Attribution Statement: LactMed is a registered trademark of the U.S. Department of Health and Human Services.
NCBI Bookshelf. A service of the National Library of Medicine, National Institutes of Health.
Drugs and Lactation Database (LactMed®) [Internet]. Bethesda (MD): National Institute of Child Health and Human Development; 2006-.
CASRN: 608137-32-2
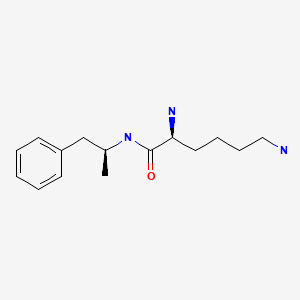
Drug Levels and Effects
Summary of Use during Lactation
Lisdexamfetamine is a prodrug of dextroamphetamine. In dosages prescribed for medical indications, some evidence indicates that dextroamphetamine might not affect nursing infants adversely. The effect of dextroamphetamine in milk on the neurological development of the infant has not been well studied. It is possible that large dosages of dextroamphetamine might interfere with milk production, especially in women whose lactation is not well established. Relevant published information was not found as of the revision date on the safety of breastfeeding during amphetamine abuse. One expert recommends that amphetamines not be used therapeutically in nursing mothers.[1]
Drug Levels
Maternal Levels. Four mothers averaging 5.5 months postpartum (range 3.3 to 10 months)were taking dextroamphetamine in an average dosage of 18 mg daily (range 15 to 45 mg daily in 2 to 4 divided doses) for attention deficit hyperactivity disorder. The median milk level was 219 mcg/L (range 66 to 313 mcg/L) which resulted in an infant dosage of 21 mcg/kg (range 11 to 39 mcg/kg) daily or 5.7% (range 4 to 10.6%) of the maternal weight-adjusted dosage.[2]
Infant Levels. Dextroamphetamine blood levels were measured in 3 breastfed infants. The mothers of these 3 infants were taking an average of 392 mcg/kg daily of dextroamphetamine. Blood levels in 2 infants were 2 and 18 mcg/L, corresponding to 6 and 14% of the maternal plasma level. The plasma level of the third infant was <1 mcg/L. The times of blood collection were not stated.[2]
Effects in Breastfed Infants
The author of a 1973 newsletter reported a personal communication from the drug manufacturer which stated that of 103 nursing mothers treated with dextroamphetamine (dosage unspecified) for postpartum depression, no infant showed any evidence of stimulation or insomnia.[3]
Four mothers averaging 5.5 months postpartum (range 3.3 to 10 months) were taking dextroamphetamine in an average dosage of 18 mg daily (range 15 to 45 mg daily in 2 to 4 divided doses) for attention deficit hyperactivity disorder. Their infants had been breastfed (extent not stated) since birth. The infants all had weights between the 10th and 75th percentiles for their age, normal progress, and no adverse effects according to their pediatricians. Denver developmental ages for 2 of the infants were 100% and 117% of normal.[2]
A prospective study followed 13 women who were taking an amphetamine (7 mixed racemic amphetamine salts [Adderal] and 6 lisdexamfetamine) during breastfeeding (9 exclusively). Median age of the child at the follow-up was 18 (IRQ 5.25 to 34) months. Adverse effects were reported among 5 children: somnolence in 1, crying or restlessness in 3, and colic or constipation in 4. All children were reported to have normal gross motor development, based on the Denver developmental scale. Neurodevelopment was also normal with median PEDsQL score of 97.16, psychosocial health score 99.33 and physical health score 98.75.[4]
Effects on Lactation and Breastmilk
In 2 papers by the same authors, 20 women with normal physiologic hyperprolactinemia were studied on days 2 or 3 postpartum. Eight received dextroamphetamine 7.5 mg intravenously, 6 received 15 mg intravenously and 6 who served as controls received intravenous saline. The 7.5 mg dose reduced serum prolactin by 25 to 32% compared to control, but the difference was not statistically significant. The 15 mg dose significantly decreased serum prolactin by 30 to 37% at times after the infusion. No assessment of milk production was presented.[5,6] The authors also quoted data from another study showing that a 20 mg oral dose of dextroamphetamine produced a sustained suppression of serum prolactin by 40% in postpartum women. The maternal prolactin level in a mother with established lactation may not affect her ability to breastfeed.
In a retrospective Australian study, mothers who used intravenous amphetamines during pregnancy were less likely to be breastfeeding their newborn infants at discharge than mothers who abused other drugs (27% vs 42%). The cause of this difference was not determined.[7]
Alternate Drugs to Consider
(ADHD) Amphetamine, Dextroamphetamine, Methylphenidate (Narcolepsy) Amphetamine, Armodafinil, Dextroamphetamine, Methylphenidate, Modafinil, Oxybate Salts, Pitolisant
References
- 1.
- Ornoy A. Pharmacological treatment of attention deficit hyperactivity disorder during pregnancy and lactation. Pharm Res 2018;35:46. [PubMed: 29411149]
- 2.
- Wang BP, Li QL, Hu YF. [Impact of epidural anesthesia during delivery on breast feeding]. Di Yi Jun Yi Da Xue Xue Bao 2005;25:114-5, 118. [PubMed: 15684016]
- 3.
- Ayd FJ. Excretion of psychotropic drugs in human breast milk. Int Drug Ther Newsl 1973;8:33-40.
- 4.
- Hazan A, Kaduri NB, De-Haan T, et al. I am a law student treated with amphetamines for Attention Deficit Hyperactive Disorder (ADHD): Can I breastfeed my child? A pilot study. Neurotoxicol Teratol 2023;98:15. doi:10.1016/j.ntt.2023.107219 [CrossRef]
- 5.
- DeLeo V, Cella SG, Camanni F, et al. Prolactin lowering effect of amphetamine in normoprolactinemic subjects and in physiological and pathological hyperprolactinemia. Horm Metab Res 1983;15:439-43.
- 6.
- Petraglia F, De Leo V, Sardelli S, et al. Prolactin changes after administration of agonist and antagonist dopaminergic drugs in puerperal women. Gynecol Obstet Invest 1987;23:103-9. [PubMed: 3583091]
- 7.
- Oei J, Abdel-Latif ME, Clark R, et al. Short-term outcomes of mothers and infants exposed to antenatal amphetamines. Arch Dis Child Fetal Neonatal Ed 2010;95:F36-F41. [PubMed: 19679891]
Substance Identification
Substance Name
Lisdexamfetamine
CAS Registry Number
608137-32-2
Drug Class
Breast Feeding
Milk, Human
Adrenergic Agents
Central Nervous System Stimulants
Dopamine Agents
Sympathomimetics
Wakefulness-Promoting Agents
Disclaimer: Information presented in this database is not meant as a substitute for professional judgment. You should consult your healthcare provider for breastfeeding advice related to your particular situation. The U.S. government does not warrant or assume any liability or responsibility for the accuracy or completeness of the information on this Site.
- User and Medical Advice Disclaimer
- Drugs and Lactation Database (LactMed) - Record Format
- LactMed - Database Creation and Peer Review Process
- Fact Sheet. Drugs and Lactation Database (LactMed)
- Drugs and Lactation Database (LactMed) - Glossary
- LactMed Selected References
- Drugs and Lactation Database (LactMed) - About Dietary Supplements
- Breastfeeding Links
- PubChem SubstanceRelated PubChem Substances
- PubMedLinks to PubMed
- Review Dextroamphetamine.[Drugs and Lactation Database (...]Review Dextroamphetamine.. Drugs and Lactation Database (LactMed®). 2006
- Review Amphetamine.[Drugs and Lactation Database (...]Review Amphetamine.. Drugs and Lactation Database (LactMed®). 2006
- Review Lisdexamfetamine.[Paediatr Drugs. 2007]Review Lisdexamfetamine.Blick SK, Keating GM. Paediatr Drugs. 2007; 9(2):129-35; discussion 136-8.
- Review Methamphetamine.[Drugs and Lactation Database (...]Review Methamphetamine.. Drugs and Lactation Database (LactMed®). 2006
- Comparison of lisdexamfetamine and dextroamphetamine exposures reported to U.S. poison centers.[Clin Toxicol (Phila). 2015]Comparison of lisdexamfetamine and dextroamphetamine exposures reported to U.S. poison centers.Kaland ME, Klein-Schwartz W. Clin Toxicol (Phila). 2015 Jun; 53(5):477-85. Epub 2015 Apr 2.
- Lisdexamfetamine - Drugs and Lactation Database (LactMed®)Lisdexamfetamine - Drugs and Lactation Database (LactMed®)
Your browsing activity is empty.
Activity recording is turned off.
See more...
