OVERVIEW
Introduction
Colestipol is a nonabsorbed bile acid sequestrant that is used a therapy of hyperlipidemia and for the pruritus of chronic liver disease and biliary obstruction. Colestipol has not been associated with clinically apparent liver injury.
Background
Colestipol (koe les' ti pol) is a large, highly positively charged anion exchange resin that binds to negatively charged anions such as bile acids (as well as other organic compounds and some medications). The binding of bile acids to colestipol creates an insoluble compound that cannot be reabsorbed and is thus excreted in the feces. Bile acids ordinarily undergo extensive (>95%) enterohepatic recirculation, being secreted in bile, acting as fat solubilizing compounds in the upper intestine, and then being reabsorbed in the distal small bowel. Chronic loss of bile acids from colestipol use results in a contraction of the total bile acid pool. The liver compensates for this decrease by increasing bile acid synthesis, which directly competes with cholesterol synthesis resulting in a decrease in serum levels of cholesterol. Some of the decrease in serum cholesterol may also result from inhibition of fat absorption by the binding of bile acids to colestipol. Colestipol was approved for use in the United States in 1977 and is one of the oldest and safest cholesterol lowering agents, but it is currently used largely as an adjunctive therapy when statins or other lipid lowering agents result in an inadequate decrease in cholesterol levels. Colestipol is used off-label to reduce the pruritus of chronic liver disease probably as a result of binding the “pruritogen” in the intestine (which is either a bile acid or an organic anion like a bile acid that undergoes enterohepatic circulation). Colestipol is available in multiple generic forms and under the brand name of Colestid as a tablet of 2 grams or as powdered granules. The usual dose of colestipol tablets is 2 grams daily increasing to a maximum of 16 grams; whereas, that for the granules is 5 grams daily increasing to a maximum of 30 grams, based upon tolerance and effect. Colestipol is best given before meals and at bedtime. Other drugs should be given 1 hour before or 4 to 6 hours after colestipol. Colestipol granules can be unpalatable and difficult to swallow. Other side effects include abdominal discomfort, indigestion, nausea, flatuence and constipation.
Hepatotoxicity
There is little evidence that colestipol causes liver injury. Mild elevations in serum aminotransferase and alkaline phosphatase levels have been reported in small numbers of patients on bile acid resins, although the elevations have been mild, transient and without accompanying symptoms. In addition, a case report of more marked aminotransferase elevations (>10 times ULN) with rapid recovery on stopping colestipol has been published, but the mechanism by which it might cause hepatotoxicity is very unclear. Colestipol is used in patients with liver disease to treat pruritus, and has little or no effect on serum enzyme or bilirubin levels.
Likelihood score: E (unlikely cause of clinically apparent liver injury with jaundice).
Mechanism of Injury
The lack of hepatic injury by colestipol is probably due to the fact that it is not absorbed, and the contraction of the bile acid pool caused by its use does not harm the liver. Because colestipol can interfere with the absorption of other medications or vitamins, it may indirectly worsen liver disease by lowering effective levels of medications. These effects are particularly important for vitamins A, D, E, K, hormones such as estrogens, corticosteroids, and thyroid hormone, and medications such as thiazide diuretics, acetaminophen and digoxin.
References on the safety and hepatotoxicity of colestipol are given with those for colesevelam and cholestyramine in the Overview section on Bile Acid Resins/Sequestrants.
Drug Class: Antilipemic Agents, Bile Acid Resins/Sequestrants
PRODUCT INFORMATION
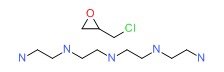
CHEMICAL FORMULA AND STRUCTURE
Publication Details
Publication History
Last Update: September 28, 2017.
Copyright
Publisher
National Institute of Diabetes and Digestive and Kidney Diseases, Bethesda (MD)
NLM Citation
LiverTox: Clinical and Research Information on Drug-Induced Liver Injury [Internet]. Bethesda (MD): National Institute of Diabetes and Digestive and Kidney Diseases; 2012-. Colestipol. [Updated 2017 Sep 28].