Attribution Statement: LactMed is a registered trademark of the U.S. Department of Health and Human Services.
NCBI Bookshelf. A service of the National Library of Medicine, National Institutes of Health.
Drugs and Lactation Database (LactMed®) [Internet]. Bethesda (MD): National Institute of Child Health and Human Development; 2006-.
CASRN: 51-52-5
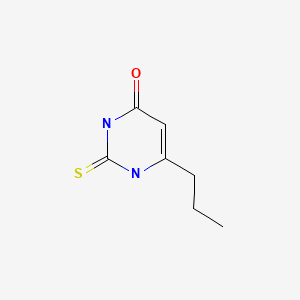
Drug Levels and Effects
Summary of Use during Lactation
Propylthiouracil (PTU) had been considered the antithyroid drug of choice during lactation;[1,2] however, findings that the rates of liver injury higher with PTU than with methimazole has altered this judgement. Some experts now recommend that methimazole should be considered the antithyroid drug of choice in nursing mothers.[3-5] No cases of PTU-induced liver damage have been reported in breastfed infants and it is unknown if the small amounts of the drug in breastmilk can cause liver damage. The drug or breastfeeding should be discontinued if liver toxicity is suspected. Dosages of PTU should be limited to 450 mg daily during breastfeeding.[6]
The American Thyroid Association recommends only monitoring infants for appropriate growth and development during routine pediatric health and wellness evaluations and routine assessment of serum thyroid function in the child is not recommended.[6] Rare idiosyncratic reactions (e.g., agranulocytosis) might occur, and the infant should be watched for signs of infection. Monitoring of the infant's complete blood count and differential is advisable if there is a suspicion of a drug-induced blood dyscrasia.
Drug Levels
Maternal Levels. A woman (time postpartum not stated) given a single dose of 100 mg of propylthiouracil (PTU) excreted a total of 0.077% of the dose in her breastmilk in 24 hours.[7]
After a single oral dose of 400 mg of propylthiouracil (PTU) in 9 women who were 1 to 9 months postpartum, peak milk levels averaging 0.7 mg/L were reached 1.5 hours after the dose. The authors estimated that the infant of a mother taking 200 mg 3 times a day would receive no more than 462 mcg daily or a maximum of 0.025% (range 0.07 to 0.077%) of the maternal dosage.[8]
Infant Levels. Relevant published information was not found as of the revision date.
Effects in Breastfed Infants
A mother was taking oral propylthiouracil 100 mg daily during pregnancy and 125 mg daily after delivery. In her infant, serum thyroxine (T4) concentration dropped slightly below the lower limit of normal on day 4 of life, but both T4 and thyrotropin (TSH) concentrations were normal on day 19 with continued maternal PTU therapy.[9] The drop in T4 was possibly due to propylthiouracil in breastmilk, but more likely from PTU received transplacentally.
An infant whose mother was taking propylthiouracil 200 to 300 mg daily was followed for 5 months and found to have normal thyroid function tests.[8]
A mother took PTU in a starting dose of 100 mg 3 times daily that was tapered to 50 mg twice daily over a period of 6 months. Her breastfed infant had normal thyroid function tests during this period at the ages of 9 to 13 months of age.[10]
Eight mothers taking PTU during pregnancy and doses of 50 to 300 mg daily after delivery exclusively or nearly exclusively breastfed their infants. The infants all had slightly low free T4 levels at birth and TSH levels were above normal in 7 of the 8, indicating that they had been affected by PTU in utero. All of their infants had normal free T4 and TSH levels when measured between 18 days and 8 months of age and none had any adverse effects reported from PTU in milk.[11]
The mothers of 11 fully breastfed infants were taking 300 to 750 mg daily of PTU starting at various times between delivery and 11 months postpartum. One infant had slightly elevated TSH level at 19 weeks of age when his mother was taking PTU 450 mg daily. Two other infants had elevated TSH levels at birth. TSH normalized in both infants with maternal PTU doses of 600 mg daily in one and a dose starting at 300 mg daily at term and increasing to 600 mg daily in the other.[12]
Two other infants were reported to be hypothyroid at birth, but to have normal thyroid function at 1 month of age despite maternal PTU therapy during breastfeeding.[13]
Effects on Lactation and Breastmilk
Relevant published information was not found as of the revision date.
References
- 1.
- Cooper DS. Antithyroid drugs: To breast-feed or not to breast-feed. Am J Obstet Gynecol 1987;157:234-5 [PubMed: 2441601]
- 2.
- Mandel SJ, Cooper DS. The use of antithyroid drugs in pregnancy and lactation. J Clin Endocrinol Metab 2001;86:2354-9 [PubMed: 11397822]
- 3.
- Karras S, Tzotzas T, Krassas GE. Antithyroid drugs used in the treatment of hyperthyroidism during breast feeding. An update and new perspectives. Hormones (Athens) 2009;8:254-7 [PubMed: 20058397]
- 4.
- Hudzik B, Zubelewicz-Szkodzinska B. Anti-thyroid drugs during breastfeeding. Clin Endocrinol (Oxf) 2016;85:827-30 [PubMed: 27561657]
- 5.
- Amino N, Arata N. Thyroid dysfunction following pregnancy and implications for breastfeeding. Best Pract Res Clin Endocrinol Metab 2020;34:101438 [PubMed: 32651061]
- 6.
- Alexander EK, Pearce EN, Brent GA, et al. 2017 Guidelines of the American Thyroid Association for the diagnosis and management of thyroid disease during pregnancy and the postpartum. Thyroid 2017;27:315-89 [PubMed: 28056690]
- 7.
- Low LC, Lang J, Alexander WD. Excretion of carbimazole and propylthiouracil in breast milk. Lancet 1979;314:1011 [PubMed: 91730]
- 8.
- Kampmann JP, Johansen K, Hansen JM, et al. Propylthiouracil in human milk: Revision of a dogma. Lancet 1980;1 (8171):736-7 [PubMed: 6103158]
- 9.
- Lamberg BA, Ikonen E, Osterlund K, et al. Antithyroid treatment of maternal hyperthroidism during lactation. Clin Endocrinol (Oxf) 1984;21:81-7 [PubMed: 6744638]
- 10.
- McDougall IR, Bayer MF. Should a woman taking propylthiouracil breast-feed? Clin Nucl Med 1986;11:249-50 [PubMed: 3754191]
- 11.
- Momotani N, Yamashita R, Yoshimoto M, et al. Recovery from foetal hypothyroidism: Evidence for the safety of breast-feeding while taking propylthiouracil. Clin Endocrinol (Oxf) 1989;31:591-5 [PubMed: 2627753]
- 12.
- Momotani N, Yamashita R, Makino F, et al. Thyroid function in wholly breast-feeding infants whose mothers take high doses of propylthiouracil. Clin Endocrinol (Oxf) 2000;53:177-81 [PubMed: 10931098]
- 13.
- Lee A, Moretti ME, Collantes A, et al. Choice of breastfeeding and physicians' advice: A cohort study of women receiving propylthiouracil. Pediatrics 2000;106:27-30 [PubMed: 10878145]
Substance Identification
Substance Name
Propylthiouracil
CAS Registry Number
51-52-5
Disclaimer: Information presented in this database is not meant as a substitute for professional judgment. You should consult your healthcare provider for breastfeeding advice related to your particular situation. The U.S. government does not warrant or assume any liability or responsibility for the accuracy or completeness of the information on this Site.
- User and Medical Advice Disclaimer
- Drugs and Lactation Database (LactMed) - Record Format
- LactMed - Database Creation and Peer Review Process
- Fact Sheet. Drugs and Lactation Database (LactMed)
- Drugs and Lactation Database (LactMed) - Glossary
- LactMed Selected References
- Drugs and Lactation Database (LactMed) - About Dietary Supplements
- Breastfeeding Links
- PubChem SubstanceRelated PubChem Substances
- PubMedLinks to PubMed
- Review Methimazole.[Drugs and Lactation Database (...]Review Methimazole.. Drugs and Lactation Database (LactMed®). 2006
- Review Carbimazole.[Drugs and Lactation Database (...]Review Carbimazole.. Drugs and Lactation Database (LactMed®). 2006
- Review Fluorouracil.[Drugs and Lactation Database (...]Review Fluorouracil.. Drugs and Lactation Database (LactMed®). 2006
- Review Mercaptopurine.[Drugs and Lactation Database (...]Review Mercaptopurine.. Drugs and Lactation Database (LactMed®). 2006
- Review Chloramphenicol.[Drugs and Lactation Database (...]Review Chloramphenicol.. Drugs and Lactation Database (LactMed®). 2006
- Propylthiouracil - Drugs and Lactation Database (LactMed®)Propylthiouracil - Drugs and Lactation Database (LactMed®)
Your browsing activity is empty.
Activity recording is turned off.
See more...
