Attribution Statement: LactMed is a registered trademark of the U.S. Department of Health and Human Services.
NCBI Bookshelf. A service of the National Library of Medicine, National Institutes of Health.
Drugs and Lactation Database (LactMed®) [Internet]. Bethesda (MD): National Institute of Child Health and Human Development; 2006-.
CASRN: 93413-62-8
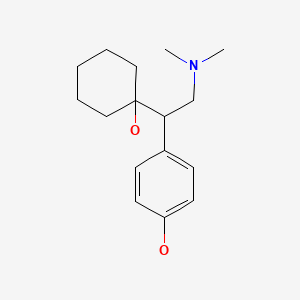
Drug Levels and Effects
Summary of Use during Lactation
Modest doses of desvenlafaxine are excreted into breastmilk, but serum drug levels of breastfed infants are less than 10% of simultaneous maternal levels. Total drug exposure of breastfed infants is about half of that experienced by breastfed infants whose mothers are taking venlafaxine.[1]. With the related drug venlafaxine, newborn infants of mothers who took the drug during pregnancy sometimes experienced poor neonatal adaptation as seen with other antidepressants such as SSRIs or SNRIs. Similar effects may occur with desvenlafaxine. Monitor breastfed infants for excessive sedation and adequate weight gain if this drug is used during lactation, especially newborn or preterm infants.
Drug Levels
Desvenlafaxine (O-desmethylvenlafaxine) is an active metabolite of venlafaxine with similar antidepressant activity.[2]
Maternal Levels. Ten lactating women with postpartum depression who were an average of 4.3 (range 0.9 to 12.7) months postpartum were taking extended-release desvenlafaxine (Pristiq) from 4 to 35 days in doses of 50 to 150 mg daily or an average of 1.2 mg/kg daily (95% CI: 0.93 to 1.5 mg/kg daily). Each woman provided up to 8 milk samples over a 24-hour period. Peak milk concentrations occurred at an average of 3.3 hours after the dose. An exclusively breastfed infant in this study would have received an estimated 85 mcg/kg daily or 6.8% (95% CI: 5.5 to 8.1%) of the maternal weight-adjusted dosage.[1]
A nursing mother was taking oral desvenlafaxine 250 mg and amisulpride 100 mg twice daily. Eight breastmilk samples were obtained over a 24-hour period with a breast pump. The average breastmilk concentration was 1.9 mg/L which equated to an infant dose of 0.29 mg/kg daily or 7.8% of the maternal weight-adjusted dosage.[3]
Infant Levels. Ten infants with an average age of 4.3 (range 0.9 to 12.7) months were breastfed (8 exclusively) during maternal use of desvenlafaxine in doses of 50 to 150 mg daily or an average of 1.2 mg/kg daily. The infants had an average serum desvenlafaxine level of 16 mcg/L, which averaged 4.8% of the simultaneous maternal serum concentration taken at about 6.5 hours after the maternal dose. Considering only the exclusively breastfed infants, infant exposure would have averaged 5.8% of the maternal serum concentration.[1]
A nursing mother was taking oral desvenlafaxine 250 mg and amisulpride 100 mg twice daily for 12.6 weeks. Her partially breastfed infant was 5 months old. The infant's serum desvenlafaxine concentration 3.1 hours after the mother's daily dose was 13 mcg/L or 1.7% of the maternal serum concentration.[3]
Effects in Breastfed Infants
Ten infants ranging in age from 0.9 to 12.7 months were breastfed (8 exclusively) during maternal use of desvenlafaxine in doses of 50 to 150 mg daily or an average of 1.2 mg/kg daily. Mothers were also taking lorazepam (n = 6), quetiapine (n = 5), lamotrigine (n = 2), levonorgestrel (n = 2), domperidone (n = 1), and temazepam (n = 1). Infants were studied after an average of 9 days of exposure (range 4 to 35 days) of desvenlafaxine exposure via breastmilk. At the time of the study, 7 of the 10 infants were at a lower growth percentile than at the time of birth. Examination by a pediatrician found that all infants were healthy and had Denver developmental scores that matched their age on the day of the study.[1]
A woman with depressive type schizoaffective disorder was taking lurasidone 40 mg at night and desvenlafaxine 50 mg daily after giving birth. She exclusively breastfed her infant. The infant’s growth and development was good during a follow-up period of 39 days.[4]
Effects on Lactation and Breastmilk
In an outpatient study that followed 1395 patients who received long-term desvenlafaxine therapy, 2 patients developed elevated serum prolactin levels and one developed galactorrhea.[5] The clinical relevance of these findings in nursing mothers is not known. The prolactin level in a mother with established lactation may not affect her ability to breastfeed.
An observational study looked at outcomes of 2859 women who took an antidepressant during the 2 years prior to pregnancy. Compared to women who did not take an antidepressant during pregnancy, mothers who took an antidepressant during all 3 trimesters of pregnancy were 37% less likely to be breastfeeding upon hospital discharge. Mothers who took an antidepressant only during the third trimester were 75% less likely to be breastfeeding at discharge. Those who took an antidepressant only during the first and second trimesters did not have a reduced likelihood of breastfeeding at discharge.[6] The antidepressants used by the mothers were not specified.
A retrospective cohort study of hospital electronic medical records from 2001 to 2008 compared women who had been dispensed an antidepressant during late gestation (n = 575) to those who had a psychiatric illness but did not receive an antidepressant (n = 1552) and mothers who did not have a psychiatric diagnosis (n = 30,535). Women who received an antidepressant were 37% less likely to be breastfeeding at discharge than women without a psychiatric diagnosis, but no less likely to be breastfeeding than untreated mothers with a psychiatric diagnosis.[7] None of the mothers were taking desvenlafaxine.
In a study of 80,882 Norwegian mother-infant pairs from 1999 to 2008, new postpartum antidepressant use was reported by 392 women and 201 reported that they continued antidepressants from pregnancy. Compared with the unexposed comparison group, late pregnancy antidepressant use was associated with a 7% reduced likelihood of breastfeeding initiation, but with no effect on breastfeeding duration or exclusivity. Compared with the unexposed comparison group, new or restarted antidepressant use was associated with a 63% reduced likelihood of predominant, and a 51% reduced likelihood of any breastfeeding at 6 months, as well as a 2.6-fold increased risk of abrupt breastfeeding discontinuation. Specific antidepressants were not mentioned.[8]
Alternate Drugs to Consider
References
- 1.
- Rampono J, Teoh S, Hackett LP, et al. Estimation of desvenlafaxine transfer into milk and infant exposure during its use in lactating women with postnatal depression. Arch Womens Ment Health 2011;14:49-53. [PubMed: 20960017]
- 2.
- Weissman AM, Levy BT, Hartz AJ, et al. Pooled analysis of antidepressant levels in lactating mothers, breast milk, and nursing infants. Am J Psychiatry 2004;161:1066-78. [PubMed: 15169695]
- 3.
- Ilett KF, Watt F, Hackett LP, et al. Assessment of infant dose through milk in a lactating woman taking amisulpride and desvenlafaxine for treatment-resistant depression. Ther Drug Monit 2010;32:704-7. [PubMed: 20926994]
- 4.
- Keightley P, Schmidt Sotomayor N, O'Hara K, et al. Lurasidone in lactation: A case study with laboratory and clinical outcomes. Aust N Z J Psychiatry 2020;54:1035-6. [PubMed: 32611245]
- 5.
- Tourian KA, Pitrosky B, Padmanabhan SK, Rosas GR. A 10-month, open-label evaluation of desvenlafaxine in outpatients with major depressive disorder. Prim Care Companion CNS Disord 2011;13:PCC.10m00977. [PMC free article: PMC3184590] [PubMed: 21977353]
- 6.
- Venkatesh KK, Castro VM, Perlis RH, Kaimal AJ. Impact of antidepressant treatment during pregnancy on obstetric outcomes among women previously treated for depression: An observational cohort study. J Perinatol 2017;37:1003-9. [PMC free article: PMC10034861] [PubMed: 28682318]
- 7.
- Leggett C, Costi L, Morrison JL, et al. Antidepressant use in late gestation and breastfeeding rates at discharge from hospital. J Hum Lact 2017;33:701-9. [PubMed: 28984528]
- 8.
- Grzeskowiak LE, Saha MR, Nordeng H, et al. Perinatal antidepressant use and breastfeeding outcomes: Findings from the Norwegian Mother, Father and Child Cohort Study. Acta Obstet Gynecol Scand 2022;101:344-54. [PMC free article: PMC9564556] [PubMed: 35170756]
Substance Identification
Substance Name
Desvenlafaxine
CAS Registry Number
93413-62-8
Drug Class
Breast Feeding
Milk, Human
Antidepressive Agents
Serotonin-Norepinephrine Reuptake Inhibitors
Disclaimer: Information presented in this database is not meant as a substitute for professional judgment. You should consult your healthcare provider for breastfeeding advice related to your particular situation. The U.S. government does not warrant or assume any liability or responsibility for the accuracy or completeness of the information on this Site.
- User and Medical Advice Disclaimer
- Drugs and Lactation Database (LactMed) - Record Format
- LactMed - Database Creation and Peer Review Process
- Fact Sheet. Drugs and Lactation Database (LactMed)
- Drugs and Lactation Database (LactMed) - Glossary
- LactMed Selected References
- Drugs and Lactation Database (LactMed) - About Dietary Supplements
- Breastfeeding Links
- PMCPubMed Central citations
- PubChem SubstanceRelated PubChem Substances
- PubMedLinks to PubMed
- Review Venlafaxine.[Drugs and Lactation Database (...]Review Venlafaxine.. Drugs and Lactation Database (LactMed®). 2006
- Desvenlafaxine in the treatment of major depressive disorder.[Neuropsychiatr Dis Treat. 2009]Desvenlafaxine in the treatment of major depressive disorder.Lourenco MT, Kennedy SH. Neuropsychiatr Dis Treat. 2009; 5:127-36. Epub 2009 Apr 8.
- Review Citalopram.[Drugs and Lactation Database (...]Review Citalopram.. Drugs and Lactation Database (LactMed®). 2006
- False-positive phencyclidine (PCP) on urine drug screen attributed to desvenlafaxine (Pristiq) use.[BMJ Case Rep. 2017]False-positive phencyclidine (PCP) on urine drug screen attributed to desvenlafaxine (Pristiq) use.Farley TM, Anderson EN, Feller JN. BMJ Case Rep. 2017 Nov 23; 2017. Epub 2017 Nov 23.
- Analysis of treatment patterns and persistence on branded and generic medications in major depressive disorder using retrospective claims data.[Neuropsychiatr Dis Treat. 2016]Analysis of treatment patterns and persistence on branded and generic medications in major depressive disorder using retrospective claims data.Solem CT, Shelbaya A, Wan Y, Deshpande CG, Alvir J, Pappadopulos E. Neuropsychiatr Dis Treat. 2016; 12:2755-2764. Epub 2016 Oct 25.
- Desvenlafaxine - Drugs and Lactation Database (LactMed®)Desvenlafaxine - Drugs and Lactation Database (LactMed®)
Your browsing activity is empty.
Activity recording is turned off.
See more...
