Burden of Disease
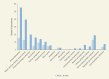
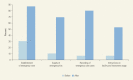
Burn injuries are among the most devastating of all injuries and a major global public health concern (Forjuoh 2006). Each year, more than 265,000 people die from fire-related burn injuries. Millions more suffer from burn-related disabilities and disfigurements, which have psychological, social, and economic effects on the survivors and their families. Fire-related burns account for 17 million DALYs lost worldwide annually (WHO 2013b). Strikingly, fires rank third worldwide for DALYs lost because of unintentional injury in Sub-Saharan Africa, second in Eastern Mediterranean and South-East Asian countries, and fifth in HICs.
Burn is a disease of poverty; the burden of burn injury falls predominantly on the world’s poor, with 95 percent of fire-related burn deaths occurring in LMICs. Not only are burn deaths and injuries more common in people of lower socioeconomic status, but the survivors find that their poverty levels worsen after recovery (Peck, Molnar, and Swart 2009). The high incidence of burns in this population is driven by negative impact factors, including the influx of people to urban areas, haphazard urban development, inadequate electrification of homes, paraffin used as a primary energy source, and lack of preventive programs.
The worldwide incidence of death from fire-related injuries in 2004 was estimated to be 3.8 per 100,000 population, with the highest rates in Southeast Asia and Sub-Saharan Africa. The incidence of burns in LMICs is 4.4 per 100,000 population, compared with an incidence of 0.84 per 100,000 population in HICs (WHO 2013b). In Bangladesh, the incidence of nonfatal burn injury is 166.3 per 100,000 per year (Mashreky and others 2009).
In addition, the epidemiology of burn injuries is also different in LMICs, where it is predominantly a pediatric and geriatric disease (Ahuja and Bhattacharya 2002). Children, especially those under age five, have been shown to constitute the highest risk group of burn victims, followed by those ages 20–29. Of the studies that reported data on childhood burns, children under age four had a disproportionately higher number of burns; they accounted for nearly one-third of the total number of burn cases, all age groups considered. In many settings, including Brazil, Côte d’Ivoire, India, and Malawi, this age group accounts for nearly half of all childhood burns (Forjuoh 2006).
Burn centers are usually part of large urban hospitals and act as referral centers for patients from smaller first-level hospitals and health centers. Burn units are dedicated units within hospital structures that manage care for patients of all ages; burn units typically have dedicated nurses and staff. In LMICs, most existing burn centers are situated in large cities and are insufficient for the high incidence of injuries. Although management in these centers is based primarily on standard principles, hospitals are ill-equipped with staff and support facilities. In addition to inadequate physical structures, these centers are invariably plagued by lack of resources, lack of operating time, and shortages of blood. Often, no dedicated burn surgeons are available; general surgeons without formal burn training are involved in burn care. Burn nursing is also not a recognized concept. Resuscitation is often delayed because patients have to travel long distances and transport facilities are poor. Ambulance and prehospital services are practically nonexistent (Atiyeh, Masellis, and Conte 2009). Furthermore, coordination between first-level hospitals and third-level burn centers is limited.
Cost-Effectiveness of Burn Care
Burn care requires a significant number of dedicated expert personnel and is resource intensive. When choosing between different treatment options, the available funds, personnel, and required expertise must be weighed. Reliable information relating costs to clinical outcomes is needed. Burn-care costs have been the subject of very few investigations and are among the least studied topics by health services researchers, particularly in LMICs (Atiyeh and others 2002). In a prospective study by Ahachi and others, the direct hospitalization cost of managing major acute burns in Lagos, Nigeria, was examined to identify the factors that influenced cost. The researchers found that the average daily cost of treating a burn patient was approximately US$6, and that the average overall cost for a burn admission was approximately US$62; the costs of wound dressings, hospital admission, and surgery constituted 29.5 percent, 25.7 percent, and 19.1 percent, respectively, of the total amount spent (Ahachi and others 2011). In a similar study in Bangladesh, the average cost for serious and major burns was US$166 and US$58 per burn injury, respectively. For the treatment of a severe burn, a family spent an average of US$462 (Mashreky and others 2009).
Prehospital care of burn victims using simple measures, such as irrigation with clean cool water and clean dressings, is of particular importance where access to hospital care is commonly delayed. Prehospital care is discussed at greater length in chapter 14.
Cost-Effectiveness of Hospital Management
Although very little literature exists on the effectiveness of burn centers compared with smaller local burn units, data suggest that the early burn excision frequently done in burn centers improves the survival of patients (Church and others 2006). Patients with burns exceeding 90 percent of total body surface area (TBSA) regularly survive in the world’s best centers; this rate is in stark contrast to the mortality for burns exceeding 40 percent of TBSA in most LMICs, which approaches 100 percent (WHO 2002b). Cost-effective burn treatment to conserve scarce resources includes emphasizing early fluid resuscitation and ensuring proper compliance with established resuscitation protocols, such as the Parkland formula.
Increasingly aggressive surgical approaches, with early tangential excision and wound closure, are standard practice in burn units in HICs. Such approaches likely represent the most significant change in recent years and have led to improvements in mortality rates of burn victims at substantially lower costs than waiting for the eschar—the dead burned skin that forms a scab over the burned area—to peel off. In the absence of proper burn-care facilities, blood supply, and other resources such as dressings, and with inadequately trained personnel, such aggressive therapy in burn victims can induce further trauma and result in suboptimal outcomes (Munster, Smith-Meek, and Sharkey 1994). Smaller burns over critical areas such as joints are better suited to this technique (WHO 2011). However, for a large percentage of patients with extensive burns in most LMICs, early excisional surgery is not available.
Triage. With the realities of inadequate access to surgical facilities in the LMIC environment, closed burn wound dressing, eschar separation, and delayed skin grafting will help to separate patients with less extensive injuries (less than 40 percent of TBSA) with the potential to survive from those patients with extensive wounds exceeding 50 percent of TBSA with poor survival who should be triaged to palliative care (Ahuja and Bhattacharya 2004).
Wound Care. Local wound care in developing countries is one of the greatest barriers to effective burn wound management; wound-care products and dressing supplies are not easily obtainable or are too expensive. Cool running water at a temperature between 10 and 15 degrees centigrade for 20–30 minutes is considered adequate burn first aid treatment (Skinner and Peat 2002). In one study of burn treatment in LMICs that included all countries in Latin America and the Caribbean, the Middle East and North Africa, and Sub-Saharan Africa, plus China, India, and other countries in Asia and adjoining islands, cool water was applied to the burned area as a first aid therapy in one-third of the cases, a ratio comparable to that observed in some HICs (Forjuoh 2006). Silver-based dressing and ointment should be used, if available. However, the use of locally available and effective wound-care alternatives, amniotic membrane in particular, is cost-effective and ideal as a biological dressing. Amniotic membrane remarkably reduces the cost of dressing changes and the periods of stay in hospitals. It also significantly reduces nursing time and thereby nursing costs (Atiyeh, Gunn, and Hayek 2005). It is often in ample supply if the facility has a busy obstetrics department. However, other considerations, such as cultural acceptability or the risk of HIV or hepatitis infections, also need to be considered.
The medicinal properties of honey and other hive products have been well described for a variety of medicinal and nutritional purposes, including the treatment of burn wounds. The beneficial effects of honey include the cleansing of wounds, absorption of edema fluids, antimicrobial activity, promotion of granulation tissue, epithelialization, and the improvement of nutrition. Another cost-effective, locally available burn dressing is the banana leaf dressing (BLD). Its preparation is very simple: a banana leaf is washed, pasted to bandage cloth with flour paste, dried for 24 hours, rolled, packed into a paper bag, and autoclaved. This process can be easily taught to previously treated patients, relatives of patients, and literate as well as illiterate individuals. Banana leaves are readily available in most cities, towns, and villages in LMICs. It is even possible to have a patch of land with a banana plantation within the hospital premises in a busy burn unit. BLD, being totally nonadherent, tends to slip. BLD is 160 times cheaper than Soframycin-impregnated gauze, 1,750 times cheaper than collagen sheet, and 5,200 times cheaper than biosynthetic dressing (Atiyeh, Masellis, and Conte 2009). More recently, moist exposed burn ointment (MEBO), a traditional Chinese burn remedy, was reported to provide an adequate moist environment for optimal healing without the need for a cumbersome and expensive protective dressing. Its main active component is beta-sitosterol in a base of beeswax and sesame oil. MEBO has been found to be a useful alternative in the treatment of partial-thickness burns because of its convenient method of application; it could be a valuable treatment modality in LMICs (Atiyeh and others 2003).
Exposure therapy is often the method of choice because gauze dressings are considered expensive. The exposure method is particularly suitable for the treatment of pediatric burn injuries, especially in a tropical climate where patients are nursed under mosquito nets to keep flies and other insects away from open burn wounds. In an observational study by Gosselin and Kuppers comparing open and closed dressing in burn wounds, the open method had as good or better early outcomes than the closed method, at significantly lower cost; it is the recommended treatment for burns in environments similar to the one in this study (Gosselin and Kuppers 2008).
Pain Management. Pain management, particularly in children, is another factor that divides the developed from the developing world. Provision of pain relief in the face of limited resources and a limited spectrum of analgesics, if any are available, is a challenge. In a study of the patterns of pediatric analgesic use in Sub-Saharan Africa, paracetamol and ibuprofen were widely employed, constituting approximately 60 percent of all analgesics, while morphine was used in only 0.2 percent of cases. This falls short of the WHO standards (Madadi and others 2012).
Antibiotic Use. Because of the paucity of studies, whether the use of prophylactic systemic antibiotics is effective and cost-effective in preventing infective complications remains unclear; however, the available evidence does not support its use for prophylaxis (ICHRC 2013).
Adequate Nutrition. Healing a burn injury demands a great deal of energy from the body. Adequate nourishment, including adequate protein, calories, vitamins, and micronutrients, is essential to support healing. Some burn units have started to introduce “Plumpy’nut,” a high-protein and high-energy peanut-based food that is readily available as a nutritional supplement for malnourished children, to the burn nutrition regimen. A two-month Plumpy’nut regimen for a child costs US$60.
Rehabilitation. In addition to burn-related mortality, burn-related disabilities have substantial functional and economic impacts. Functional disability is defined in the Global Burden of Disease report as disability-adjusted life years (DALYs), or the number of years lost due to poor health, disability, or early death (Murray and Lopez 1996). Worldwide, burns covering more than 20 percent of TBSA rank first among injury types causing short- or long-term disability. The WHO estimates that 116 million people have suffered such burns—approximately four times the number of people with HIV/AIDS at 31 million people (WHO 2008).
Rehabilitation of burn patients must begin immediately after the injury; the delay between inpatient and outpatient therapy should be minimized to facilitate a quick return of functional patients to society (Takayanagi, Kawai, and Aoki 1999). Part of the rehabilitation process is the prevention and treatment of postburn scarring, the most common and frustrating complication because of its aesthetic and functional consequences (van den Kerckhove 2001). The lack of available personnel significantly limits inpatients and outpatient postburn rehabilitation. The ability to train family members in basic physical and occupational therapy skills, such as range of motion exercises, is a cost-effective way to reduce the extent of disabilities. Effective rehabilitation can minimize the need for reconstruction. Local surgeons, where available, need to be trained in basic plastic surgical techniques, such as contracture release (see chapter 13).
Burn prevention strategies are well recognized as being very cost-effective, more so than burn treatment (see chapter 20).
Future Developments in the Treatment of Burns
Mandatory reporting of burn admissions to a central registry can generate data invaluable for evaluating strategies and prevention programs. Optimizing the current information system is achievable by customizing coding developments already underway; combining data from the various agencies to form a national burn injury database will provide the best national overview of burns.
Large-scale awareness programs aimed at policy makers, politicians, professionals, the general public, and the media are required to communicate the burden, impact, and losses due to burn-related injuries. Recognizing that burns are a public health problem, and making burn prevention and management a national programmatic priority, can ensure that sufficient funds are available for such programs.
Telemedicine is an effective tool for accurately evaluating the condition of patients with burns. This tool can reduce undertriage or overtriage for transport, improve resource utilization, and enhance and extend burn center expertise to many rural communities at low cost (Saffle and others 2009). Data specific to burn assessment and diagnosis using telemedicine suggest that this is a safe, reliable, and cost-effective means to attain consultation from specialists for patients in underserved areas (Kiser and others 2013). As this technology has evolved, it has become only slightly more expensive than a standard computer with a high-speed Internet connection.