11.1.1. What Is CDSS?
Clinical decision support includes a variety of tools and interventions, computerized as well as non- computerized. Non-computerized tools include clinical guidelines or digital clinical decision support resources like ClinicalKey® or UpToDate ® [1, 2]. Such clinical decision support systems (CDSS) are characterized as tools for information management. Another category of CDSS sometimes also called basic or simple clinical decision support systems are tools to help focus attention. Examples of such CDSS include laboratory information systems (LISs) highlighting critical care values or pharmacy information systems (PISs) presenting an alert ordering a new drug and proposing a possible drug-drug interaction [3, 4]. Most focus in the past few decades however has gone to tools to provide patient-specific recommendations called advanced CDSS. Advanced CDSS mayinclude, for example, checking drug disease interactions, individualized dosing support during renal impairment, or recommendations on laboratory testing during drug use.
11.1.2. Why CDSS?
The quantity and quality of clinical data are rapidly expanding, including electronic health records (EHRs), disease registries, patient surveys and information exchanges. Big data and digitalization however, does not automatically mean better patient care. Several studies have shown that only implementing an EHRand computerized physician order entry (CPOE) has rapidly decreased the incidence of certain errors, introducing however many more [5–7]. Therefore, high-quality clinical decision support is essential if healthcare organizations are to achieve the full benefits of electronic health records and CPOE. In the current healthcare setting when facing a decision, healthcare providers often do not know that certain patient data are available in the EHR, do not always know how to access the data, do not have the time to search for the data or are not fully informed on the most current medical insights. It is said the healthcare providers often drown in the midst of plenty [8–10].
Moreover, decisions by healthcare professionals are often made during direct patient contact, ward rounds or multidisciplinary meetings. This means that many decisions are made in a matter of seconds or minutes, and depend on the healthcare provider having all patient parameters and medical knowledge readily available at that time of the decision. Consequently, current decisions are still strongly determined by experience and knowledge of the professional. Also, subtle changes in a patient’s condition taking place before hospital- or ward admission are often overlooked because clinicians regularly perceive a patient in his current state without taking into account changes within normal range. A computer however, takes into account all data available making it also possible to notice changes outside the scope of the professional and notices changes specific for a certain patient, within normal limits.
11.1.3. Types of CDSS
To understand literature on the topic of CDSS and familiarize oneself on the subject it is important to categorize the vast array of CDSS. Categorization of CDSS is often based on the following characteristics: system function, model for giving advice, style of communication, underlying decision making process and human computer interaction which are briefly explained below [11].
The characteristic ‘System function’ distinguishes two types of functions. Systems determining: what is true?: These include purely diagnostic CDSS like many popular differential diagnosis websites like Diagnosaurus® or WebMD® [12, 13]. These CDSS base their advices on a fixed set of data that is user inputted or readily available. The other type of CDSS determine: what to do?, advising which test to order with the purpose of further differential diagnosis or which drug to prescribe for the patient’s current condition. However, this distinction is of limited value as most current integrated CDSS almost always do both: first determine what is true about a patient and then suggest what to do.
Another parameter of CDSS is the approach to give advice, either passive or active. Passive CDSS require the user to do something to receive advice, for example clicking a button or opening a tab. These passive types however, have been abandoned for most part because of their lack of efficacy and dependence of human involvement [14, 15]. A challenge of active systems is to avoid the generation of excessive amount of alerts, causing alert fatigue with the user. This topic is discussed further on in the paragraph on alert fatigue. A closely related characteristic commonly used to categorize CDSS is thestyle of communication, distinguishing a consulting and critiquing model. In a consulting model the system is an advisor, asking questions and proposes subsequent actions. For example, when entering a medication order, the computer asks for the diagnosis and advises the right dose or an alternative treatment. A critiquing system lets the user decide the right dose for itself and only afterwards alerts the user that the dose prescribed for this therapy is too low.
Human computer interaction is another clinical decision support system characteristic. How does a user interact with the computer? Historically CDSS were slow, difficult to access and difficult to use. However, modern day computing power, electronic health record integration and computer mobility have made these problems of the past. However, human computer interaction is still a good way to categorize CDSS describing EHR integration or overlay, keyboard or voice recognition and advice by means of pop-ups, acoustic alarms or messaging systems.
The last commonly used characterization of CDSS, and perhaps the most interesting, is the underlying decision-making process ormodel. The simplest models are problem-specific flowcharts encoded for computerized use, these are discussed further on. With the availability of additional statistical models, mathematical techniques and increasing computing power, much more complex models have been researched and used since, like Bayesian models [16, 17], artificial neural networks [18], support vector machines [19] and artificial intelligence [20]. Many of these systems are used to improve prediction of outcome, prioritize treatment or help choosing the best course of action. Use of such systems in practice however is delayed mainly because of trust issues towards ‘black box’ systems. If a computer tells you to start drug A for a patient based solely on a mathematical model, without a guideline to back it up, are you convinced to do it? Linked to the major trust issue towards ‘black box’ systems is the current model of evidence based medicine and concurrent guidelines based on these studies. Are you willing to ignore an international guideline saying you should start a patient on drug A only because your CDSS says you should start the patient on drug B?
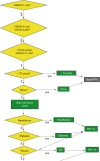
Decision tree models are the oldest but still most used models in clinical practice today. These CDSS use a tree-like model of decisions consisting of multiple steps of ‘if then else’ logic. Figure shows an example of such a decision tree model. These models have the advantage of being interpretable by humans and follow logical steps based on conventional medical guidelines. Such decision tree models are also called clinical rules (CRs), computer-interpretable guidelines (CIGs) or decision support algorithms. [15] Instead of predicting outcome or best therapy, a CDSS only automatizes information gathering and provides advice in accordance to a guideline.
Part of the clinical rule gastric protection, represented in GLIF, created in CDSS Gaston (Medecs BV). (Picture adopted from Scheepers et al. 2009 [14])
The next few paragraphs will focus on CDSS that determine both what is true? and what to do?, as well as the use of mainly active critiquing advice and the use of a decision tree model as underlying decision making process.
11.1.4. Medication Related CDSS
From a historical point of view, medication related CDSS seem to go the farthest back and are likely to have the largest potential for benefit [21]. They date back as long as the 1960s [22]. They supported pharmacists with drug allergy checking, dose guidance, drug-drug interaction checking and duplicate therapy checking. Medication related CDSS took further shape when directly linked to computerized physician order entry (CPOE) [23]. CPOE being the system that enabled physicians to prescribe medication using electronic entry. The combination of CPOE and CDSS helped physicians choose the right drug in the right dose and alert the physician during prescribing if for example the patient is allergic. Combining CPOE with basic medication related CDSS meant a giant leap in safer medication prescribing [24, 25]. However, all of the checks mentioned above follow simple ‘if then else’ logic and do not combine multiple patient characteristics when producing alerts. This addition came with the introduction of advanced medication related CDSS.
Such advanced CDSS follow decision tree based models and can assist the physician in dosing medication for patients with renal insufficiency, provide guidance for medication-related laboratory testing and perform drug – disease contraindication checking [23, 26]. Parameters incorporated into medication related CDSS rose steadily in the past few decades including pharmacogenetics and more and more drug disease interactions.
Many current EHRs with integrated CDSS however, still fail to provide guidance relevant to the specific patient receiving care, poorly presenting data and causing alert fatigue to health care providers [27]. One of the main issues with these systems is that they combine only one or two parameters to provide alerts, thereby only increasing the number of alerts. For example, prescribing nortriptyline to a patient with hepatorenal syndrome and being an intermediate metabolizer of CYP2D6 will generate a total of 3 alerts with different advices. An advice on how to dose nortriptyline in a patient with renal insufficiency, another alert with an advice how to dose nortriptyline in patients with liver failure and last but not least an advice how to start treatment in a patient being an CYP2D6 intermediate metabolizer. So which advice should we follow? Therefore, effort should be made into combining multiple parameters and clinical rules to provide one correct advice to the healthcare provider. Designs should incorporate the engagement of all clinicians involved in the delivery of health care and combine multiple patient characteristics and context simultaneously, to ensure that CDSS are actually helpful to clinicians, rather than interrupt health care delivery.


 2.
2.