weeks after starting prochlorperazine [peak bilirubin 26 mg/dL, ALT 50-90 U/L, Alk P 120-500 U/L], jaundice and pruritus persisting for more than a year, but then gradual clinical improvement but with persistent enzyme elevations, and biopsy 22 months after onset showed fibrosis and paucity of bile ducts).
- Pillans PI. Drug associated hepatic reactions in New Zealand: 21 years experience. NZ Med J 1996; 109: 315-9. [PubMed: 8816722](Over 21 year period in New Zealand, there were 943 adverse event reports of liver injury involving 205 drugs; chlorpromazine was in the top 20 drugs implicated accounting for 2.7% of cases; prochlorperazine was the cause of 4 cases, but other phenothiazines were not mentioned).
- Sabaté M, Ibáñez L, Pérez E, Vidal X, Buti M, Xiol X, Mas A, et al. Risk of acute liver injury associated with the use of drugs: a multicentre population survey. Aliment Pharmacol Ther 2007; 25: 1401-9. [PubMed: 17539979](Among 126 cases of drug induced liver injury seen in Spain between 1993-2000, 3 were due to chlorpromazine with relative risk of 613: frequency of 261 per 100,000 person year exposures; no mention of fluphenazine).
- Aruna AS, Murungi JH. Fluphenazine-induced neuroleptic malignant syndrome in a schizophrenic patient. Ann Pharmacother 2005; 39: 1131-5. [PubMed: 15840734](21 year old man developed fever, tremors, obtundation and tachycardia 7 days after an injection of fluphenazine while continuing thioridazine, haloperidol, lithium and carbamazepine [bilirubin normal, ALT 116 U/L, AST 410 U/L, CPK 36,696], resolving with intensive medical support; enzyme elevations likely from muscle).
- Chalasani N, Fontana RJ, Bonkovsky HL, Watkins PB, Davern T, Serrano J, Yang H, Rochon J; Drug Induced Liver Injury Network (DILIN). Causes, clinical features, and outcomes from a prospective study of drug-induced liver injury in the United States. Gastroenterology 2008; 135: 1924-34. [PMC free article: PMC3654244] [PubMed: 18955056](Among 300 cases of drug induced liver disease in the US collected between 2004 and 2008, none were attributed to phenothiazines).
- Reuben A, Koch DG, Lee WM; Acute Liver Failure Study Group. Drug-induced acute liver failure: results of a U.S. multicenter, prospective study. Hepatology 2010; 52: 2065-76. [PMC free article: PMC3992250] [PubMed: 20949552](Among 1198 patients with acute liver failure enrolled in a US prospective study between 1998 and 2007, 133 were attributed to drug induced liver injury including 4 due to psychotropic agents; one each for quetiapine, nefazodone, fluoxetine and venlafaxine, but none for phenothiazines).
- Molleston JP, Fontana RJ, Lopez MJ, Kleiner DE, Gu J, Chalasani N; Drug-induced Liver Injury Network. Characteristics of idiosyncratic drug-induced liver injury in children: results from the DILIN prospective study. J Pediatr Gastroenterol Nutr 2011; 53: 182-9. [PMC free article: PMC3634369] [PubMed: 21788760](Among 30 children with suspected drug induced liver injury, half [n=15] were due to antimicrobials [minocycline 4, INH 3, azithromycin 3] and the rest largely due to CNS agents and anticonvulsants; one case was attributed to perphenazine).
- Marwick KF, Taylor M, Walker SW. Antipsychotics and abnormal liver function tests: systematic review. Clin Neuropharmacol 2012; 35: 244-53. [PubMed: 22986798](Systematic review of the literature found rates of any serum enzyme elevation during antipsychotic therapy to range from 5-78% and "clinically significant' elevations in 0-15%; lists 3 reports of clinically apparent liver injury due to fluphenazine, none of which were fatal [Holt 1984; Snyder 1980; Kennedy 1983]).
- Drugs for psychiatric disorders. Treat Guidel Med Lett 2013; 11 (130): 53-64. [PubMed: 23715100](Concise review and recommendations on use of antidepressants and antipsychotic medications including fluphenazine; no discussion of hepatotoxicity).
- Björnsson ES, Bergmann OM, Björnsson HK, Kvaran RB, Olafsson S. Incidence, presentation and outcomes in patients with drug-induced liver injury in the general population of Iceland. Gastroenterology 2013; 144: 1419-25. [PubMed: 23419359](In a population based study of drug induced liver injury from Iceland, 96 cases were identified over a 2 year period including one non-fatal but icteric case due to chlorpromazine, but none to fluphenazine).
- Hernández N, Bessone F, Sánchez A, di Pace M, Brahm J, Zapata R, A Chirino R, et al. Profile of idiosyncratic drug induced liver injury in Latin America: an analysis of published reports. Ann Hepatol 2014; 13: 231-9. [PubMed: 24552865](Among 176 reports of drug induced liver injury from Latin America published between 1996 and 2012, one non-fatal, but icteric case [from 2003] was attributed to chlorpromazine but none to fluphenazine).
- Chalasani N, Bonkovsky HL, Fontana R, Lee W, Stolz A, Talwalkar J, Reddy KR, et al.; United States Drug Induced Liver Injury Network. Features and outcomes of 899 patients with drug-induced liver injury: The DILIN Prospective Study. Gastroenterology 2015; 148: 1340-52.e7. [PMC free article: PMC4446235] [PubMed: 25754159](Among 899 cases of drug induced liver injury enrolled in a US prospective study between 2004 and 2013, 5 [0.4%] were attributed to antipsychotic agents, including 3 to quetiapine and 2 olanzapine, but none phenothiazines such as fluphenazine).
- Drugs for psychotic disorders. Med Lett Drugs Ther 2016; 58 (1510): 160-4. [PubMed: 27960194](Concise review of medications available in the US for therapy of psychotic disorders; mentions fluphenazine, but does not discuss hepatotoxicity).
Publication Details
Publication History
Last Update: February 2, 2018.
Copyright
Publisher
National Institute of Diabetes and Digestive and Kidney Diseases, Bethesda (MD)
NLM Citation
LiverTox: Clinical and Research Information on Drug-Induced Liver Injury [Internet]. Bethesda (MD): National Institute of Diabetes and Digestive and Kidney Diseases; 2012-. Fluphenazine. [Updated 2018 Feb 2].