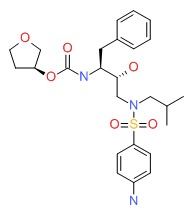
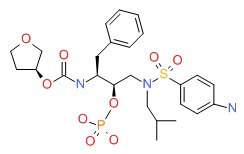
Fosamprenavir
OVERVIEW
Introduction
Amprenavir is an antiretroviral protease inhibitor used in the therapy and prevention of human immunodeficiency virus (HIV) infection and the acquired immunodeficiency syndrome (AIDS). Fosamprenavir is a prodrug of amprenavir that has better oral bioavailability and that has largely replaced amprenavir in clinical use. Both amprenavir and fosamprenavir can cause transient and usually asymptomatic elevations in serum aminotransferase levels and are rare causes of clinically apparent, acute liver injury. In coinfected patients, hepatic injury during highly active antiretroviral therapy may be a result of exacerbation of the underlying chronic hepatitis B or C rather than a direct toxic effect of the medication.
Background
Amprenavir (am pren' a vir) is sulfonamide nonpeptide HIV protease inhibitor that acts by binding to the catalytic site of the viral protease, thereby preventing the cleavage of HIV polyprotein precursors into mature, functional proteins that are necessary for viral replication. Fosamprenavir (fos" am pren' a vir) is a phosphonooxy prodrug of amprenavir which is more water soluble and has greater bioavailability than amprenavir. Fosamprenavir is rapidly converted to amprenavir in the intestinal mucosa. Amprenavir was approved for use in the United States in 1999 and fosamprenavir in 2003 for the therapy of HIV infection in adults and children in combination with other antiretroviral agents. Amprenavir was previously available in capsules of 50 mg under the brand name Agenerase. The pill burden of amprenavir therapy made fosamprenavir preferable and amprenavir is no longer availble in the United States. Fosamprenavir is available in tablets of 700 mg and in a liquid solution for pediatric use (50 mg/mL) under the brand name Lexiva. Both agents are typically used in combination with low "booster" doses of ritonavir (100 or 200 mg daily). The recommended dose of fosamprenavir is 1400 mg twice daily when given without ritonavir or 1400 mg once daily when given with ritonavir. The dose in children is weight based. Common side effects include diarrhea, nausea, gastrointestinal upset, headache, fatigue and, with long term use, hyperlipidemia and lipodystrophy.
Hepatotoxicity
Some degree of serum aminotransferase elevations occur in a high proportion of patients taking amprenavir or fosamprenavir containing antiretroviral regimens. In large, multicenter trials of fosamprenavir based antiretroviral therapy, moderate-to-severe elevations in serum aminotransferase levels (>5 times the upper limit of normal) were found in 3% to 10% of patients. Rates of enzyme elevations are higher in patients with HIV-HCV coinfection then in those with monoinfection. These elevations are usually asymptomatic and self-limited and can resolve even with continuation of the medication. Furthermore, similar rates of enzyme elevations were found in comparator arms (using other HIV protease inhibitors).
Clinically apparent acute liver injury due to amprenavir or fosamprenavir is rare and the specific clinical features have not been characterized in any detail. The few cases of symptomatic liver injury that have been reported have arisen after 1 to 8 weeks of starting the agent, and the pattern of serum enzyme elevations has not been well defined, but probably largely hepatocellular (Cases 1 and 2). Signs of hypersensitivity (fever, rash, eosinophilia) can occur, but autoantibody formation is rare. The acute liver injury due to HIV protease therapy is usually self-limited, but it can be severe, and isolated cases of acute liver failure have been reported with some agents. In HBV or HCV coinfected patients, acute liver injury may be caused by an exacerbation of the underlying chronic liver disease, perhaps as a result of sudden immune reconstitution. Neither amprenavir nor fosamprenavir have been clearly linked to lactic acidosis and acute fatty liver that is reported in association with several nucleoside analogue reverse transcriptase inhibitors.
Likelihood score: D (possible rare cause of clinically apparent liver injury)
Mechanism of Injury
The cause of the clinical hepatotoxicity from amprenavir or fosamprenavir is not well understood. Amprenavir is extensively metabolized by the liver, largely by the cytochrome P450 system (CYP 3A4), and toxic or immunogenic intermediates may be the cause of some liver injury. Clinically apparent cases of liver injury have had many features of hypersensitivity. In patients with HIV infection who are coinfected with either HBV or HCV, initiation of potent antiretroviral therapy may be associated with flares of the underlying chronic hepatitis which may be the result of reconstitution of the immune system, viral interactions or a direct effect of the drug.
Outcome and Management
The severity of the liver injury from amprenavir or fosamprenavir ranges from mild and transient enzyme elevations to more marked and symptomatic enzyme elevations and, rarely, to acute hepatitis which is usually self-limited. Typically, improvements start within a few days of stopping therapy and recovery is usually rapid. Rechallenge with either or switching from one to the other is likely to lead to recurrence and should be avoided. There is little evidence for cross reactivity to the hepatotoxicity of amprenavir and fosamprenavir with other HIV protease inhibitors.
References to amprenavir and fosprenavir are included with references to all the HIV protease inhibitors in the Overview section of Protease Inhibitors (updated September 2017). Most of the HIV protease inhibitors in clinical use are proteinomimetic drugs and are structurally unrelated.
Drug Class: Antiviral Agents, Antiretroviral Agents
Other Drugs in the Subclass, Protease Inhibitors: Atazanavir, Darunavir, Indinavir, Lopinavir, Nelfinavir, Ritonavir, Saquinavir, Tipranavir
CASE REPORTS
Case 1. Liver injury during fosamprenavir therapy for post exposure prophylaxis.
[Modified from: Pavel S, Burty C, Alcaraz I, de la Tribonnière X, Baclet V, Ajana F, Mouton Y, et al. Severe liver toxicity in postexposure prophylaxis for HIV infection with a zidovudine, lamivudine and fosamprenavir/ritonavir regimen. AIDS 2007; 21: 268-9. PubMed Citation]
A 22 year old woman with an acute exposure to an individual suspected to have HIV and HCV developed nausea and abdominal pain 8 days after starting a prophylactic regimen of lamivudine, zidovudine and fosamprenavir/ritonavir. Blood tests taken one week later showed ALT of 517 U/L without HCV RNA or HIV viremia. She had received HBV vaccine and was anti-HBs positive. The antiretroviral agents were stopped and serum aminotransferase levels were normal 2 weeks later. She remained free of both HCV and HIV infection.
Key Points
Comment
Scant information is provided, but the patient appeared to have elevations in serum aminotransferase levels two weeks after starting combination antiretroviral therapy, including fosamprenavir with low dose ritonavir. This regimen is also associated with gastrointestinal symptoms (abdominal pain and nausea) independent of hepatic injury and it is not clear whether the symptoms and the ALT elevations were related. Interestingly, this regimen was not associated with high rates of hepatotoxicity in clinical trials and other case series, but has been associated with precipitation of hepatic decompensation in patients with cirrhosis due to hepatitis C.
Case 2. Liver toxicity after post exposure prophylaxis with fosamprenavir in 29 year old male.
[Modified from: Pavel S, Burty C, Alcaraz I, de la Tribonnière X, Baclet V, Ajana F, Mouton Y, et al. Severe liver toxicity in postexposure prophylaxis for HIV infection with a zidovudine, lamivudine and fosamprenavir/ritonavir regimen. AIDS 2007; 21: 268-9. PubMed Citation]
A 29 year old man, undergoing postexposure prophylaxis after a sexual exposure to HIV, developed a generalized maculopapular rash after 9 days of therapy with lamivudine, zidovudine and fosamprenavir/ritonavir. Physical examination suggested the diagnosis of erythema multiforme. Serum ALT was 958 U/L, but neither HCV RNA nor HIV viremia were detected. Both HBsAg and anti-HBc were also negative. The antiretrovirals were stopped. He improved and six weeks later the rash was gone and serum aminotransferase levels were normal.
Key Points
Comment
Another case from the same investigators with few details of the nature and course of the hepatic injury (no bilirubin, alkaline phosphatase or INR results). The patient appeared to develop an acute hypersensitivity reaction after 9 days of an antiretroviral regimen that included fosamprenavir and low dose ritonavir (as well as lamivudine and zidovudine). Acute hypersensitivity reactions due to medications with rash, fever and eosinophilia are frequently accompanied by evidence of hepatitis, sometimes with symptoms and jaundice, but more frequently with serum aminotransferase elevations without hyperbilirubinemia.
PRODUCT INFORMATION
REPRESENTATIVE TRADE NAMES
Amprenavir – Agenerase®
Fosamprenavir – Lexiva®
DRUG CLASS
Antiviral Agents
Product labeling at DailyMed, National Library of Medicine, NIH
CHEMICAL FORMULAS AND STRUCTURES
Publication Details
Publication History
Last Update: September 1, 2017.
Copyright
Publisher
National Institute of Diabetes and Digestive and Kidney Diseases, Bethesda (MD)
NLM Citation
LiverTox: Clinical and Research Information on Drug-Induced Liver Injury [Internet]. Bethesda (MD): National Institute of Diabetes and Digestive and Kidney Diseases; 2012-. Fosamprenavir. [Updated 2017 Sep 1].