OVERVIEW
Introduction
Usnic acid is a furandione found uniquely in lichen that is used widely in cosmetics, deodorants, toothpaste and medicinal creams as well as some herbal products. Taken orally, usnic acid can be toxic and has been linked to instances of clinically apparent, acute liver injury.
Background
Usnic acid is a dibenzo-furandione which is uniquely found in lichen (Usnea) species, which are distributed worldwide. In vitro usnic acid has antibacterial, antifungal and antiviral activities, and lichen extracts containing usnic acid have been used in folk medicine externally for wound healing and athlete’s foot and internally for sore throat, toothache and fever. Usnic acid has also found several commercial uses, largely in perfumery and cosmetic products, but also in medicinal creams. However, usnic acid appears to be toxic when taken orally in high doses and, for instance, can cause ataxia and paralysis in animals grazing on lichen contaminated crops and grains. Usnic acid has been purified and extensively studied in vitro and has been shown to uncouple oxidative phosphorylation in isolated mitochondria, which may account for its broad antimicrobial activity. Uncoupling of oxidative phosphorylation by decreasing the efficacy of energy use and causing increased thermogenesis has been proposed as an approach to treatment of obesity. However, this approach is potentially dangerous and has not been shown to be effective in causing weight loss other than by extreme toxicity. Nevertheless, usnic acid has been used in several commercial over-the-counter weight loss products.
Hepatotoxicity
Several cases of clinically apparent acute liver injury have been attributed to commercial dietary supplements that contain usnic acid. “LipoKinetix” was one such supplement advertised as a weight loss and body building supplement. Each tablet contained sodium usniate (100 mg), norephedrine (25 mg), diiodothyronine (100 mg), yohimbine (3 mg) and caffeine (100 mg). The product has been linked to multiple instances of acute liver injury. The time to onset was 2 to 12 weeks and the clinical presentation resembled acute viral hepatitis with onset of fatigue and nausea, followed by jaundice. The pattern of serum enzyme elevations was hepatocellular, with marked elevations in serum ALT and minimal increases in alkaline phosphatase levels. Liver biopsy demonstrated acute hepatocellular necrosis and inflammation. Immunoallergic features (fever, rash and eosinophilia) were not common and autoantibodies were usually not present. Recovery was rapid with stopping the dietary supplement, but some cases were severe and led to acute liver failure and either death or need for emergency liver transplantation. Instances of acute hepatitis have also been reported with other multi-ingredient dietary supplements that contain usnic acid, but much more rarely than with LipoKinetix which was withdrawn from distribution after a FDA warning letter. Rare instances of hepatotoxicity have also been reported with use of lichen based teas known as Kombucha tea, but whether these were due to usnic acid or another contaminant of the tea was not shown.
Likelihood score (usnic acid): B (highly likely cause of clinically apparent liver injury).
Likelihood score (Kombucha tea): C (probable cause of clinically apparent liver injury).
Mechanism of Injury
The hepatotoxicity of usnic acid is probably caused by uncoupling of oxidative phosphorylation in the liver, which can produce hepatocyte lysis and apoptosis and induces acute liver injury in animal models.
Outcome and Management
Hepatotoxicity attributed usnic acid and products such as LipoKinetix is often clinically apparent, but is usually reversible with prompt discontinuation of the nutritional supplement. Usnic acid is a direct hepatotoxin and thus is unlikely to share cross sensitivity to liver injury with other agents.
Drug Class: Herbal and Dietary Supplements
CASE REPORT
Case 1. Acute liver failure due to usnic acid.
[Modified from case 1 of: Sanchez W, Maple JT, Burgart LJ, Kamath PS. Severe hepatotoxicity associated with use of a dietary supplement containing usnic acid. Mayo Clinic Proc 2006; 81: 541-4. PubMed Citation].
A 38 year old woman developed fatigue, abdominal discomfort and jaundice 3 months after starting a multiingredient health supplement called UCP-1, which contained usnic acid. She was previously well and had no history of liver disease, alcohol abuse or risk factors for viral hepatitis. She had been on oral contraceptives and received a 2 week course of tinidazole 3 weeks before presentation. She was a fitness trainer at a health club in Asia, and she and her husband started taking the health supplement UCP-1 as an aid to body building in the recommended dose of 3 capsules 3 times daily, each capsule containing usnic acid (150 mg), L-carnitine (525 mg) and calcium pyruvate (1050 mg). She was hospitalized at which time her bilirubin was 23.0 mg/dL and serum aminotransferase levels markedly elevated (ALT 1636 U/L, AST 1536 U/L), while alkaline phosphatase levels were minimally increased (195 U/L) (Table). When she developed signs of hepatic encephalopathy, she was transferred to a liver transplant center in the United States. Over the next few days she developed worsening hepatic failure and underwent emergency liver transplantation. Tests for hepatitis A, B and C were negative as were autoimmune markers and tests for Wilson disease. The explant demonstrated massive necrosis and collapse. She recovered after transplant and was discharged a week later. Her husband had also used the nutritional supplement and, although not symptomatic, had marked elevations in serum aminotransferase values (ALT 1462 U/L, AST 451 U/L) with normal bilirubin levels. After stopping the supplement, his serum liver tests began to improve and were normal four months later.
Key Points
Laboratory Values
Comment
Usnic acid taken as a weight loss supplement has been associated with at least a dozen published cases of acute liver injury which, as in this case, can be severe, leading to acute liver failure and death or need for emergency liver transplantation. The fact that both husband and wife developed liver injury while on UCP-1 is in favor of its role in causing the injury, but they also shared common exposures and therefore the episode could also be due to common infectious agent. Nevertheless, the clinical presentation and course were entirely compatible with usnic acid associated hepatotoxicity.
PRODUCT INFORMATION
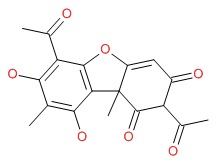
CHEMICAL FORMULA AND STRUCTURE
ANNOTATED BIBLIOGRAPHY
References updated: 25 April 2018
- Zimmerman HJ. Unconventional drugs. Miscellaneous drugs and diagnostic chemicals. In, Zimmerman, HJ. Hepatotoxicity: the adverse effects of drugs and other chemicals on the liver. 2nd ed. Philadelphia: Lippincott,1999: pp. 731-4.(Expert review of hepatotoxicity published in 1999; unconventional drugs including Kombucha tea are discussed, but not usnic acid).
- Seeff L, Stickel F, Navarro VJ. Hepatotoxicity of herbals and dietary supplements. In, Kaplowitz N, DeLeve LD, eds. Drug-induced liver disease. 3rd ed. Amsterdam: Elsevier, 2013, pp. 631-58.(Review of hepatotoxicity of herbal and dietary supplements [HDS]; usnic acid is listed as a cause of acute liver failure and was a component of Lipokinetix, a commercial product that has been withdrawn from the market).
- Usnea. In, PDR for Herbal Medicines. 4th ed. Montvale, New Jersey: Thomson Healthcare Inc. 2007: pp. 867-8.(Compilation of short monographs on herbal medications and dietary supplements).
- Perron AD, Patterson JA, Yanofsky NN. Kombucha “mushroom” hepatotoxicity. Ann Emerg Med 1995; 26: 660-1. [PubMed: 7486385](53 year old man developed fever, rash and abdominal cramping 4 weeks after starting and 2 weeks after stopping Kombucha tea [bilirubin normal, ALT 285 U/L, Alk P 168 U/L], resolving 1 month later).
- Centers for Disease Control. Unexplained severe illness possibly associated with consumption of Kombucha tea – Iowa, 1995. MMWR 1995; 44: 892-900. [PubMed: 7476846](Two patients from a rural town in Iowa developed severe unexplained illness [lactic acidosis and cardiopulmonary collapse] after taking Kombucha tea for 2 months; cause was not identified).
- Srinivasan R, Smolinske S, Greenbaum D. Probable gastrointestinal toxicity of Kombucha tea: is this beverage healthy or harmful? J Gen Intern Med 1997; 12: 643-4. [PMC free article: PMC1497178] [PubMed: 9346462](55 year old woman with history of heavy alcohol use developed jaundice 2 months after starting a daily intake of Kombucha tea [bilirubin 5.3 mg/dL, ALT 585 U/L, Alk P 203 U/L], resolving within 7 weeks of stopping; 3 other patients developed symptoms of toxicity without liver abnormalities while drinking Kombucha tea).
- Ingolfsdottir K. Usnic acid. Phytochemistry 2002; 61: 729-36. [PubMed: 12453567](Usnic acid is a lichen metabolite used in creams, toothpaste, deodorants and as a preservative; also has antimicrobial activity and recently promoted as weight loss agent; toxic in high doses, it can cause paralysis, ataxia and acidosis).
- Favreau JT, Ryu ML, Braunstein G, Orshansky G, Park SS, Coody GL, Love LA, Fong TL. Severe hepatotoxicity associated with the dietary supplement LipoKinetix. Ann Intern Med 2002; 136: 590-5.(7 patients, 4 women and 3 men, ages 20-32 years, developed symptoms and jaundice [n=5] or liver test abnormalities [n=2], 1-12 weeks after starting LipoKinetix [norephedrine, usniate, diiodothyronine, yohimbine, caffeine] for weight loss [peak bilirubin 2.2-14.6 mg/dL, ALT 438-14,150 U/L], resolving in 1-3 months of stopping).
- 'Dietary supplement' warning. FDA Consum 2002; 36: 4. [PubMed: 11989472](FDA warning of the potential hepatotoxicity of usnic acid containing weight loss products).
- Lewis JD, Strom BL. Balancing safety of dietary supplements with the free market. Ann Intern Med 2002; 136: 616-8.(Editorial on Favreau [2002] regarding Lipo-Kinetix and the regulation of dietary supplements in the US).
- Estes JD, Stolpman D, Olyaei A, Corless CL, Ham JM, Schwartz JM, Orloff SL. High prevalence of potentially hepatotoxic herbal supplement use in patients with fulminant hepatic failure. Arch Surg 2003; 138: 852-8. [PubMed: 12912743](Among 20 patients undergoing liver transplantation for acute liver failure during 2001-2, 10 were potentially caused by herbals: 3 due to Ma Huang, 3 kava, 2 LipoKinetix [usnic acid], 1 chaparral, 1 skullcap and 2 miscellaneous Chinese herbs).
- Russo MW, Galanko JA, Shrestha R, Fried MW, Watkins P. Liver transplantation for acute liver failure from drug-induced liver injury in the United States. Liver Transpl 2004; 10: 1018-23. [PubMed: 15390328](Among ~50,000 liver transplants reported to UNOS between 1990 and 2002, 270 [0.5%] were done for drug induced acute liver failure, including 7 [5%] due to herbal medications; usnic acid was not specifically mentioned).
- Durazo FA, Lassman C, Han SH, Saab S, Lee NP, Kawano M, Saggi B, et al. Fulminant liver failure due to usnic acid for weight loss. Am J Gastroenterol 2004; 99: 950-2. [PubMed: 15128366](28 year old woman developed nausea and fatigue 2 weeks after starting usnic acid and, despite stopping it, developed jaundice, confusion and hepatic failure requiring liver transplantation [bilirubin 28 mg/dL, ALT 449 U/L, AST 1016 U/L, INR 4.6]; the explant demonstrated massive necrosis).
- Neff GW, Reddy KR, Durazo FA, Meyer D, Marrero R, Kaplowitz N. Severe hepatotoxicity associated with the use of weight loss diet supplements containing ma huang or usnic acid. J Hepatol 2004; 41: 1062-4. [PubMed: 15582145](Summary report of 12 patients who developed liver injury after taking herbal weight loss products including two who were taking Lipokinetix [bilirubin 20 and 35 mg/dL, ALT 1500 and 1420, Alk P not given], one of whom recovered and one underwent transplantation).
- Willett KL, Roth RA, Walker L. Workshop overview: Hepatotoxicity assessment for botanical dietary supplements. Toxicol Sci 2004; 79: 4-9. [PubMed: 14976355](Summary of a workshop on the hepatotoxicity of botanicals focusing upon mechanisms of hepatic injury and means of prediction and prevention).
- Han D, Matsumaru K, Tettori D, Kaplowitz N. Usnic acid-induced necrosis of cultured mouse hepatocytes: inhibition of mitochondrial function and oxidative stress. Biochem Pharmacol 2004; 67: 439-51. [PubMed: 15037196](Usnic acid caused necrosis of isolated mouse hepatocytes probably by uncoupling of electron transport in mitochondria, oxidative stress and depletion of glutathione).
- Hsu LM, Huang YS, Chang FY, Lee SD. ‘Fat burner’ herb, usnic acid, induced acute hepatitis in a family. J Gastroenterol Hepatol 2005; 20: 1138-9. [PubMed: 15955234](3 sisters with toxicity from herbal “fat burner” consisting of soybean extract and usnic acid; 36 year old woman had abdominal pain 2 weeks after starting herbal [bilirubin normal, ALT 442 U/L, Alk P 217 U/L], resolving within 6 weeks; 32 year old sister developed jaundice after 4 weeks of use [bilirubin 29 mg/dL, ALT 778 U/L, Alk P 118 U/L, INR 2.6], resolving in 4 months; third sister stopped the herbal after 3 days because of fatigue).
- Arneborn P, Jansson A, Böttiger Y. [Acute hepatitis in a woman after intake of slimming pills bought via Internet]. Lakartidningen 2005; 102: 2071-2. Swedish. [PubMed: 16097177](20 year old overweight woman developed nausea followed by jaundice 4 weeks after starting a weight loss agent [Termoxical, containing usnic acid] purchased over the Internet [bilirubin 4.9 mg/dL, ALT 1320 U/L, Alk P 198 U/L], resolving within a month of stopping).
- Sanchez W, Maple JT, Burgart LJ, Kamath PS. Severe hepatotoxicity associated with use of a dietary supplement containing usnic acid. Mayo Clinic Proc 2006; 81: 541-4. [PubMed: 16610575](Two cases: 38 year old woman developed jaundice 3 months after starting UCP-1 in a dose of 1350 mg daily [bilirubin 23.0 mg/dL, ALT 1636 U/L, Alk P 195 U/L, protime 22.7 sec], progressing to hepatic failure and successful liver transplantation [Case 1]; 38 year old husband of previous case developed back pain 3 months after starting UCP-1 [bilirubin 0.6 mg/dL, ALT 1462 U/L], with rapid resolution on stopping and normal values 4 months later).
- Chitturi S, Farrell GC. Hepatotoxic slimming aids and other herbal hepatotoxins. J Gastroenterol Hepatol 2008; 23: 366-73. [PubMed: 18318821](Review of hepatotoxicity of herbal medications focusing upon those used for weight loss, including nitrosofenfluramine, usnic acid, ephedra, germander, skullcap and green tea).
- Foti RS, Dickmann LJ, Davis JA, Greene RJ, Hill JJ, Howard ML, Pearson JT, et al. Metabolism and related human risk factors for hepatic damage by usnic acid containing nutritional supplements. Xenobiotica 2008; 38: 264-80. [PubMed: 18274956](In vitro analyses of effects of usnic acid on hepatic cytochrome P450 enzymes found that it was a potent inhibitor of CYP 2C19 and 2C9, suggesting that it could cause significant drug-herb interactions).
- Guo L, Shi Q, Fang JL, Mei N, Ali AA, Lewis SM, Leakey JE, Frankos VH. Review of usnic acid and Usnea barbata toxicity. J Environ Sci Health C Environ Carcinog Ecotoxicol Rev 2008; 26: 317-38. [PMC free article: PMC5739313] [PubMed: 19034791](Usnea extracts have been used in traditional Chinese medicine for centuries as an antimicrobial and for other uses, including in cosmetics, food, toothpaste and mouthwash; in vitro, it has mitochondrial uncoupling properties and was therefore used for weight loss; FDA has received 21 adverse event reports including 1 death attributed to dietary supplements containing usnic acid [LipoKinetix and UCP-1] and 12 cases have appeared in the literature, leading to warnings and recommendations for it to be withdrawn).
- Chalasani N, Fontana RJ, Bonkovsky HL, Watkins PB, Davern T, Serrano J, Yang H, Rochon J; Drug Induced Liver Injury Network (DILIN). Causes, clinical features, and outcomes from a prospective study of drug-induced liver injury in the United States. Gastroenterology 2008; 135: 1924-34. [PMC free article: PMC3654244] [PubMed: 18955056](Among 300 cases of drug induced liver disease in the US collected between 2004 and 2008, 9% of cases were attributed to herbal medications, usnic acid was not listed).
- Navarro VJ. Herbal and dietary supplement hepatotoxicity. Semin Liver Dis 2009; 29: 373-82. [PubMed: 19826971](Overview of the regulatory environment, clinical patterns, and future directions in research with HDS including traditional Chinese herbal medicines and usnic acid).
- Jacobsson I, Jönsson AK, Gerdén B, Hägg S. Spontaneously reported adverse reactions in association with complementary and alternative medicine substances in Sweden. Pharmacoepidemiol Drug Saf 2009; 18: 1039-47. [PubMed: 19650152](Review of 778 spontaneous reports of adverse reactions to herbals to Swedish Registry does not mention usnic acid specifically).
- SungHee Kole A, Jones HD, Christensen R, Gladstein J. A case of Kombucha tea toxicity. J Intensive Care Med 2009; 24 205-7. [PubMed: 19460826](22 year old man with HIV infection developed fever and agitation a day after drinking a large amount of Kombucha tea, presenting with lactic acidosis and fever [bilirubin and Alk P normal, ALT 57 U/L, lactate 12.9 mmol/L, arterial pH 7.21], resolving within 72 hours with supportive care only).
- Reuben A, Koch DG, Lee WM; Acute Liver Failure Study Group. Drug-induced acute liver failure: results of a U.S. multicenter, prospective study. Hepatology 2010; 52: 2065-76. [PMC free article: PMC3992250] [PubMed: 20949552](Among 1198 patients with acute liver failure enrolled in a US prospective study between 1998 and 2007, 133 [11%] were attributed to drug induced liver injury, of which 12 [9%] were due to herbals, including 2 due to usnic acid).
- Stickel F, Kessebohm K, Weimann R, Seitz HK. Review of liver injury associated with dietary supplements. Liver Int 2011; 31: 595-605. [PubMed: 21457433](Review of current understanding of liver injury from herbals and dietary supplements focusing upon herbalife and hydroxycut products, green tea, usnic acid, Noni juice, Chinese herbs, vitamin A and anabolic steroids).
- Yellapu RK, Mittal V, Grewal P, Fiel M, Schiano T. Acute liver failure caused by 'fat burners' and dietary supplements: a case report and literature review. Can J Gastroenterol 2011; 25: 157-60. [PMC free article: PMC3076034] [PubMed: 21499580](28 year old woman developed jaundice one month after starting two "fat burners" [Somalyz and Lipolyz] containing usnic acid as an aid to body building [bilirubin 4.8 mg/dL, ALT 1220 U/L, Alk P 111 U/L, INR 2.6], with rapid progression to acute liver failure requring liver transplantation; the explant showed massive necrosis).
- Bunchorntavakul C, Reddy KR. Review article: herbal and dietary supplement hepatotoxicity. Aliment Pharmacol Ther 2013; 37: 3-17. [PubMed: 23121117](Systematic review of literature on HDS associated liver injury mentions that usnic acid has been implicated in causing clinically apparent hepatotoxicity).
- Björnsson ES, Bergmann OM, Björnsson HK, Kvaran RB, Olafsson S. Incidence, presentation and outcomes in patients with drug-induced liver injury in the general population of Iceland. Gastroenterology 2013; 144: 1419-25. [PubMed: 23419359](In a population based study of drug induced liver injury from Iceland, 96 cases were identified over a 2 year period, including 15 attributed to herbals or dietary supplements, but none were linked to usnic acid containing products specifically).
- Licata A, Macaluso FS, Craxì A. Herbal hepatotoxicity: a hidden epidemic. Intern Emerg Med 2013; 8: 13-22. [PubMed: 22477279](Review and commentary on herbal hepatotoxicity with specific focus on ephedra, germander, kava, chapararal, black cohosh, greater celandine, usnic acid, and Herbalife, Hydroxycut and LipoKinetix products).
- Navarro VJ, Seeff LB. Liver injury induced by herbal complementary and alternative medicine. Clin Liver Dis 2013; 17: 715-35. [PubMed: 24099027](Review of HDS induced liver injury including regulatory problems, difficulties in diagnosis and causality assessment, includes specific comments on usnic acid).
- de Oliveira AV, Rocha FT, Abreu SR. Acute liver failure and self-medication. Arq Bras Cir Dig 2014; 27: 294-7. [PMC free article: PMC4743226] [PubMed: 25626943](Review of published literature on acute liver failure associated with self-medication identified cases related to acetaminophen, GTE, linoleic acid, rhamnus purshianus [Fitosoja] and usnic acid).
- Navarro VJ, Barnhart H, Bonkovsky HL, Davern T, Fontana RJ, Grant L, Reddy KR, et al. Liver injury from herbals and dietary supplements in the U.S. Drug-Induced Liver Injury Network. Hepatology 2014; 60: 1399-408. [PMC free article: PMC4293199] [PubMed: 25043597](Among 85 cases of HDS associated liver injury [not due to anabolic steroids] enrolled in a US prospective study between 2004 and 2013, the single most commonly implicated herbal agent was green tea extract; usnic acid not specifically mentioned or listed).
- Seeff LB, Bonkovsky HL, Navarro VJ, Wang G. Herbal products and the liver: a review of adverse effects and mechanisms. Gastroenterology 2015; 148: 517-32. [PubMed: 25500423](Extensive review of possible beneficial as well as harmful effects of herbal products on the liver; no specific discussion of usnic acid).
- Stickel F, Shouval D. Hepatotoxicity of herbal and dietary supplements: an update. Arch Toxicol. 2015; 89: 851-65. [PubMed: 25680499](Extensive review of liver injury due to HDS discusses usnic acid which was introduced as a potential weight loss agent because of its activity in uncoupling oxidative phosphorylation, but which also can cause mitochondrial injury and has been implicated in cases of acute hepatitis which can be severe and has resulted in fatalities, leading to FDA warnings and its withdrawal from the market).
- Chalasani N, Bonkovsky HL, Fontana R, Lee W, Stolz A, Talwalkar J, Reddy KR, et al.; United States Drug Induced Liver Injury Network. Features and outcomes of 899 patients with drug-induced liver injury: The DILIN Prospective Study. Gastroenterology 2015; 148: 1340-52. [PMC free article: PMC4446235] [PubMed: 25754159](Among 899 cases of drug induced liver injury enrolled in a prospective database between 2004 and 2012, HDS were implicated in 145 [16%], the single major herbal cause being green tea extract; usnic acid was not discussed).
- Zheng EX, Navarro VJ. Liver injury from herbal, dietary, and weight loss supplements: a review. J Clin Transl Hepatol 2015; 3: 93-8. [PMC free article: PMC4548352] [PubMed: 26357638](Review of literature on liver injury due to HDS products used for weight loss, focusing upon the case series of liver injury attributed to green tea as well as the commercial products that appear to contain it such as Herbalife and Hydroxycut, the injury of which was predominantly hepatocellular [acute hepatitis-like] and had a significant mortality rate).
- Gedela M, Potu KC, Gali VL, Alyamany K, Jha LK. A case of hepatotoxicity related to Kombucha tea consumption. S D Med 2016; 69: 26-8. [PubMed: 26882579](58 year old woman developed jaundice 1 month after starting daily Kombucha tea use [bilirubin 4.1 rising to 7.5 mg/dL, ALT 330 U/L, Alk P 630 U/L], resolving within 1 month of stopping the herbal tea).
- García-Cortés M, Robles-Díaz M, Ortega-Alonso A, Medina-Caliz I, Andrade RJ. Hepatotoxicity by dietary supplements: A tabular listing and clinical characteristics. Int J Mol Sci 2016; 17. pii: E537. (Listing of published cases of liver injury from HDS products, including cases of hepatitis and acute liver failure due to usnic acid). [PMC free article: PMC4848993] [PubMed: 27070596]
- Brown AC. Liver toxicity related to herbs and dietary supplements: Online table of case reports. Part 2 of 5 series. Food Chem Toxicol 2017; 107 (Pt A): 472-501. [PubMed: 27402097](Description of an online compendium of cases of liver toxicity attributed to HDS products, lists at least 46 published cases of green tea associated liver injury and concludes that green tea may warrant a warning label).
- Wong LL, Lacar L, Roytman M, Orloff SL. Urgent liver transplantation for dietary supplements: an under-recognized problem. Transplant Proc 2017; 49: 322-5. [PubMed: 28219592](Among 2048 adult liver transplants recipients enrolled in the Scientific Registry of Transplant Recipients [SRTR] between 2003 and 2015, 625 were done for acute hepatic necrosis due to drug induced liver injury, half being due to acetaminophen and the 4th most frequent cause [n=21] being HDS products, although none were specifically listed as containing usnic acid).
- Vega M, Verma M, Beswick D, Bey S, Hossack J, Merriman N, Shah A, et al; Drug Induced Liver Injury Network (DILIN). The incidence of drug- and herbal and dietary supplement-induced liver injury: preliminary findings from gastroenterologist-based surveillance in the population of the State of Delaware. Drug Saf 2017; 40: 783-7. [PMC free article: PMC5699929] [PubMed: 28555362](A prospective, population based registry of cases of drug induced liver injury occurring in Delaware during 2014, identified 20 cases [2.7 per 100,000] overall, including 6 due to HDS products, all of which were proprietary multiingredient products, but none listed usnic acid as a component).
Publication Details
Publication History
Last Update: April 25, 2018.
Copyright
Publisher
National Institute of Diabetes and Digestive and Kidney Diseases, Bethesda (MD)
NLM Citation
LiverTox: Clinical and Research Information on Drug-Induced Liver Injury [Internet]. Bethesda (MD): National Institute of Diabetes and Digestive and Kidney Diseases; 2012-. Usnic Acid. [Updated 2018 Apr 25].