Attribution Statement: LactMed is a registered trademark of the U.S. Department of Health and Human Services.
NCBI Bookshelf. A service of the National Library of Medicine, National Institutes of Health.
Drugs and Lactation Database (LactMed®) [Internet]. Bethesda (MD): National Institute of Child Health and Human Development; 2006-.
CASRN: 41575-94-4
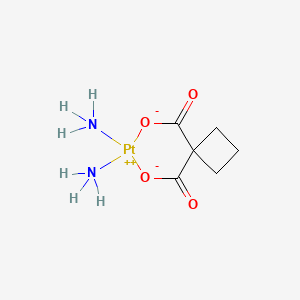
Drug Levels and Effects
Summary of Use during Lactation
Most sources consider that mothers receiving antineoplastic therapy should not breastfeed, especially with alkylating agents such as carboplatin.[1] It might be possible to breastfeed safely during intermittent therapy with an appropriate period of breastfeeding abstinence, but the duration of abstinence is not clear. Platinum in milk may increase with repeated courses of chemotherapy and the exact form(s), and toxicity of platinum excreted into breastmilk are also not known. The nursing infant would receive platinum compounds orally rather than intravenously and oral absorption of platinum compounds by infants is not known. It appears that it is not safe to breastfeed after carboplatin chemotherapy, and breastfeeding should probably be discontinued.
Chemotherapy may adversely affect the normal microbiome and chemical makeup of breastmilk.[2] Women who receive chemotherapy during pregnancy are more likely to have difficulty nursing their infant.[3]
Drug Levels
Maternal Levels. A woman with a history of treatment for thyroid cancer and recurrence during pregnancy was treated postpartum with carboplatin and paclitaxel. Her intravenous carboplatin dose was 233 mg (2.9 mg/kg; AUC 1.5) weekly for 6 weeks. Whole milk samples were obtained at 4, 28, 172, and 316 hours after the dose. The highest milk carboplatin level was 0.9 mg/L in the 4-hour sample and carboplatin was still measurable (0.16 mg/L) in the 317 hour sample. Metabolites were not measured. The authors calculated an average milk carboplatin level over the 316 hour collection period of 0.4 mg/L, resulting in an estimated total infant weight-adjusted daily dose of 2% of the maternal weekly dose.[4] Note that the above estimate of an infant daily dose is expressed as percentage of the maternal weekly dose, and that the authors used a level of zero as the trough milk level, rather than a milk level taken before the sixth dose (which would equal approximately the 172-hour level of 0.25 mg/L), resulting in an underestimate of the AUC and infant dose.
A woman with breast cancer diagnosed during pregnancy received chemotherapy beginning a few days after delivery. It consisted of doxorubicin 118 mg and cyclophosphamide 1180 mg every 2 weeks for 4 cycles, followed by paclitaxel 156 mg weekly and carboplatin 900 mg every 4 weeks. She collected 97 milk samples; a selection of 78 samples were analyzed for carboplatin. Reported carboplatin concentrations in the milk samples were calculated based on the measured platinum concentrations using the molecular weight of carboplatin with the assumption that all measured platinum was carboplatin. Peak levels ranged from 160 mcg/L to 350 mcg/L. Milk levels dropped rapidly to less than 100 mcg/L by 2 days after the dose. Platinum levels plateaued after several days at levels between 10 and 50 mcg/L that appeared to increase with repeated cycles of chemotherapy. The authors calculated the times for the milk concentrations to reach various relative infant dosage (RID) levels. It took less than 1 day to fall below an RID of 1%; however, the actual platinum species in milk were not determined.[5]
Infant Levels. Relevant published information was not found as of the revision date.
Effects in Breastfed Infants
Relevant published information was not found as of the revision date.
Effects on Lactation and Breastmilk
A telephone follow-up study was conducted on 74 women who received cancer chemotherapy at one center during the second or third trimester of pregnancy to determine if they were successful at breastfeeding postpartum. Only 34% of the women were able to exclusively breastfeed their infants, and 66% of the women reported experiencing breastfeeding difficulties. This was in comparison to a 91% breastfeeding success rate in 22 other mothers diagnosed during pregnancy, but not treated with chemotherapy. Other statistically significant correlations included: 1. mothers with breastfeeding difficulties had an average of 5.5 cycles of chemotherapy compared with 3.8 cycles among mothers who had no difficulties; and 2. mothers with breastfeeding difficulties received their first cycle of chemotherapy on average 3.4 weeks earlier in pregnancy. Of the 3 women who received a regimen containing the similar drug, cisplatin, 1 had breastfeeding difficulties.[3]
References
- 1.
- Pistilli B, Bellettini G, Giovannetti E, et al. Chemotherapy, targeted agents, antiemetics and growth-factors in human milk: How should we counsel cancer patients about breastfeeding? Cancer Treat Rev. 2013;39:207–11. [PubMed: 23199900]
- 2.
- Urbaniak C, McMillan A, Angelini M, et al. Effect of chemotherapy on the microbiota and metabolome of human milk, a case report. Microbiome. 2014;2:24. [PMC free article: PMC4109383] [PubMed: 25061513]
- 3.
- Stopenski S, Aslam A, Zhang X, et al. After chemotherapy treatment for maternal cancer during pregnancy, is breastfeeding possible? Breastfeed Med. 2017;12:91–7. [PubMed: 28170295]
- 4.
- Griffin SJ, Milla M, Baker TE, et al. Transfer of carboplatin and paclitaxel into breast milk. J Hum Lact. 2012;28:457–9. [PubMed: 23087196]
- 5.
- Damoiseaux D, Calpe S, Rosing H, et al. Presence of 5 chemotherapeutic drugs in breast milk as a guide for the safe use of chemotherapy during breastfeeding: Results from a case series. Clin Pharmacol Ther. 2022;112:404–10. [PubMed: 35486426]
Substance Identification
Substance Name
Carboplatin
CAS Registry Number
41575-94-4
Disclaimer: Information presented in this database is not meant as a substitute for professional judgment. You should consult your healthcare provider for breastfeeding advice related to your particular situation. The U.S. government does not warrant or assume any liability or responsibility for the accuracy or completeness of the information on this Site.
- User and Medical Advice Disclaimer
- Drugs and Lactation Database (LactMed) - Record Format
- LactMed - Database Creation and Peer Review Process
- Fact Sheet. Drugs and Lactation Database (LactMed)
- Drugs and Lactation Database (LactMed) - Glossary
- LactMed Selected References
- Drugs and Lactation Database (LactMed) - About Dietary Supplements
- Breastfeeding Links
- PMCPubMed Central citations
- PubChem SubstanceRelated PubChem Substances
- PubMedLinks to PubMed
- Review Cisplatin.[Drugs and Lactation Database (...]Review Cisplatin.. Drugs and Lactation Database (LactMed®). 2006
- Review Oxaliplatin.[Drugs and Lactation Database (...]Review Oxaliplatin.. Drugs and Lactation Database (LactMed®). 2006
- Review Dacarbazine.[Drugs and Lactation Database (...]Review Dacarbazine.. Drugs and Lactation Database (LactMed®). 2006
- Review Gemcitabine.[Drugs and Lactation Database (...]Review Gemcitabine.. Drugs and Lactation Database (LactMed®). 2006
- Review Bleomycin.[Drugs and Lactation Database (...]Review Bleomycin.. Drugs and Lactation Database (LactMed®). 2006
- Carboplatin - Drugs and Lactation Database (LactMed®)Carboplatin - Drugs and Lactation Database (LactMed®)
Your browsing activity is empty.
Activity recording is turned off.
See more...
