CASRN: 12650-69-0
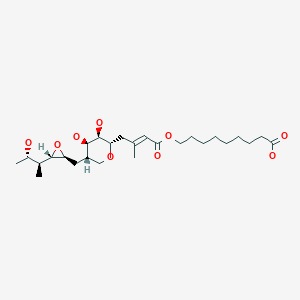
Drug Levels and Effects
Summary of Use during Lactation
Because less than 1% is absorbed after topical application, mupirocin is considered a low risk to the nursing infant.[1] Ensure that the infant's skin does not come into direct contact with the areas of skin that have been treated. Only water-miscible cream or gel products should be applied to the breast because ointments may expose the infant to high levels of mineral paraffins via licking.[2] Mupirocin applied topically to the nipples appears to be relatively ineffective as a treatment for sore, cracked nipples.
Drug Levels
Maternal Levels. Relevant published information was not found as of the revision date.
Infant Levels. Relevant published information was not found as of the revision date.
Effects in Breastfed Infants
A mother who was exclusively nursing her 52-day-old infant developed a soft-tissue infection. She was treated with intravenous teicoplanin 400 mg every 12 hours for 3 doses, then 400 mg daily for 5 days total, intravenous ceftriaxone 1 gram daily, topical mupirocin cream twice daily. A careful follow-up indicated that her infant had no adverse effects.[3]
Effects on Lactation and Breastmilk
A small, randomized, unblinded trial of mothers with sore, cracked nipples was performed. Mupirocin 2% applied to the nipples after each feeding was much less effective (16% vs 79%) than an oral antibiotic (cloxacillin or erythromycin for 10 days) in resolving the problem. Additionally, more patients' condition worsened (28% vs 5%) with mupirocin than with an oral antibiotic.[4]
In a randomized, double-bind trial, lanolin was compared to an all-purpose nipple ointment containing mupirocin 1%, betamethasone 0.05%, and miconazole 2% for painful nipples while nursing in the first 2 weeks postpartum. The two treatments were equally effective in reducing nipple pain, nipple healing time, breastfeeding duration, breastfeeding exclusivity rate, mastitis and nipple symptoms, side effects or maternal satisfaction with treatment.[5]
Alternate Drugs to Consider
References
- 1.
- Leachman SA, Reed BR. The use of dermatologic drugs in pregnancy and lactation. Dermatol Clin. 2006;24:167-97. [PubMed: 16677965]
- 2.
- Noti A, Grob K, Biedermann M et al. Exposure of babies to C(15)-C(45) mineral paraffins from human milk and breast salves. Regul Toxicol Pharmacol. 2003;38:317-25. [PubMed: 14623482]
- 3.
- Kaplan YC, Keskin-Arslan E, Acar S et al. Teicoplanin use during breastfeeding. Breastfeed Med. 2017. [PubMed: 28051878]
- 4.
- Livingstone V, Stringer LJ. The treatment of Staphyloccocus aureus infected sore nipples: a randomized comparative study. J Hum Lact. 1999;15:241-6. [PubMed: 10578803]
- 5.
- Dennis CL, Schottle N, Hodnett E, McQueen K. An all-purpose nipple ointment versus lanolin in treating painful damaged nipples in breastfeeding women: A randomized controlled trial. Breastfeed Med. 2012. [PubMed: 22428572]
Substance Identification
Substance Name
Mupirocin
CAS Registry Number
12650-69-0
Drug Class
- Breast Feeding
- Lactation
- Anti-Infective Agents, Local
- Antibacterial Agents
Disclaimer: Information presented in this database is not meant as a substitute for professional judgment. You should consult your healthcare provider for breastfeeding advice related to your particular situation. The U.S. government does not warrant or assume any liability or responsibility for the accuracy or completeness of the information on this Site.
Publication Details
Publication History
Last Revision: October 31, 2018.
Copyright
Attribution Statement: LactMed is a registered trademark of the U.S. Department of Health and Human Services.
Publisher
National Institute of Child Health and Human Development, Bethesda (MD)
NLM Citation
Drugs and Lactation Database (LactMed®) [Internet]. Bethesda (MD): National Institute of Child Health and Human Development; 2006-. Mupirocin. [Updated 2018 Oct 31].