Attribution Statement: LactMed is a registered trademark of the U.S. Department of Health and Human Services.
NCBI Bookshelf. A service of the National Library of Medicine, National Institutes of Health.
Drugs and Lactation Database (LactMed®) [Internet]. Bethesda (MD): National Institute of Child Health and Human Development; 2006-.
CASRN: 52-01-7
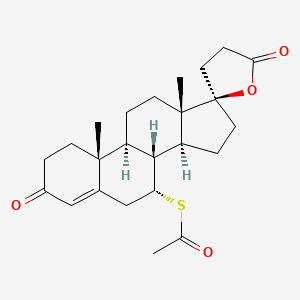
Drug Levels and Effects
Summary of Use during Lactation
Limited data indicate that spironolactone is poorly excreted into breastmilk. Case of mothers breastfeeding during spironolactone therapy reported no adverse effects in infants. Spironolactone appears to be acceptable to use during breastfeeding.
Drug Levels
Maternal Levels. The major metabolite of spironolactone, canrenone, was measured in the serum and milk of a 17-day postpartum woman who was taking 25 mg of spironolactone four times daily. Milk canrenone levels 2 hours after the dose were 104 mcg/L, and 47 mcg/L at 14.5 hours after the dose. The authors estimated that the nursing infant would receive about 0.2% of the mother's total daily dosage in the form of canrenone.[1] Active sulfur-containing metabolites were not measured.
Infant Levels. Relevant published information was not found as of the revision date.
Effects in Breastfed Infants
In 17-day-old breastfed (extent not stated) infant whose mother was taking 25 mg of spironolactone 4 times daily since pregnancy, serum sodium and potassium remained normal.[1]
Spironolactone 75 mg every other day was taken orally by a mother while nursing a newborn. She was also taking 400 mg of bretylium tosylate every 8 hours, atenolol 25 mg daily, propranolol 20 mg 3 times a day, and multivitamin, potassium and magnesium supplements. Jaundice, thought to be unrelated to the drug, occurred at 60 hours of age, but resolved. The infant had appropriate weight gain and development during the first 4 months of life.[2]
A transgender woman took and spironolactone 50 mg twice daily to suppress testosterone, domperidone 10 mg three times daily, increasing to 20 mg four times daily, oral micronized progesterone 200 mg daily and oral estradiol to 8 mg daily and pumped her breasts 6 times daily to induce lactation. After 3 months of treatment, estradiol regimen was changed to a 0.025 mg daily patch and the progesterone dose was lowered to 100 mg daily. Two weeks later, she began exclusively breastfeeding the newborn of her partner. Breastfeeding was exclusive for 6 weeks, during which the infant's growth, development and bowel habits were normal. The patient continued to partially breastfeed the infant for at least 6 months.[3]
A woman with Gitleman syndrome took spironolactone in an unspecified dosage along with potassium and magnesium supplements for at least 4 months while breastfeeding her infant. No adverse infant effects were reported.[4]
Effects on Lactation and Breastmilk
Intense diuresis can suppress lactation;[5,6] however, it is unlikely that spironolactone alone is sufficiently potent to cause this effect.
Spironolactone can cause gynecomastia. The estimated risk is 52 cases per 1000 patients treated, which is 8.4 times the baseline risk.[7]
A transgender woman was taking sublingual estradiol 4 mg twice daily, spironolactone 100 mg twice daily and progesterone 200 mg at bedtime for gender-affirming therapy. In order to prepare for the birth of the infant being carried by her partner, sublingual estradiol was increased to 6 mg twice daily and progesterone was increased to 400 mg at bedtime. Domperidone 10 mg twice daily was also started to increase serum prolactin levels and later increased to 20 mg 4 times daily. Before the delivery date, progesterone was stopped, spironolactone was decreased to 100 mg daily and estradiol was changed to 25 mcg per day transdermally. At day 59 postpartum, estradiol was changed to 2 mg per day sublingually and spironolactone was increased to 100 mg twice daily. The patient was able to produce up to 240 mL of milk daily containing typical macronutrient and oligosaccharide levels.[8]
References
- 1.
- Phelps DL, Karim A. Spironolactone: Relationship between concentrations of dethioacetylated metabolite in human serum and milk. J Pharm Sci 1977;66:1203. [PubMed: 894512]
- 2.
- Gutgesell M, Overholt E, Boyle R. Oral bretylium tosylate use during pregnancy and subsequent breastfeeding: A case report. Am J Perinatol 1990;7:144-5. [PubMed: 2331276]
- 3.
- Reisman T, Goldstein Z. Case report: Induced lactation in a transgender woman. Transgend Health 2018;3:24-6. [PMC free article: PMC5779241] [PubMed: 29372185]
- 4.
- de Jong MFC, Riphagen IJ, Kootstra-Ros JE, Groenewout M. Potassium and magnesium in breast milk of a woman with Gitelman syndrome. Kidney Int Rep 2022;7:1720-1. [PMC free article: PMC9263202] [PubMed: 35812288]
- 5.
- Healy M. Suppressing lactation with oral diuretics. Lancet 1961;277:1353-4.
- 6.
- Cominos DC, Van Der Walt A, Van Rooyen AJ. Suppression of postpartum lactation with furosemide. S Afr Med J 1976;50:251-2. [PubMed: 3858]
- 7.
- Trinchieri A, Perletti G, Magri V, et al. Drug-induced gynecomastia: A systematic review and meta-analysis of randomized clinical trials. Arch Ital Urol Androl 2021;93:489-96. [PubMed: 34933535]
- 8.
- Delgado D, Stellwagen L, McCune S, et al. Experience of induced lactation in a transgender woman: Analysis of human milk and a suggested protocol. Breastfeed Med 2023;18:888-93. [PubMed: 37910800]
Substance Identification
Substance Name
Spironolactone
CAS Registry Number
52-01-7
Drug Class
Breast Feeding
Milk, Human
Antihypertensive Agents
Diuretics
Mineralocorticoid Receptor Antagonists
Disclaimer: Information presented in this database is not meant as a substitute for professional judgment. You should consult your healthcare provider for breastfeeding advice related to your particular situation. The U.S. government does not warrant or assume any liability or responsibility for the accuracy or completeness of the information on this Site.
- User and Medical Advice Disclaimer
- Drugs and Lactation Database (LactMed) - Record Format
- LactMed - Database Creation and Peer Review Process
- Fact Sheet. Drugs and Lactation Database (LactMed)
- Drugs and Lactation Database (LactMed) - Glossary
- LactMed Selected References
- Drugs and Lactation Database (LactMed) - About Dietary Supplements
- Breastfeeding Links
- PMCPubMed Central citations
- PubChem SubstanceRelated PubChem Substances
- PubMedLinks to PubMed
- Review Norethynodrel.[Drugs and Lactation Database (...]Review Norethynodrel.. Drugs and Lactation Database (LactMed®). 2006
- Review Norethindrone.[Drugs and Lactation Database (...]Review Norethindrone.. Drugs and Lactation Database (LactMed®). 2006
- Review Medroxyprogesterone Acetate.[Drugs and Lactation Database (...]Review Medroxyprogesterone Acetate.. Drugs and Lactation Database (LactMed®). 2006
- Review Eplerenone.[Drugs and Lactation Database (...]Review Eplerenone.. Drugs and Lactation Database (LactMed®). 2006
- Isolation and identification of novel impurities in spironolactone.[J Pharm Biomed Anal. 2006]Isolation and identification of novel impurities in spironolactone.Chen H, Wang YF, Yang ZD, Li YC. J Pharm Biomed Anal. 2006 Mar 18; 40(5):1263-7. Epub 2005 Oct 19.
- Spironolactone - Drugs and Lactation Database (LactMed®)Spironolactone - Drugs and Lactation Database (LactMed®)
- Unidentified soil organism R6-100 16S rRNA gene, partial sequenceUnidentified soil organism R6-100 16S rRNA gene, partial sequencegi|1381457|gb|U42927.1|USU42927Nucleotide
Your browsing activity is empty.
Activity recording is turned off.
See more...
