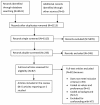
1. Randomized trials (1 study)
In Boston, USA, a randomized trial called the USHER study (Universal Screening for HIV Infection in the Emergency Room) compared two models of HTS provision in an emergency department setting: HTS by lay providers (trained HIV counselors) compared with HTS by regular emergency department healthcare providers (emergency service assistants) (2). In the lay provider arm, all activities were conducted by trained HIV counselors, from test consent to delivery of reactive or nonreactive test results and referral for confirmatory testing. In the healthcare provider arm, emergency service assistants (generally a 2-year college degree) offered and consented participants for HTS, collected the specimen, and developed the test in an on-site laboratory. Non-reactive results were shared with the client by resident physicians or physician assistants, while clients were told of reactive results by attending physicians who also requested consent for confirmatory testing. All HTS was conducted with the OraQuick® ADVANCE HIV-1/2 (OraSure Technologies, Inc. Bethlehem, PA, USA) HIV rapid diagnostic test using oral fluid. Both lay providers and emergency service assistants received the same 1-day OraQuick® HTS training and successfully completed the accompanying competency test. Lay providers completed the Massachusetts Department of Public Health HIV counsellor certification process; while emergency service assistants also watched a 90 minute training video led by the trial's principal investigator (the training video was optional for other trained healthcare providers responsible for delivery of test results in the lay provider arm of the trial). In the Cochrane risk of bias assessment, this study received a low or uncertain risk of bias across all measures except blinding of participants and personnel; participants, counsellors, and providers were not masked to the assigned study arms (as this would be difficult/impossible given the nature of the comparison), but neither were they incentivized in any way to complete the testing process.
Uptake of HTS among emergency department patients was 57% (1,382/2,446) in the lay provider arm compared with 27% in the healthcare provider arm (643/2,409; p<.001). Uptake of HTS was the only PICO outcome measured in this trial.
2. Pre/post studies (1 study)
One study examined HIV testing uptake before and after the use of lay providers for HTS (11). This study was conducted in Thyolo, a rural district of Malawi, and employed a number of different programmatic efforts to enable rapid scale-up of HIV care and treatment services, including task sharing to increase the number of health workers engaged in HIV care, as well as decentralization of care to health centers and community sites, simplification of protocols for testing and treatment; community engagement to increase capacity and support programme sustainability; and health system strengthening. HTS was delegated to health surveillance assistant (HSA) counsellors, who received a 10-week basic training to become HSAs and then an additional 3 weeks of training on HTS to become HTS counselors. Further details on the type of HIV testing were not provided.
After delegating HTS to lay providers (the HSAs in this model), uptake of testing increased from 1300 tests per month in 2003 to 6500 tests per month in 2009. This was the result of an increase from 14 HTS sites at the end of 2003 (with an average of 93 tests per month performed at each site) to 39 sites at the end of 2009 (with an average of 167 tests per site per month). While the study also reported numbers of patients initiated on ART, the additional changes in the health system described above seriously limited the ability to link these outcome changes with the changes in cadres providing HTS.
3. Quality comparison between lay providers and laboratory staff (3 studies)
Three studies conducted quality comparisons between lay providers and laboratory staff.
In Sisonke District, South Africa, the Good Start cluster randomized trial evaluated an integrated, scalable package delivered by community health workers to improve infant feeding and HIV-free infant survival (9). As part of the intervention arm of this trial, home-based HTS was conducted by lay providers. These lay providers completed a 10-day nationally accredited course in HTS, during which they learned how to conduct both of the rapid HIV tests used in the district protocol. They spent a further three months shadowing facility lay counsellors and gaining nurse-supervised testing experience at local health facilities. Additionally, they received one-day training on obtaining and packaging dried blood spot (DBS) samples from laboratory technicians. Testing was conducted using HIV rapid diagnostic tests (SD Bioline (Standard Diagnostics Inc., Kyonggi-do, South Korea) with confirmatory SENSA (Sensa Tri-line HIV 1/2/0; Hitech Healthcare Ltd, Beijing, China)) on finger prick blood samples. Additional dried blood spot samples from the same finger prick were also taken, and a sample of HIV-negative results (62.5%) and all HIV-positive, indeterminate and discordant-couple results were also sent for laboratory-based enzyme-linked immunosorbent assay (ELISA) testing. Study authors provided further details on the selection of samples sent for laboratory testing. All HIV positive and indeterminate samples were sent for laboratory testing. During the first few months of the study, all HIV-negative samples were sent for laboratory testing, and thereafter a systematic sample of HIV-negative specimens was sent for laboratory testing. Of 3986 matched samples, lay provider and laboratory results of HTS were concordant in all but 23 cases. Of these, further examination revealed only 2 cases that could be considered “critical errors” where the lay provider found a HIV positive result and the laboratory had a negative result; the rest were cases where at least one result was indeterminate, and most of these were considered cases of the lay provider being extra cautious. Overall, sensitivity was calculated as 98.0% (95% CI: 96.3- 98.9%) and specificity as 99.6% (95% CI: 99.4-99.7%).
In rural Karonga District, Malawi, the Karonga Prevention Study (KPhS) examined the quality of home-based rapid testing on venous whole-blood samples taken by lay providers (10). These lay providers were trained and certified by Ministry of Health staff to perform HIV counselling, whole-blood rapid testing and specimen collection by finger prick, using standard training procedures. HIV testing was conducted using an algorithm of Determine™ HIV-1/2 (Abbott Japan Co Ltd, Tokyo, Japan) with Uni-Gold™ HIV (Trinity Biotech PLC, Bray, Ireland) as the first and second rapid tests, respectively. If the test results were discordant SD Bioline HIV 1/2 3.0 (Standard Diagnostics Inc, Kyonggi-do, Korea) was used as a “tie-breaker”. Of 10819 samples, 2911 were sent to for laboratory quality control or confirmation based on quality control procedures of retesting all positive and every tenth negative specimen. Of these, lay provider and laboratory results were concordant in all but 4 cases, 3 of which were considered most likely the result of “sample peculiarities”. Results showed a sensitivity of 99.6% and specificity of 100.0%.
In Cambodia, a study compared results of rapid HIV testing by lay providers working in a prevention of mother-to-child transmission (PMTCT) site with results from laboratory technicians (13). Lay providers were trained HTS counsellors, who were midwives without any laboratory or phlebotomy experience. They received a half-day training on HTS and how to use Determine™ HIV1/2 (Abbott Japan Co Ltd, Tokyo, Japan) test kits using finger stick whole blood samples. Laboratory technicians routinely did the same test and returned the report of test results to lay providers. A total of 563 samples were tested by both lay providers and laboratory technicians; study authors confirmed that these were all blood samples from pregnant women who wanted to be tested for HIV during the study period. Of these 563 samples, lay provider and laboratory results of HTS were concordant in all but 4 cases. For these 4 cases, the authors report that, “Further investigation confirmed that all the reports by the counsellors were correct, and that human error in writing reports in the laboratory was a cause of these discordant reports”(13).